15 Abdominal Visual Changes That Prompt Further Diagnostic Investigation
The human abdomen serves as a remarkable diagnostic canvas, offering healthcare professionals and patients alike crucial visual clues about underlying pathological processes that may be occurring within the body's core systems. From subtle skin discolorations to dramatic distensions, abdominal visual changes represent one of the most accessible and immediate indicators of internal dysfunction, often preceding more severe symptoms by weeks or months. The complexity of abdominal anatomy, encompassing multiple organ systems including the gastrointestinal tract, hepatobiliary system, genitourinary apparatus, and vascular networks, means that surface manifestations can reflect a vast spectrum of conditions ranging from benign inflammatory processes to life-threatening malignancies. Modern medical practice emphasizes the critical importance of systematic visual assessment of the abdomen, as early recognition of these changes can significantly impact patient outcomes through timely intervention. This comprehensive exploration examines fifteen distinct abdominal visual alterations that should prompt immediate clinical investigation, providing healthcare professionals and informed patients with the knowledge necessary to recognize when surface changes demand deeper diagnostic scrutiny. Understanding these visual markers not only enhances clinical decision-making but also empowers individuals to seek appropriate medical attention when concerning changes arise, potentially preventing progression to more advanced disease states.
1. Abdominal Distension - Beyond Simple Bloating

Abdominal distension represents one of the most common yet potentially concerning visual changes that can indicate serious underlying pathology requiring immediate diagnostic evaluation. While many individuals experience temporary bloating from dietary indiscretions or gas accumulation, persistent or progressive abdominal enlargement warrants comprehensive investigation to rule out conditions such as ascites, bowel obstruction, organomegaly, or intra-abdominal masses. The pattern of distension provides crucial diagnostic clues: generalized enlargement may suggest fluid accumulation or gaseous distension, while localized bulging could indicate specific organ involvement or mass effect from tumors. Healthcare professionals must differentiate between physiological causes like pregnancy or obesity and pathological processes through careful history-taking and physical examination. Advanced imaging modalities including computed tomography and magnetic resonance imaging have revolutionized the evaluation of abdominal distension, allowing for precise identification of underlying causes and guiding appropriate therapeutic interventions. The temporal progression of distension also carries significant diagnostic weight, with acute onset suggesting emergent conditions like bowel obstruction or perforation, while gradual development over weeks to months may indicate chronic processes such as liver disease with ascites formation or slowly growing neoplasms. Recognition of associated symptoms such as pain, nausea, changes in bowel habits, or constitutional symptoms helps clinicians prioritize diagnostic workup and determine the urgency of intervention required.
2. Jaundice and Scleral Icterus - Hepatobiliary System Dysfunction

The development of jaundice, characterized by yellowish discoloration of the skin, mucous membranes, and sclera, represents a critical visual indicator of hepatobiliary dysfunction that demands immediate and thorough diagnostic investigation. This distinctive coloration results from elevated bilirubin levels in the blood, which can occur through three primary mechanisms: increased bilirubin production from excessive hemolysis, impaired hepatic processing due to liver disease, or obstruction of bile flow through the biliary system. The subtle onset of jaundice often begins with scleral icterus, where the whites of the eyes take on a yellowish hue before skin changes become apparent, making careful examination of the eyes crucial in early detection. Healthcare providers must systematically evaluate patients presenting with jaundice through comprehensive laboratory studies including complete blood count, comprehensive metabolic panel, liver function tests, and specific markers such as direct and indirect bilirubin levels, alkaline phosphatase, and gamma-glutamyl transferase. Advanced imaging studies including ultrasound, computed tomography, or magnetic resonance cholangiopancreatography may be necessary to identify structural abnormalities, stones, or masses within the hepatobiliary system. The clinical context surrounding jaundice development provides essential diagnostic information, with acute onset potentially indicating viral hepatitis, drug-induced liver injury, or biliary obstruction, while gradual progression might suggest chronic liver disease, malignancy, or inherited disorders of bilirubin metabolism. Early recognition and appropriate workup of jaundice can prevent progression to more severe complications and guide targeted therapeutic interventions.
