12 Visible Vein Patterns and What They Can Indicate
# 12 Visible Vein Patterns and What They Can Indicate: A Comprehensive Guide to Understanding Your Vascular Health
Visible veins beneath the skin serve as a fascinating window into our circulatory system, offering valuable insights into our overall health and well-being. While many people view prominent veins as merely cosmetic concerns, these intricate patterns can actually reveal important information about circulation, hydration levels, genetic predispositions, and underlying medical conditions. The human vascular system consists of approximately 60,000 miles of blood vessels, with veins responsible for returning deoxygenated blood back to the heart. When these vessels become more prominent or exhibit unusual patterns, they're often communicating something significant about our body's internal state. From the delicate blue tracery visible on fair-skinned individuals to the more pronounced venous networks that appear with age or physical exertion, each pattern tells a unique story. Understanding these visible manifestations can empower individuals to make informed decisions about their health, recognize when medical consultation might be necessary, and appreciate the remarkable complexity of their circulatory system. This comprehensive exploration will examine twelve distinct vein patterns, their potential meanings, and what they might indicate about your vascular health, providing you with the knowledge to better understand your body's silent communications.
1. Spider Veins - The Delicate Web Pattern

Spider veins, medically known as telangiectasias, appear as fine, thread-like vessels that create intricate web-like patterns just beneath the skin's surface. These tiny dilated capillaries and venules typically measure less than one millimeter in diameter and commonly manifest in red, blue, or purple hues. Most frequently observed on the legs, thighs, and face, spider veins affect approximately 50-55% of women and 40-45% of men over the age of 50. While often considered a cosmetic concern, spider veins can indicate several underlying factors including hormonal fluctuations, particularly during pregnancy or menopause when estrogen levels change dramatically. They may also signal chronic venous insufficiency in its early stages, where the one-way valves in leg veins begin to weaken, causing blood to pool rather than efficiently return to the heart. Additional contributing factors include prolonged standing or sitting, genetic predisposition, sun exposure (particularly for facial spider veins), and certain medications that affect blood vessel dilation. Although spider veins rarely cause serious health complications, their appearance can serve as an early warning system for individuals to pay closer attention to their vascular health through lifestyle modifications, compression therapy, or medical evaluation when patterns become extensive or symptomatic.
2. Varicose Veins - The Twisted Highway

Varicose veins represent one of the most recognizable vein patterns, characterized by enlarged, twisted, and often bulging vessels that create a rope-like appearance beneath the skin. These dilated veins typically measure 3 millimeters or larger in diameter and most commonly affect the superficial veins of the legs and feet, though they can occur elsewhere on the body. The distinctive tortuous pattern develops when venous valves become incompetent, allowing blood to flow backward and pool within the vessel, causing progressive dilation and elongation. This condition affects approximately 23% of adults in the United States, with prevalence increasing significantly with age, reaching up to 60% in individuals over 60 years old. Varicose veins often indicate chronic venous insufficiency, a condition where the venous system struggles to efficiently return blood from the extremities back to the heart against gravity. Risk factors include family history, pregnancy, obesity, prolonged standing occupations, and age-related deterioration of vein walls and valves. Beyond their cosmetic impact, varicose veins can cause significant symptoms including aching, heaviness, cramping, swelling, and in severe cases, skin changes or ulceration. The pattern and severity of varicose veins can help healthcare providers assess the degree of venous insufficiency and determine appropriate treatment strategies, ranging from conservative management to minimally invasive procedures or surgical intervention.
