12 Tooth and Enamel Changes That Signal Nutritional and Digestive Issues
The human mouth serves as a remarkable diagnostic window into our overall health, with teeth and enamel acting as sensitive indicators of nutritional deficiencies and digestive disorders that may be developing silently within our bodies. Modern dental science has established compelling connections between oral manifestations and systemic health issues, revealing that changes in tooth structure, enamel integrity, and oral tissue health often precede more obvious symptoms of underlying conditions. When our digestive system fails to properly absorb essential nutrients or when chronic inflammation disrupts normal metabolic processes, the mouth frequently displays the first visible signs through alterations in tooth color, texture, strength, and overall oral environment. These dental changes occur because teeth and supporting structures require a constant supply of minerals, vitamins, and other nutrients to maintain their integrity, making them particularly vulnerable to nutritional imbalances. Understanding these oral indicators can provide invaluable early warning signs, enabling individuals and healthcare providers to identify and address underlying health issues before they progress to more serious stages. From subtle enamel erosion patterns that suggest acid reflux to distinctive tooth discoloration indicating mineral deficiencies, the following twelve dental changes represent critical signals that warrant immediate attention and comprehensive evaluation of both oral and systemic health status.
1. Enamel Erosion and Acid Reflux Disease
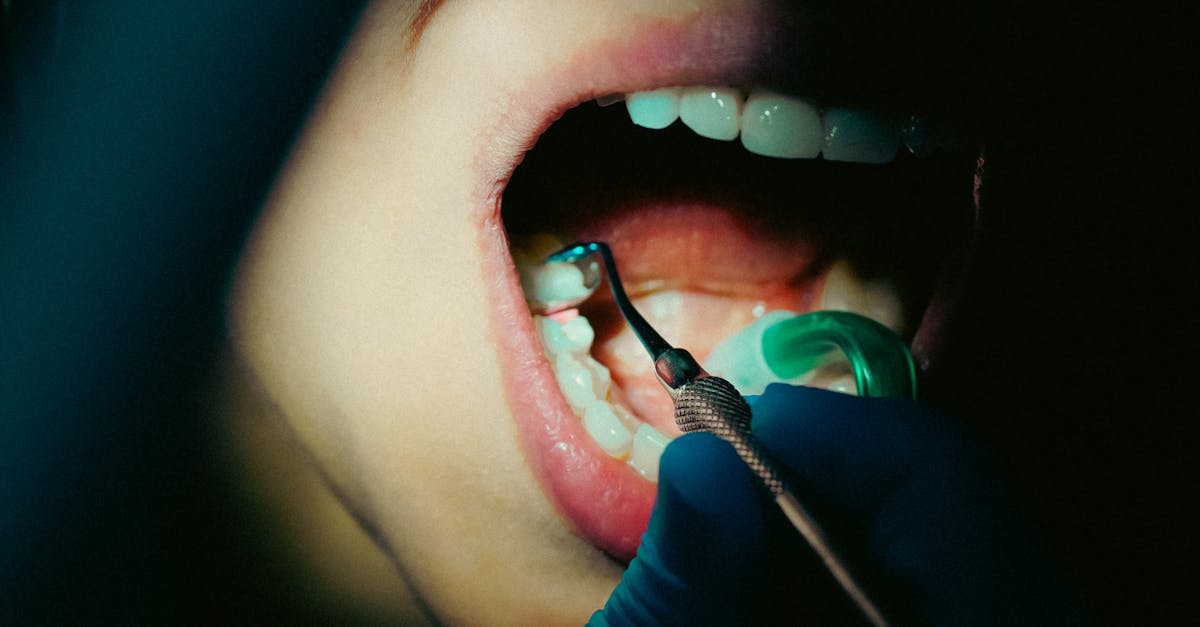
Enamel erosion represents one of the most significant dental indicators of gastroesophageal reflux disease (GERD) and other acid-related digestive disorders, manifesting as the gradual dissolution of the tooth's protective outer layer due to repeated exposure to stomach acid. When stomach acid reaches the oral cavity through reflux episodes, it creates an acidic environment that systematically weakens and dissolves the mineral structure of tooth enamel, particularly affecting the lingual surfaces of upper teeth and the occlusal surfaces of molars. This erosion pattern is distinctly different from cavity-related damage, appearing as smooth, glossy depressions or cupping on tooth surfaces rather than the rough, cavitated lesions typical of bacterial decay. The process occurs because stomach acid has a pH between 1.5 and 3.5, which is well below the critical pH of 5.5 at which enamel demineralization begins, making even brief contact potentially damaging to tooth structure. Patients with chronic acid reflux often develop characteristic wear patterns that dental professionals can readily identify, including thinning of enamel on the palatal surfaces of upper anterior teeth and flattening of posterior tooth cusps. The severity of erosion typically correlates with the frequency and duration of reflux episodes, making dental examination a valuable tool for assessing the effectiveness of GERD treatment and identifying patients who may require more aggressive acid suppression therapy. Early recognition of these erosion patterns allows for both protective dental interventions and appropriate medical evaluation to address the underlying digestive disorder before more extensive damage occurs.