3. Visible Peristalsis - Intestinal Obstruction Warning Signs
The visualization of peristaltic waves across the abdominal wall represents a dramatic and concerning physical finding that typically indicates significant intestinal obstruction requiring urgent medical evaluation and intervention. Under normal circumstances, intestinal contractions occur beneath the surface and are not visible through the abdominal wall, making their appearance a clear sign of pathological processes causing increased intraluminal pressure and compensatory muscular activity. This phenomenon most commonly manifests as wave-like movements that progress across the abdomen, often accompanied by high-pitched bowel sounds audible without a stethoscope, creating a clinical picture that demands immediate attention. The underlying pathophysiology involves the intestinal tract's attempt to overcome mechanical or functional obstruction through increased peristaltic activity, resulting in muscular contractions forceful enough to be visible through the abdominal wall. Healthcare professionals encountering visible peristalsis must rapidly assess for associated symptoms including severe cramping pain, nausea, vomiting, inability to pass gas or stool, and signs of dehydration or electrolyte imbalance that commonly accompany bowel obstruction. Diagnostic evaluation typically includes plain abdominal radiographs to identify dilated bowel loops, air-fluid levels, and the transition point of obstruction, followed by computed tomography imaging to determine the exact location, cause, and severity of the obstruction. The etiology of intestinal obstruction varies widely, encompassing adhesions from previous surgery, hernias, tumors, inflammatory bowel disease, or foreign body ingestion, each requiring specific therapeutic approaches ranging from conservative management to emergency surgical intervention. Prompt recognition of visible peristalsis and initiation of appropriate diagnostic workup can prevent progression to bowel ischemia, perforation, and life-threatening complications.
4. Abdominal Wall Hernias - Structural Integrity Compromise

Abdominal wall hernias manifest as visible protrusions or bulges that become apparent during increased intra-abdominal pressure, representing structural defects in the muscular and fascial layers that require careful evaluation to determine appropriate management strategies. These hernias can occur at various anatomical locations including the umbilical region, inguinal area, ventral abdominal wall, or at sites of previous surgical incisions, each presenting unique diagnostic and therapeutic challenges. The visual appearance of hernias typically involves a noticeable bulge that may increase in size with coughing, straining, or standing, and may reduce when the patient lies supine or applies gentle pressure to the area. Healthcare providers must distinguish between reducible hernias, where the protruding contents can be gently pushed back into the abdominal cavity, and incarcerated or strangulated hernias, which represent surgical emergencies due to compromised blood supply to the herniated tissues. The clinical evaluation of suspected hernias involves careful inspection of the entire abdominal wall, palpation to assess the size and consistency of the defect, and evaluation for signs of complications such as skin color changes, tenderness, or inability to reduce the hernia. Advanced imaging studies including ultrasound, computed tomography, or magnetic resonance imaging may be necessary to evaluate complex hernias, assess the contents of the hernia sac, or identify occult hernias not readily apparent on physical examination. The natural history of abdominal wall hernias involves progressive enlargement over time, with increasing risk of complications including incarceration, strangulation, and bowel obstruction, making early recognition and appropriate referral for surgical evaluation crucial for optimal patient outcomes.
5. Skin Discoloration Patterns - Vascular and Systemic Indicators

Abnormal skin discoloration patterns across the abdominal region can provide crucial diagnostic insights into underlying vascular, hematologic, or systemic conditions that require comprehensive medical evaluation and targeted therapeutic intervention. These color changes may manifest as erythema suggesting inflammatory processes or cellulitis, pallor indicating anemia or vascular compromise, cyanosis reflecting inadequate oxygenation, or various pigmentary alterations associated with metabolic or endocrine disorders. The distribution and characteristics of skin discoloration offer important clues about underlying pathophysiology, with localized changes potentially indicating regional processes such as infection or trauma, while generalized alterations may suggest systemic conditions affecting multiple organ systems. Healthcare professionals must carefully assess the temporal development of skin color changes, noting whether they appeared acutely or developed gradually over time, as this information helps differentiate between acute conditions requiring immediate intervention and chronic processes that may benefit from long-term management strategies. Specific patterns of abdominal skin discoloration carry particular diagnostic significance, such as the bluish periumbilical discoloration known as Cullen's sign, which may indicate retroperitoneal hemorrhage, or the flank discoloration termed Grey Turner's sign, suggesting bleeding into the retroperitoneal space. Laboratory studies including complete blood count, coagulation studies, liver function tests, and inflammatory markers help elucidate the underlying cause of skin discoloration and guide appropriate therapeutic interventions. Advanced imaging studies may be necessary to identify internal bleeding, organ dysfunction, or other pathological processes contributing to the observed skin changes, ensuring comprehensive evaluation and optimal patient care.