3. Reticular Veins - The Feeder Network
Reticular veins, often called feeder veins, present as blue-green vessels that are larger than spider veins but smaller than varicose veins, typically measuring 1-3 millimeters in diameter. These veins create a distinctive net-like or branching pattern that often appears on the outer thigh, behind the knee, or on the inner calf. The term "reticular" derives from the Latin word "reticulum," meaning small net, which perfectly describes their characteristic appearance. These veins serve as an intermediate stage in the venous disease spectrum and often act as the source vessels that feed into spider vein networks. Their prominence can indicate developing venous insufficiency, particularly in the superficial venous system, and they frequently appear before more significant varicose veins develop. Reticular veins are commonly associated with hormonal changes, making them particularly prevalent during pregnancy, menopause, or with hormone replacement therapy. They may also indicate increased venous pressure in specific areas of the leg, often related to incompetent perforating veins that connect the superficial and deep venous systems. While reticular veins rarely cause significant symptoms, some individuals experience mild aching or burning sensations, particularly after prolonged standing. Their appearance serves as an important indicator for healthcare providers to assess overall venous health and potentially recommend preventive measures to slow the progression of venous disease. Treatment options range from sclerotherapy to laser therapy, depending on the size and extent of the affected vessels.
4. Bulging Hand and Arm Veins - The Upper Extremity Display
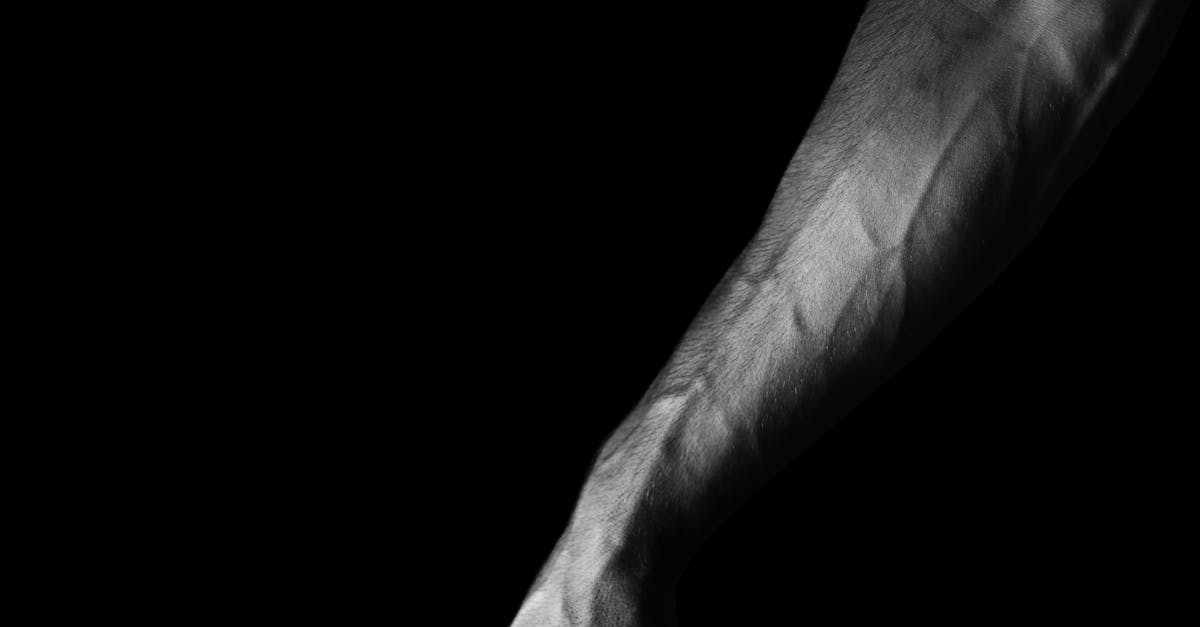
Prominent veins in the hands and arms create distinctive patterns that can indicate various physiological states and health conditions. Unlike lower extremity veins that work against gravity, arm veins benefit from gravitational assistance when the arms are lowered, making their prominence often more related to other factors. Normal hand and arm vein visibility typically increases with age as skin becomes thinner and subcutaneous fat decreases, making the underlying vascular network more apparent. However, sudden or dramatic changes in upper extremity vein patterns can signal important health developments. Dehydration commonly causes hand veins to become more prominent as blood volume decreases and vessels compensate by dilating. Conversely, excellent physical fitness and low body fat percentage can make arm veins more visible due to increased muscle mass and reduced subcutaneous tissue. Pathological causes of prominent arm veins include superior vena cava syndrome, where obstruction of the large vein returning blood from the upper body causes compensatory dilation of superficial veins. Thrombosis in deep arm veins can also cause superficial veins to become more prominent as they serve as collateral circulation routes. Additionally, certain occupations requiring repetitive arm movements or prolonged overhead positioning can lead to chronic venous dilation. Temperature changes significantly affect arm vein visibility, with heat causing vasodilation and cold causing vasoconstriction. Understanding these patterns helps distinguish between normal physiological variations and potentially concerning pathological changes that warrant medical evaluation.