2. Tooth Discoloration and Iron Deficiency
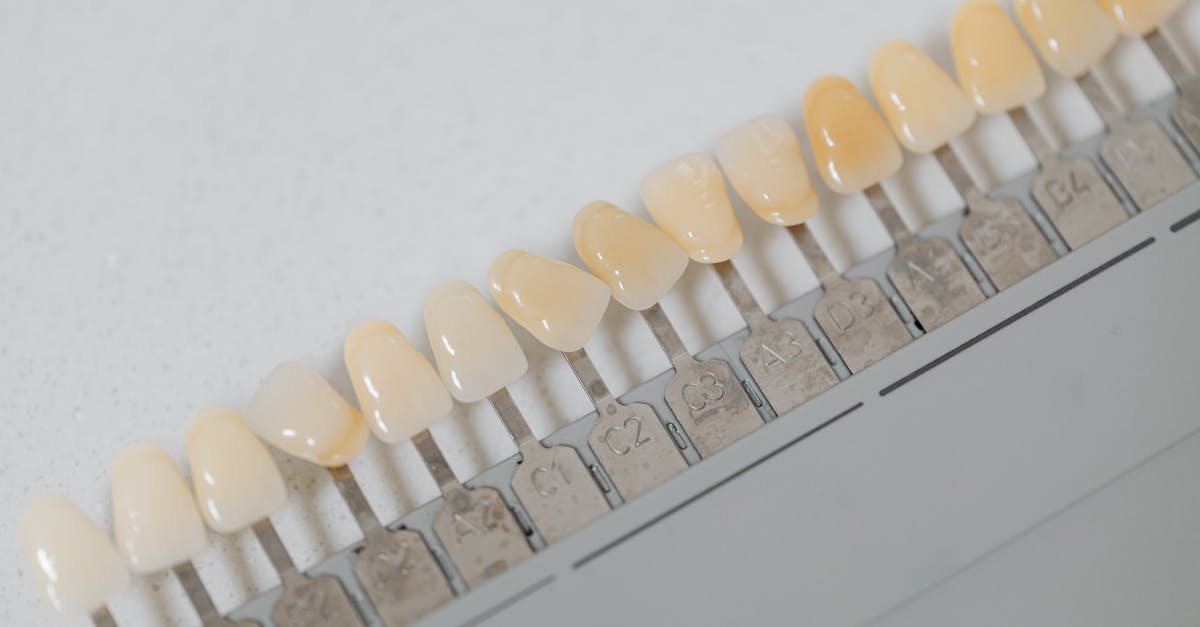
Iron deficiency, one of the most common nutritional deficiencies worldwide, frequently manifests in the oral cavity through distinctive changes in tooth color and oral tissue health that can serve as early indicators of this systemic condition. Teeth affected by iron deficiency often develop a characteristic pale, chalky appearance, particularly in the enamel, as iron plays a crucial role in the formation and maintenance of healthy tooth structure during development and throughout life. The discoloration occurs because iron is essential for proper collagen synthesis and mineralization processes that give teeth their natural translucency and color depth, and when iron levels are inadequate, these processes become compromised. Additionally, iron deficiency anemia creates an environment of chronic hypoxia in oral tissues, leading to poor circulation and reduced oxygen delivery to the dental pulp and supporting structures, which can result in a grayish or bluish tint to the teeth, particularly noticeable in the cervical regions. Patients with iron deficiency may also experience increased susceptibility to dental caries due to altered saliva composition and reduced immune function, creating a cycle where poor oral health further compromises nutritional status. The oral manifestations often appear before classic symptoms of iron deficiency anemia, such as fatigue and weakness, making dental examination a valuable screening tool for this condition. Furthermore, iron deficiency can affect the development of permanent teeth in children, leading to delayed eruption, altered crown morphology, and increased porosity of enamel that persists throughout life, emphasizing the importance of adequate iron nutrition during critical developmental periods.