6. Venous Engorgement and Collateral Circulation - Portal Hypertension Signs
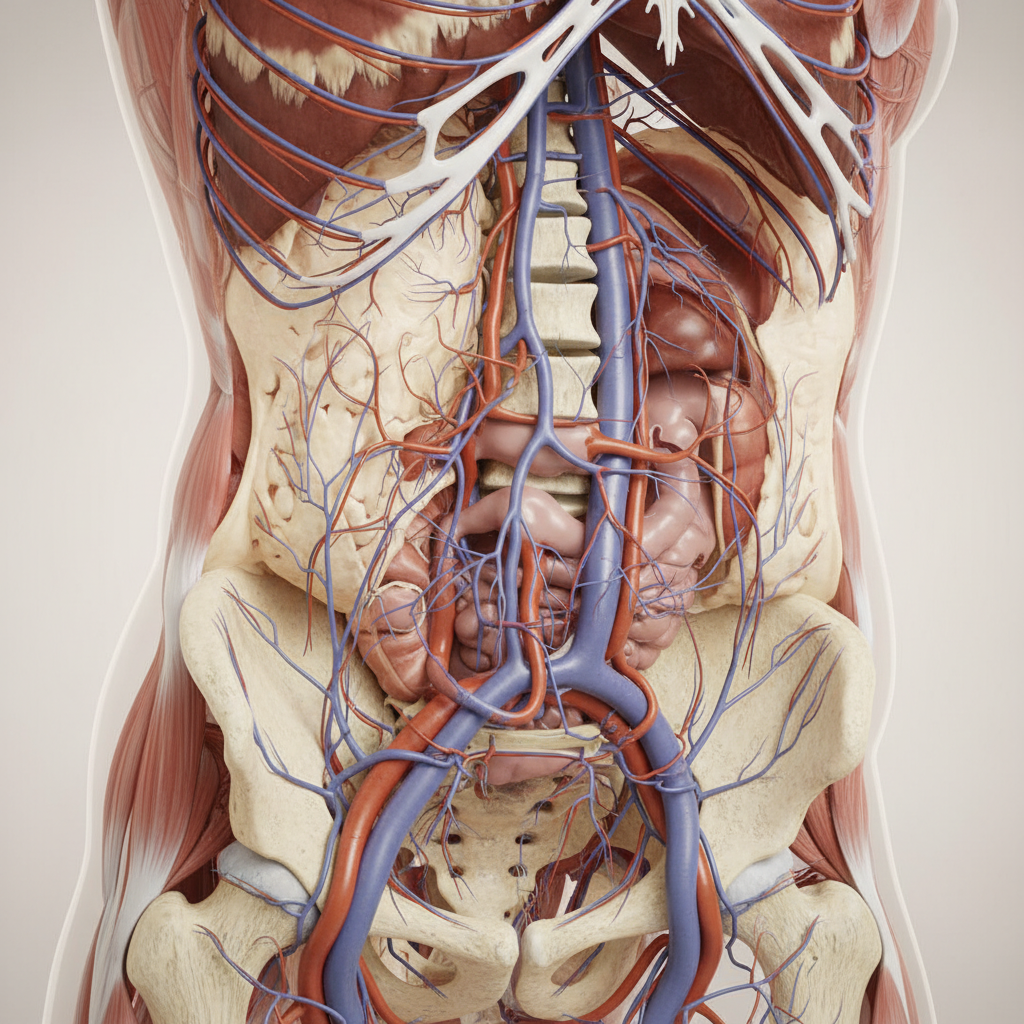
The development of prominent venous patterns across the abdominal wall, particularly the classic "caput medusae" appearance around the umbilicus, represents a critical visual indicator of portal hypertension and underlying liver disease that demands immediate diagnostic evaluation and management. This dramatic physical finding results from the formation of collateral circulation pathways as blood seeks alternative routes to return to the heart when normal portal venous flow is impeded by liver pathology or vascular obstruction. The engorged veins typically radiate outward from the umbilicus in a pattern reminiscent of Medusa's serpentine hair, creating an unmistakable clinical sign that experienced healthcare providers recognize as indicative of advanced liver disease or portal vein obstruction. The pathophysiology underlying venous engorgement involves increased pressure within the portal venous system, forcing blood to seek alternative drainage pathways through the systemic circulation via portosystemic anastomoses located at various anatomical sites including the gastroesophageal junction, rectum, and abdominal wall. Healthcare professionals encountering patients with prominent abdominal venous patterns must conduct comprehensive evaluation including detailed history-taking to identify risk factors for liver disease, physical examination to assess for other signs of portal hypertension such as splenomegaly or ascites, and laboratory studies to evaluate liver function and synthetic capacity. Advanced imaging modalities including Doppler ultrasound, computed tomography, or magnetic resonance imaging help assess portal venous anatomy, identify the underlying cause of portal hypertension, and evaluate for complications such as varices or thrombosis. The presence of collateral venous circulation indicates advanced disease with significant clinical implications, requiring multidisciplinary management involving hepatology, gastroenterology, and potentially surgical specialties to address both the underlying condition and its complications.