5. Facial Vein Patterns - The Delicate Facial Network

Facial veins present unique patterns that differ significantly from those found elsewhere on the body due to the face's rich vascular supply and thin skin. The most common facial vein manifestations include periorbital veins around the eyes, nasal veins, and cheek telangiectasias, each with distinct characteristics and implications. Periorbital veins often appear as fine blue or purple lines around the eye area and can indicate several conditions including allergies, chronic eye rubbing, sun damage, or genetic predisposition to thin skin. These delicate vessels are particularly susceptible to damage from UV radiation, making sun protection crucial for prevention. Nasal veins frequently develop due to chronic inflammation from conditions like rosacea, rhinitis, or frequent nose blowing, creating characteristic spider-like patterns across the nose and surrounding areas. Facial telangiectasias can also result from hormonal changes, particularly during pregnancy when increased blood volume and hormonal fluctuations cause vessel dilation. Rosacea, a chronic inflammatory skin condition, often presents with persistent facial redness and visible blood vessels, particularly across the cheeks, nose, and forehead. Environmental factors such as extreme temperatures, wind exposure, spicy foods, alcohol consumption, and stress can exacerbate facial vein visibility. Unlike body veins that may indicate circulatory problems, facial veins are more commonly related to local skin conditions, genetic factors, or environmental damage. Treatment approaches for facial veins often focus on addressing underlying skin conditions, sun protection, gentle skincare routines, and when necessary, laser therapy or intense pulsed light treatments to reduce visibility while preserving skin health.
6. Chest and Breast Vein Patterns - The Thoracic Network
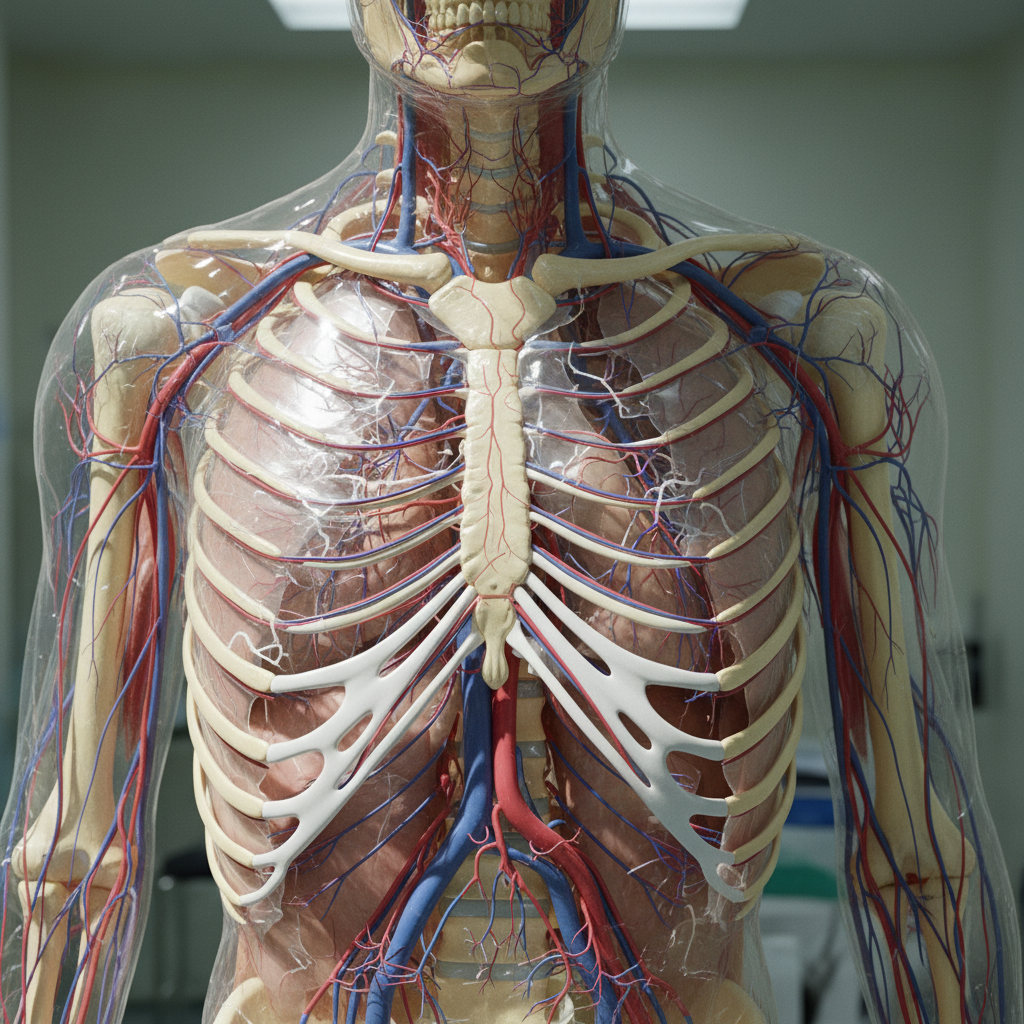