3. Enamel Hypoplasia and Celiac Disease
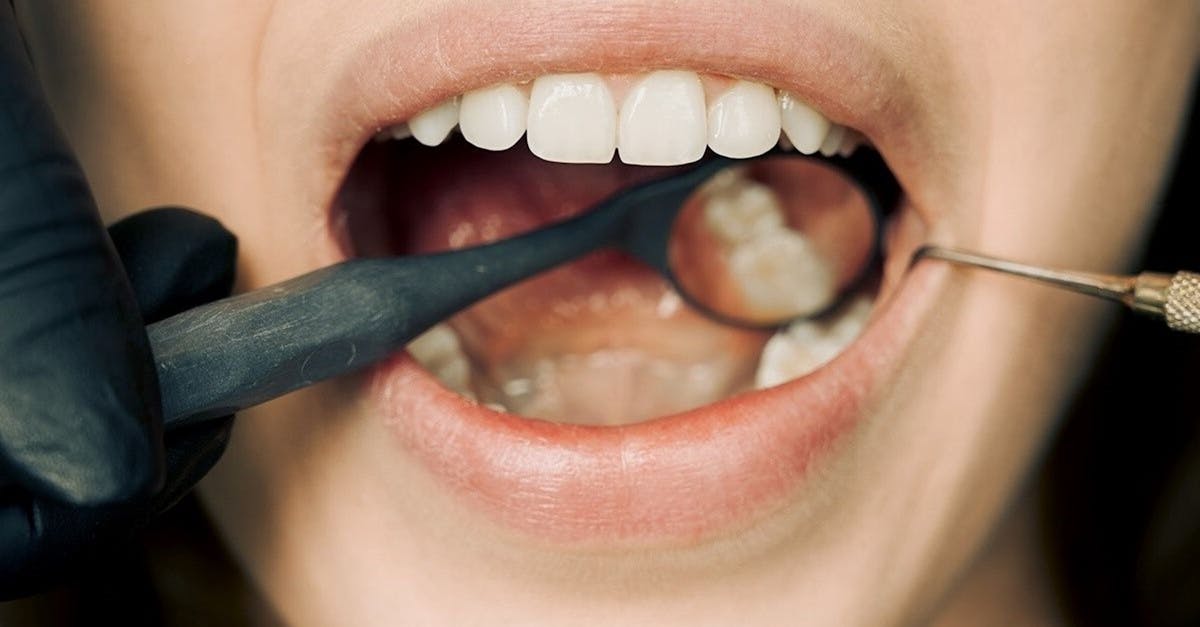
Celiac disease, an autoimmune disorder triggered by gluten consumption, frequently produces distinctive dental manifestations known as enamel hypoplasia, which appears as horizontal grooves, pits, or bands of discolored enamel that reflect periods of disrupted tooth development during childhood. These characteristic enamel defects occur because celiac disease causes chronic inflammation and villous atrophy in the small intestine, leading to malabsorption of essential nutrients required for proper tooth formation, including calcium, phosphorus, vitamin D, and various trace minerals. The timing and pattern of enamel hypoplasia can provide valuable information about when the celiac disease began affecting the patient, as the defects correspond to specific periods of tooth development when gluten exposure was causing intestinal damage and nutrient malabsorption. Research has shown that up to 95% of children with celiac disease exhibit some form of dental enamel defects, making oral examination a potentially valuable screening tool for this often-underdiagnosed condition. The enamel changes in celiac disease typically affect multiple teeth symmetrically, distinguishing them from localized trauma or infection-related defects, and often involve both primary and permanent dentitions depending on the age of onset. In addition to enamel hypoplasia, patients with celiac disease may experience delayed tooth eruption, increased susceptibility to dental caries due to altered enamel structure, and recurrent aphthous ulcers in the oral soft tissues. Early recognition of these dental signs can lead to prompt diagnosis and treatment of celiac disease, preventing long-term complications such as osteoporosis, infertility, and increased cancer risk while allowing for proper dental management to preserve remaining tooth structure and function.