7. Abdominal Masses and Organomegaly - Palpable Abnormalities

The visual detection of abdominal masses or organ enlargement represents a concerning finding that necessitates systematic diagnostic evaluation to differentiate between benign and malignant processes, inflammatory conditions, and functional abnormalities affecting intra-abdominal organs. These abnormalities may present as localized bulges, asymmetric contours, or generalized abdominal enlargement that becomes apparent through careful visual inspection, particularly when patients are positioned supine with adequate lighting and exposure of the entire abdominal region. The location of visible masses provides important diagnostic clues, with right upper quadrant enlargement potentially indicating hepatomegaly, left upper quadrant fullness suggesting splenomegaly, and central or lower abdominal masses raising concern for gastrointestinal, genitourinary, or gynecologic pathology. Healthcare providers must employ systematic palpation techniques to characterize detected masses, assessing their size, consistency, mobility, and relationship to surrounding structures, while noting any associated tenderness or changes with respiration or positioning. The differential diagnosis for abdominal masses encompasses a broad spectrum of conditions including benign cysts, inflammatory masses, malignant tumors, organomegaly from various causes, and functional abnormalities such as distended bowel or bladder. Advanced imaging studies play a crucial role in the evaluation of abdominal masses, with ultrasound providing initial assessment of solid versus cystic nature, computed tomography offering detailed anatomical information and staging capabilities, and magnetic resonance imaging providing superior soft tissue characterization and multiplanar imaging capabilities. The clinical context surrounding mass detection, including patient age, gender, symptoms, and risk factors, helps guide appropriate diagnostic workup and determines the urgency of evaluation and potential need for tissue sampling or surgical intervention.
8. Surgical Scars and Wound Complications - Post-Operative Surveillance
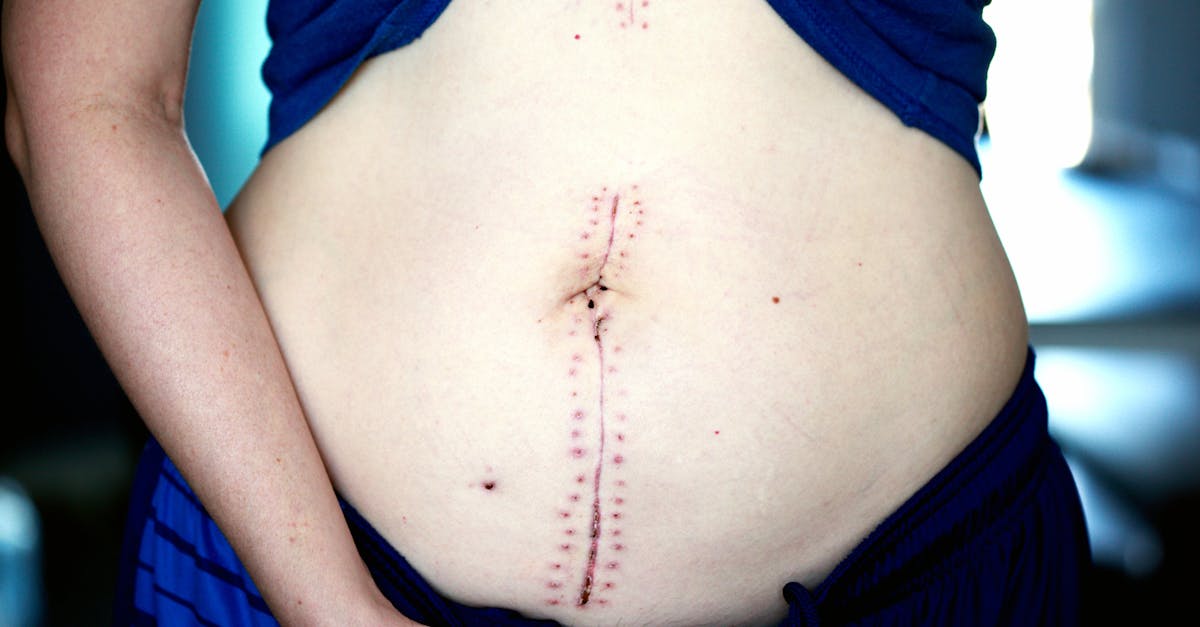
The appearance and evolution of surgical scars across the abdominal wall require ongoing surveillance to identify complications such as infection, dehiscence, hernia formation, or abnormal healing patterns that may necessitate additional medical or surgical intervention. Normal surgical scars undergo predictable healing phases, progressing from initial inflammatory response through proliferative tissue formation to final maturation and remodeling, with deviations from this expected pattern potentially indicating underlying complications or pathological processes. Healthcare professionals must carefully assess surgical incisions for signs of infection including erythema, warmth, swelling, purulent drainage, or spreading cellulitis, as these findings may indicate superficial or deep surgical site infections requiring antibiotic therapy or surgical drainage. The development of wound dehiscence, characterized by separation of tissue layers, represents a serious complication that may progress to complete fascial disruption and potential evisceration, requiring immediate surgical attention and repair. Long-term surveillance of abdominal surgical scars focuses on identifying incisional hernia formation, which can occur months to years after the initial procedure and may present as bulging or protrusion along the scar line, particularly with increased intra-abdominal pressure. Advanced imaging studies including ultrasound or computed tomography may be necessary to evaluate suspected complications, assess the integrity of fascial repair, or identify occult collections or abnormalities not readily apparent on physical examination. The management of surgical scar complications requires individualized approaches based on the specific nature of the problem, patient factors, and the urgency of intervention needed, ranging from conservative wound care and observation to complex surgical reconstruction and repair procedures.