Visible veins across the chest and breast area create patterns that can provide important insights into circulatory health, hormonal changes, and potential underlying conditions. The normal chest vein pattern typically consists of subtle vessels that may become more apparent during certain physiological states or life stages. During pregnancy, breast veins often become dramatically more visible due to increased blood volume, hormonal changes, and breast tissue expansion in preparation for lactation. This enhanced venous pattern, sometimes called the "network of Haller," is completely normal and typically subsides after breastfeeding concludes. However, sudden appearance of prominent chest veins in non-pregnant individuals can indicate more serious conditions requiring medical attention. Superior vena cava syndrome, caused by compression or obstruction of the large vein draining the upper body, can cause dramatic dilation of chest wall veins as they serve as collateral circulation pathways. This condition may result from lung tumors, lymphomas, or other mediastinal masses. Breast cancer can also cause changes in breast vein patterns, particularly if tumors affect local blood flow or lymphatic drainage. Some women notice increased breast vein visibility during menstrual cycles due to hormonal fluctuations affecting blood vessel dilation and breast tissue changes. Weight fluctuations can also impact chest vein visibility, with weight loss making vessels more apparent due to decreased subcutaneous fat. Athletes and individuals with well-developed pectoral muscles may have more visible chest veins due to increased muscle mass and reduced body fat. Understanding these patterns helps distinguish between normal physiological variations and changes that might warrant medical evaluation, particularly when accompanied by other symptoms like shortness of breath, chest pain, or breast changes.