4. Tooth Mobility and Calcium Deficiency

Calcium deficiency creates a cascade of oral health problems that begin with compromised tooth support structures and progress to increased tooth mobility, representing one of the most serious dental consequences of inadequate mineral nutrition. The alveolar bone that supports teeth requires constant calcium availability for remodeling and maintenance, and when dietary calcium is insufficient or absorption is impaired, the body prioritizes calcium delivery to vital organs by drawing from bone reserves, including the jawbone. This process, known as bone resorption, gradually weakens the foundation that holds teeth in place, leading to increased periodontal ligament space, loss of lamina dura on radiographs, and clinically detectable tooth mobility that worsens over time without intervention. Calcium deficiency often occurs in conjunction with vitamin D deficiency, as vitamin D is essential for calcium absorption in the intestines, creating a compound effect that accelerates bone loss around teeth and increases the risk of tooth loss. The condition is particularly problematic in postmenopausal women, individuals with lactose intolerance who avoid dairy products, and patients with digestive disorders that impair calcium absorption, such as Crohn's disease or chronic kidney disease. Early signs of calcium-related tooth mobility may be subtle, beginning with slight looseness during chewing or sensitivity to pressure, but can progress rapidly if the underlying deficiency is not addressed through dietary modification, supplementation, or treatment of underlying absorption disorders. Dental professionals can identify calcium deficiency through clinical examination, radiographic assessment of bone density around teeth, and correlation with patient history of dietary habits and medical conditions. Prompt recognition and treatment of calcium deficiency not only helps preserve remaining teeth but also prevents more serious complications such as pathologic fractures and severe osteoporosis that can significantly impact overall quality of life.
5. Delayed Tooth Eruption and Vitamin D Deficiency

Vitamin D deficiency profoundly affects dental development and eruption patterns, creating characteristic delays in tooth emergence that can serve as early indicators of this increasingly common nutritional deficiency. The active form of vitamin D, calcitriol, plays essential roles in calcium and phosphate homeostasis, bone mineralization, and cellular differentiation processes that are critical for normal tooth development and eruption timing. When vitamin D levels are inadequate, children experience delayed eruption of both primary and permanent teeth, often accompanied by altered crown morphology, increased enamel porosity, and higher susceptibility to dental caries due to compromised enamel quality. The mechanism behind delayed eruption involves disrupted osteoclastic and osteoblastic activity in the alveolar bone, which normally creates the pathway for erupting teeth while simultaneously forming the supporting bone structure around newly emerged teeth. Vitamin D deficiency also affects the development of tooth roots, leading to shortened, blunted, or malformed root structures that can compromise long-term tooth stability and function. Geographic location, seasonal variations in sun exposure, dietary habits, and skin pigmentation all influence vitamin D status, with populations at higher latitudes and individuals with limited sun exposure being at particular risk for deficiency-related dental problems. The dental manifestations of vitamin D deficiency often appear before classic symptoms such as rickets or osteomalacia become evident, making oral examination a valuable early screening tool for this condition. Additionally, vitamin D deficiency in pregnant women can affect fetal tooth development, leading to enamel defects and altered eruption patterns in their children, emphasizing the importance of adequate vitamin D nutrition throughout pregnancy and early childhood for optimal oral health outcomes.