9. Striae and Skin Texture Changes - Rapid Volume Alterations
The development of striae, commonly known as stretch marks, across the abdominal region can indicate rapid volume changes within the abdomen that may result from pathological processes requiring diagnostic investigation to identify underlying causes and appropriate management strategies. While striae commonly occur during pregnancy or significant weight gain, their appearance in other clinical contexts may suggest conditions such as ascites accumulation, intra-abdominal masses, Cushing's syndrome, or other endocrine disorders affecting tissue integrity and collagen synthesis. The characteristics of striae provide diagnostic information, with fresh lesions appearing red or purple due to underlying vascular changes, while older striae typically fade to white or silver as the inflammatory response resolves and tissue remodeling occurs. Healthcare providers must evaluate patients presenting with new or extensive striae through comprehensive history-taking to identify potential causes, physical examination to assess for associated findings, and appropriate laboratory studies to screen for endocrine abnormalities or other systemic conditions. The distribution pattern of striae offers additional diagnostic clues, with generalized involvement potentially suggesting systemic conditions like Cushing's syndrome or rapid weight changes, while localized patterns may indicate regional processes such as pregnancy or localized abdominal distension. Advanced evaluation may include hormonal studies to assess for hypercortisolism, imaging studies to evaluate for intra-abdominal pathology, or dermatologic consultation for complex cases involving extensive or atypical striae patterns. The clinical significance of striae extends beyond cosmetic concerns, as they may represent the earliest visible sign of underlying pathological processes that require prompt recognition and appropriate therapeutic intervention to prevent progression and complications.
10. Umbilical Changes and Abnormalities - Central Abdominal Indicators

The umbilical region serves as a crucial diagnostic landmark where various pathological processes can manifest through visible changes including protrusion, discoloration, discharge, or structural abnormalities that require systematic evaluation to identify underlying conditions and guide appropriate management. Umbilical hernias represent one of the most common abnormalities in this region, presenting as reducible or irreducible protrusions that may increase in size over time and carry risk of incarceration or strangulation, particularly in adults where spontaneous resolution is unlikely. The development of umbilical discharge, whether serous, purulent, or bloody, may indicate infection, retained foreign material, or underlying pathological processes such as urachal remnants or malignancy, requiring careful evaluation and appropriate diagnostic studies. Discoloration around the umbilicus can provide important diagnostic clues, with the bluish periumbilical discoloration known as Cullen's sign potentially indicating retroperitoneal hemorrhage from conditions such as acute pancreatitis, ruptured abdominal aortic aneurysm, or trauma. Healthcare professionals must carefully examine the umbilical region for signs of infection, structural abnormalities, or concerning changes that may indicate serious underlying pathology requiring immediate intervention. The evaluation of umbilical abnormalities may require imaging studies including ultrasound to assess for hernias or fluid collections, computed tomography for complex cases or suspected malignancy, or specialized studies such as fistulography if abnormal communications are suspected. The management of umbilical abnormalities varies widely depending on the underlying cause, ranging from conservative observation for small asymptomatic hernias to urgent surgical intervention for complicated cases or suspected malignancy, emphasizing the importance of accurate diagnosis and appropriate referral.
11. Abdominal Wall Muscle Definition Loss - Systemic Wasting Indicators
The loss of normal abdominal wall muscle definition and tone can serve as an important visual indicator of systemic wasting processes, malnutrition, or neuromuscular conditions that require comprehensive