7. Temple Vein Prominence - The Temporal Indicators
Temporal veins, located at the temples on either side of the head, can become prominently visible and create distinctive patterns that may indicate various health conditions or physiological states. The temporal arteries and veins form a complex network that supplies blood to and from the scalp, forehead, and temporal regions of the head. Normal temporal vein visibility can increase with age as skin becomes thinner and vessels may become more tortuous. However, sudden or dramatic changes in temporal vein patterns warrant careful attention as they can signal important health developments. Temporal arteritis, also known as giant cell arteritis, is a serious inflammatory condition affecting the temporal arteries that can cause them to become swollen, tender, and visibly prominent. This condition primarily affects individuals over 50 years old and can lead to serious complications including vision loss if left untreated. Symptoms often include headaches, jaw claudication, scalp tenderness, and general malaise. Dehydration can also cause temporal veins to become more prominent as the body attempts to maintain circulation with reduced blood volume. High blood pressure may contribute to temporal vessel prominence, particularly during hypertensive episodes or with poorly controlled chronic hypertension. Stress and tension can cause temporary dilation of temporal vessels, often accompanied by tension headaches. Certain medications, particularly vasodilators, can increase temporal vein visibility. Physical exertion, especially activities that increase intracranial pressure like weightlifting or straining, can temporarily make temporal veins more prominent. Understanding these patterns and their potential implications helps individuals recognize when temporal vein changes might require medical evaluation, particularly when accompanied by headaches, vision changes, or other concerning symptoms.
8. Abdominal Vein Patterns - The Central Circulation Display