6. Gingival Bleeding and B-Vitamin Complex Deficiencies
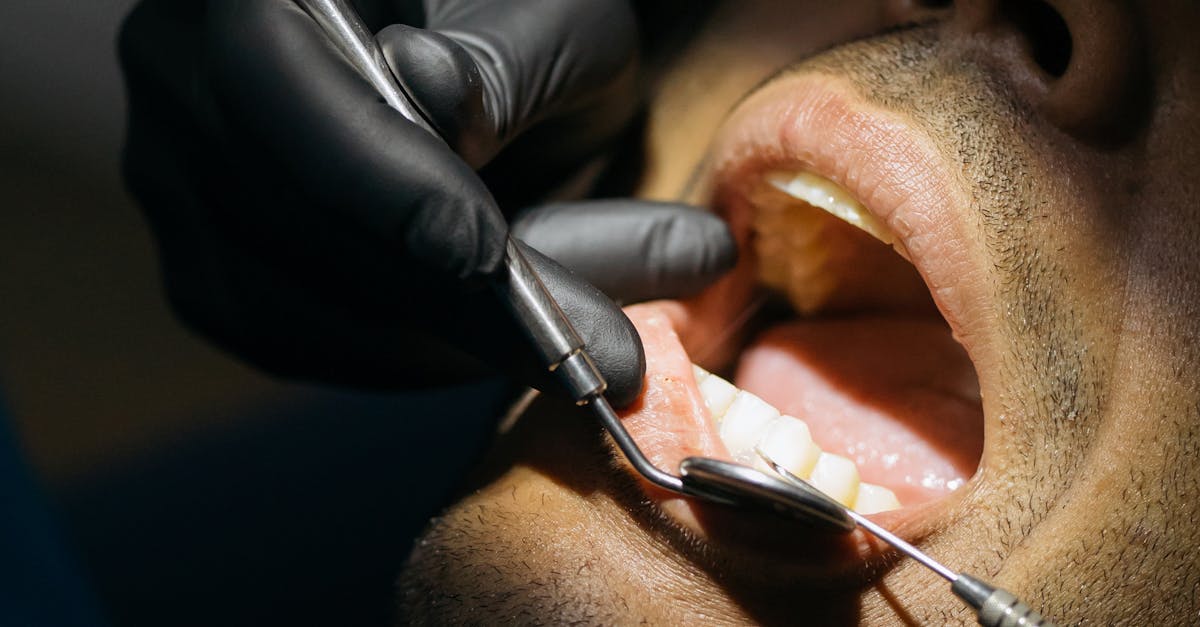
B-vitamin complex deficiencies create a spectrum of oral manifestations that prominently feature spontaneous gingival bleeding, tissue inflammation, and delayed healing responses that can significantly compromise periodontal health and overall oral function. The B-vitamin family, including thiamine (B1), riboflavin (B2), niacin (B3), pyridoxine (B6), cobalamin (B12), and folate, plays crucial roles in cellular metabolism, DNA synthesis, and tissue repair processes that are essential for maintaining healthy oral tissues. When these vitamins are deficient, the gingival tissues become fragile, hyperemic, and prone to bleeding even with minimal provocation, such as gentle tooth brushing or normal chewing forces. Folate and vitamin B12 deficiencies are particularly associated with severe gingival inflammation and bleeding because these vitamins are essential for proper DNA synthesis and cellular division in rapidly turning over oral tissues. The bleeding associated with B-vitamin deficiencies differs from that seen in typical gingivitis caused by plaque accumulation, as it tends to be more spontaneous, widespread, and resistant to conventional periodontal therapy until the underlying nutritional deficiency is corrected. Patients with B-vitamin deficiencies may also develop characteristic oral ulcerations, glossitis with a smooth, red tongue surface, and angular cheilitis at the corners of the mouth, creating a constellation of symptoms that can significantly impact eating, speaking, and overall quality of life. These deficiencies are commonly seen in individuals with malabsorption disorders, strict vegetarians who don't supplement B12, elderly patients with poor dietary intake, and individuals with chronic alcoholism who have impaired vitamin absorption and increased metabolic demands. Recognition of these oral signs can lead to early diagnosis and treatment of B-vitamin deficiencies, preventing progression to more serious complications such as megaloblastic anemia, peripheral neuropathy, and cognitive impairment.