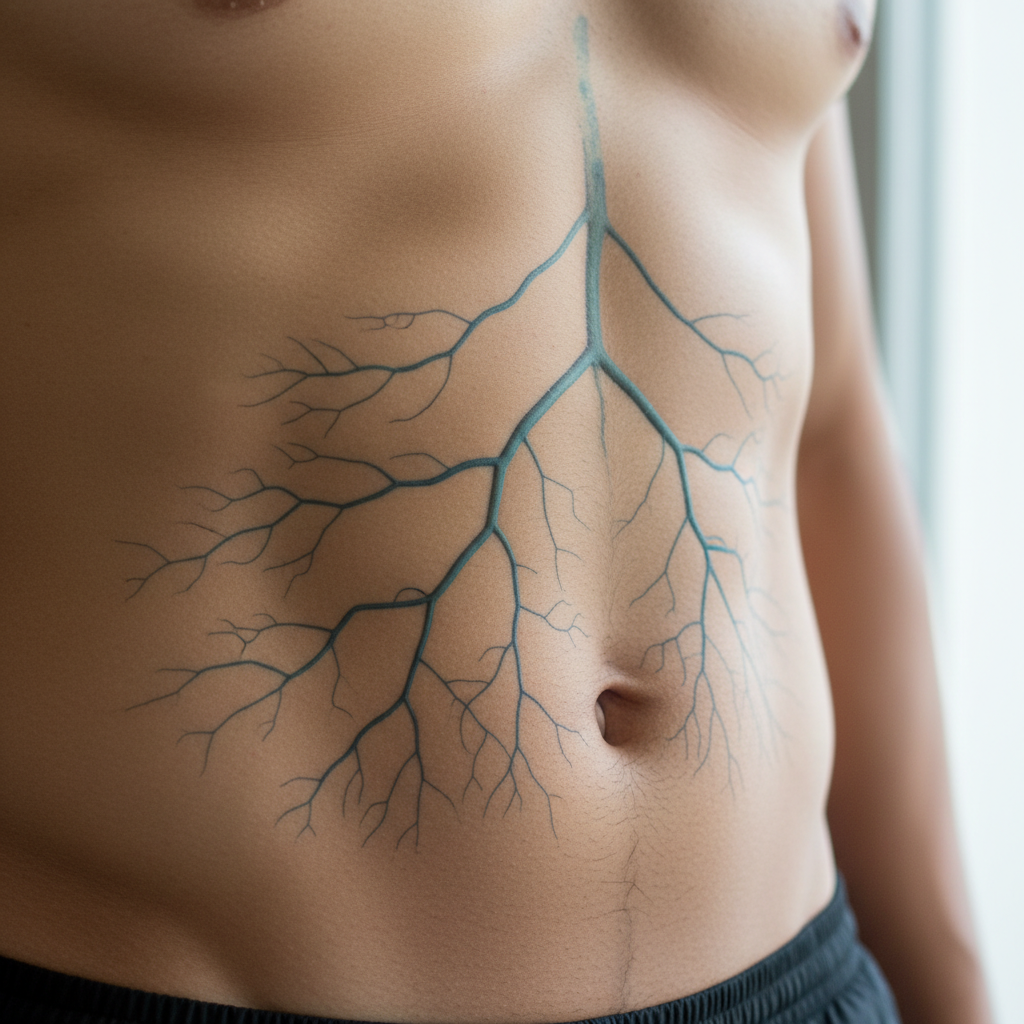
Visible veins across the abdomen can create various patterns that provide valuable insights into circulatory health and potential underlying medical conditions. Normal abdominal skin typically conceals the underlying venous network, making any prominent venous patterns potentially significant. The most concerning abdominal vein pattern is caput medusae, named after the mythological Medusa's snake-like hair, which appears as dilated veins radiating from the umbilicus (belly button). This pattern typically indicates portal hypertension, a serious condition where increased pressure in the portal vein system causes blood to seek alternative pathways back to the heart. Portal hypertension commonly results from liver cirrhosis, liver fibrosis, or other conditions that impair normal liver blood flow. The dilated umbilical and paraumbilical veins create the characteristic radiating pattern as they serve as collateral circulation routes. Other abdominal vein patterns may indicate inferior vena cava obstruction, where blockage of the large vein returning blood from the lower body causes superficial abdominal veins to dilate as alternative pathways. Pregnancy can cause increased visibility of abdominal veins due to increased blood volume, hormonal changes, and pressure from the growing uterus on major blood vessels. Weight loss may make previously hidden abdominal veins more apparent as subcutaneous fat decreases. Certain medications, particularly those affecting blood vessel dilation, can increase abdominal vein visibility. Athletic individuals with low body fat percentages may have more visible abdominal veins due to reduced subcutaneous tissue. However, any sudden appearance of prominent abdominal vein patterns, particularly when accompanied by abdominal pain, swelling, or other symptoms, should prompt immediate medical evaluation as they may indicate serious underlying conditions requiring urgent treatment.
9. Leg Vein Mapping - The Lower Extremity Roadmap
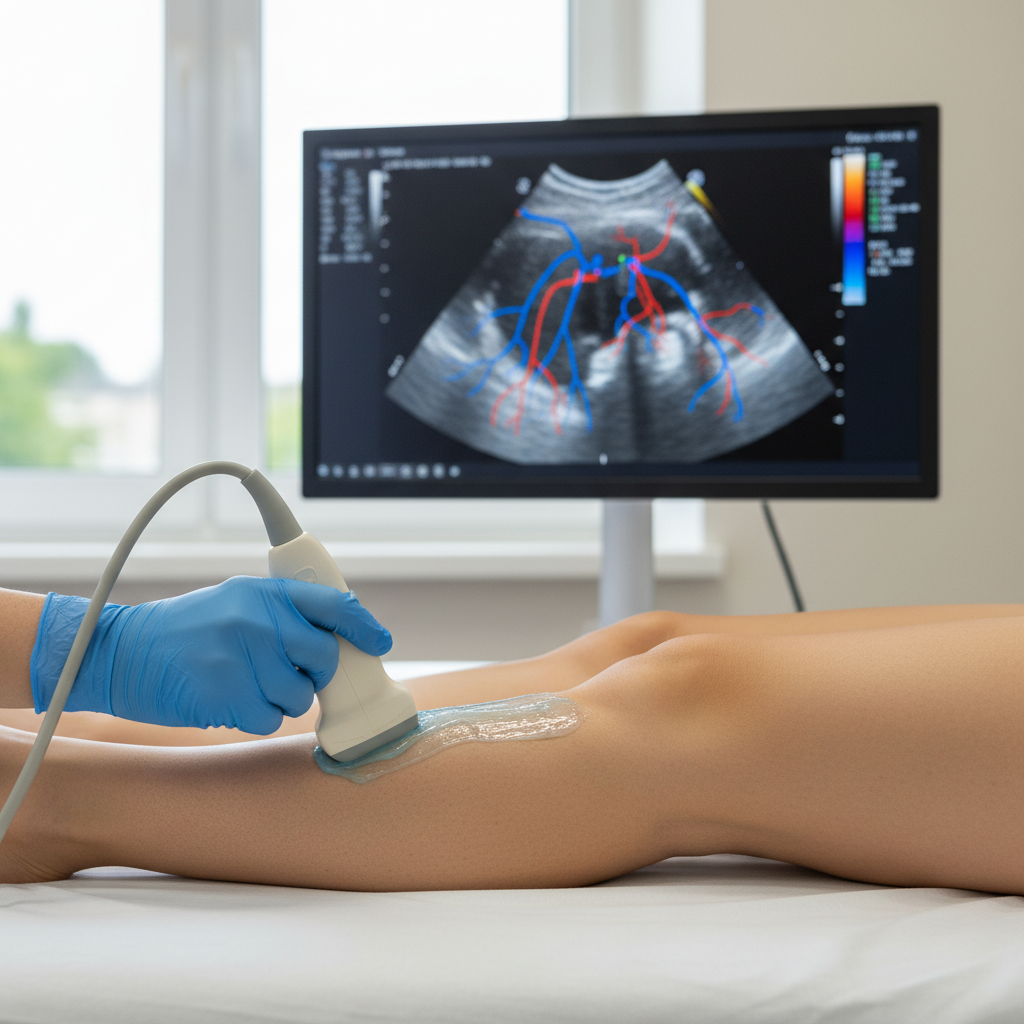
The legs contain the most complex and clinically significant venous patterns in the human body, serving as a roadmap to overall vascular health and circulation efficiency. The lower extremity venous system consists of three main components: the deep venous system, the superficial venous system, and the perforating veins that connect them. Understanding the various patterns of leg vein visibility can provide crucial insights into venous function and potential pathology. Normal leg veins may be subtly visible, particularly in individuals with fair skin or low body fat, but dramatic changes in patterns often indicate developing venous disease. The great saphenous vein, running from the ankle to the groin, is the longest vein in the body and frequently becomes varicose when valves fail. The small saphenous vein, running up the back of the calf, can also develop varicosities that create distinctive patterns. Perforating vein incompetence can cause localized areas of venous dilation and characteristic "blow-out" patterns where superficial veins become prominently dilated at specific locations. Chronic venous insufficiency often presents with progressive patterns of vein visibility, starting with spider veins and reticular veins before progressing to varicose veins and potentially more serious complications like venous ulcers. Deep vein thrombosis can cause superficial veins to become more prominent as they serve as collateral circulation when deep veins are blocked. Pregnancy commonly causes leg vein changes due to increased blood volume, hormonal effects on vein walls, and pressure from the growing uterus on pelvic veins. Athletic activities and occupational factors significantly influence leg vein patterns, with prolonged standing or sitting contributing to venous stasis and valve dysfunction. Understanding these complex patterns helps healthcare providers assess venous function, plan appropriate treatments, and monitor disease progression.
10. Neck Vein Distension - The Cardiac Connection
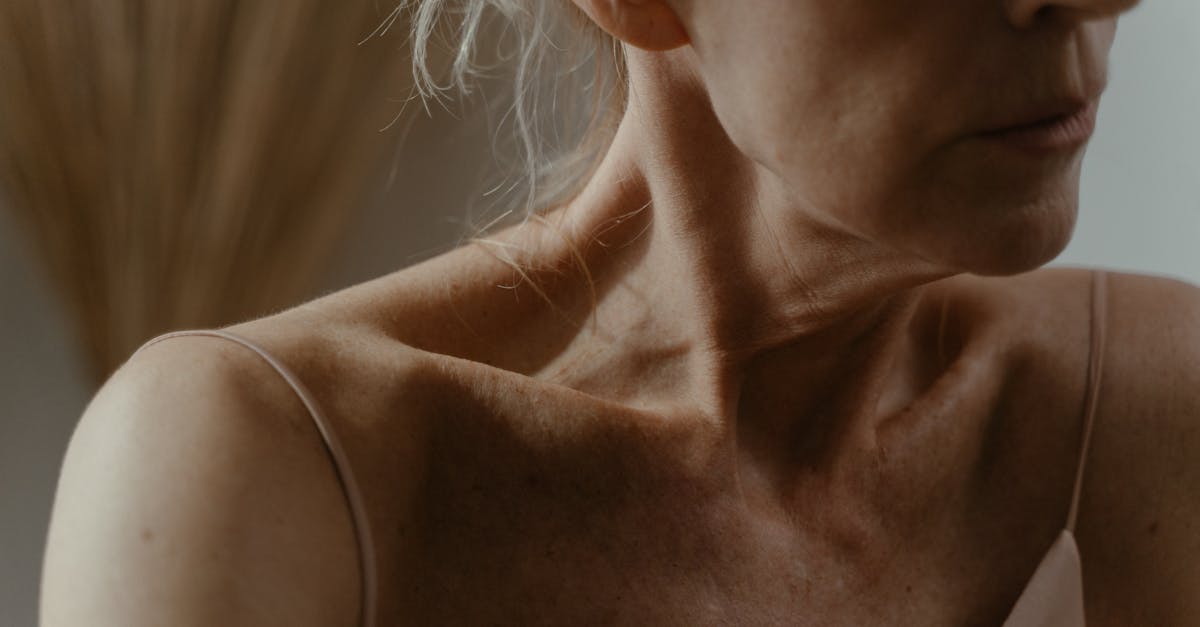
Neck vein patterns, particularly jugular vein distension, provide critical insights into cardiac function and central circulation status. The jugular veins, located on either side of the neck, serve as important indicators of central venous pressure and right heart function. Normal jugular veins are typically not visible when a person is sitting upright, but may become apparent when lying flat due to increased venous return. Abnormal jugular vein distension (JVD) occurs when these veins remain prominently visible even when the person is sitting at a 45-degree angle or higher, indicating elevated central venous pressure. This finding often suggests right heart failure, where the heart's right ventricle cannot effectively pump blood to the lungs, causing backup pressure throughout the venous system. Congestive heart failure commonly presents with JVD as one of its cardinal signs, along with shortness of breath, peripheral edema, and fatigue. Pulmonary hypertension can also cause JVD as increased pressure in the lung circulation creates back-pressure on the right heart. Tricuspid valve disease, whether stenosis or regurgitation, can manifest as prominent neck veins due to impaired blood flow through the right side of the heart. Pericardial disease, including pericarditis or pericardial effusion, can cause JVD by restricting the heart's ability to fill properly. Superior vena cava syndrome may cause neck vein distension along with facial swelling and prominent chest wall veins. Dehydration typically causes neck veins to become less visible, while fluid overload makes them more prominent. Healthcare providers use jugular vein assessment as a non-invasive method to evaluate cardiac function and guide treatment decisions. The height of jugular vein distension, measured in centimeters above the sternal angle, provides quantitative information about central venous pressure and helps monitor response to cardiac treatments.
11. Exercise-Induced Vein Changes - The Activity Response

Physical exercise creates dramatic and often temporary changes in vein patterns throughout the body, providing insights into cardiovascular fitness, hydration status, and vascular health. During exercise, the cardiovascular system undergoes significant adaptations to meet increased oxygen and nutrient demands of working muscles. Blood vessels dilate to accommodate increased blood flow, making veins more prominent and visible across the body. This exercise-induced vasodilation is a normal physiological response mediated by nitric oxide release and other vasodilatory mechanisms. Well-conditioned athletes often display more prominent vein patterns due to several factors including increased muscle mass, reduced subcutaneous fat, enhanced cardiovascular efficiency,