7. Tooth Sensitivity and Magnesium Deficiency
Magnesium deficiency manifests in the oral cavity through increased tooth sensitivity, enamel weakness, and altered pain perception that can significantly impact daily activities such as eating and drinking. Magnesium serves as a cofactor for over 300 enzymatic reactions in the body, including those involved in calcium metabolism, protein synthesis, and nerve function, making its deficiency particularly problematic for dental health. When magnesium levels are inadequate, the normal calcium-phosphate balance in teeth becomes disrupted, leading to decreased enamel mineralization and increased permeability of dentinal tubules, which allows external stimuli to more easily reach the dental pulp and trigger pain responses. The tooth sensitivity associated with magnesium deficiency typically presents as sharp, shooting pain in response to temperature changes, sweet or acidic foods, and even air exposure, often affecting multiple teeth simultaneously rather than being localized to a single tooth. Magnesium deficiency also affects the function of voltage-gated calcium channels in nerve cells, potentially amplifying pain signals and creating hypersensitivity to stimuli that would normally be tolerable. This condition is increasingly common due to modern agricultural practices that have depleted soil magnesium levels, processed food diets that are naturally low in magnesium, and increased consumption of substances that interfere with magnesium absorption, such as caffeine, alcohol, and certain medications. Patients with digestive disorders such as Crohn's disease, celiac disease, or chronic diarrhea are at particularly high risk for magnesium deficiency due to impaired absorption or increased losses. The dental manifestations of magnesium deficiency often improve dramatically with appropriate supplementation, but the underlying absorption issues must be addressed to prevent recurrence. Recognition of this connection allows dental professionals to recommend appropriate medical evaluation and nutritional intervention that can provide significant relief from tooth sensitivity while addressing the underlying systemic deficiency.
8. Enamel Fluorosis and Fluoride Toxicity
Enamel fluorosis represents a unique form of tooth discoloration and structural change that results from excessive fluoride exposure during tooth development, creating distinctive white spots, brown staining, or pitted enamel surfaces that serve as permanent markers of fluoride toxicity. This condition occurs when fluoride intake exceeds the optimal range during the critical period of enamel formation, typically between birth and eight years of age, leading to disrupted ameloblast function and altered enamel crystal formation. The severity of fluorosis ranges from mild white striping barely visible to the naked eye to severe brown discoloration with surface pitting and structural weakness that compromises tooth function and aesthetics. Fluoride toxicity can result from multiple sources, including fluoridated water supplies, fluoride toothpaste ingestion, fluoride supplements, and naturally occurring fluoride in groundwater, with the cumulative effect being more important than any single source. The mechanism of fluorosis involves fluoride incorporation into the developing enamel matrix, where it interferes with normal protein processing and mineral deposition, creating areas of hypomineralization that appear as white spots in mild cases or hypermineralization that appears as brown staining in severe cases. Geographic variations in fluorosis prevalence reflect differences in water fluoride levels, with some regions having naturally high fluoride concentrations that exceed recommended levels for dental health. While mild fluorosis may be primarily a cosmetic concern, severe fluorosis can compromise enamel strength and increase susceptibility to dental caries, creating a paradoxical situation where excessive fluoride exposure intended to prevent cavities actually increases cavity risk. The recognition of fluorosis patterns helps dental professionals assess community fluoride exposure levels and make recommendations for appropriate fluoride use, particularly in children who may be receiving fluoride from multiple sources simultaneously. Understanding fluorosis also highlights the importance of the dose-response relationship in nutrition and toxicology, demonstrating that even beneficial substances can become harmful when consumed in excessive amounts.
9. Oral Ulcerations and Zinc Deficiency
Zinc deficiency creates a characteristic pattern of recurrent oral ulcerations, delayed wound healing, and altered taste perception that can significantly impact nutritional intake and overall quality of life. Zinc plays essential roles in protein synthesis, immune function, and tissue repair processes, making its deficiency particularly problematic for the rapidly regenerating tissues of the oral cavity. When zinc levels are inadequate, patients develop frequent, painful aphthous ulcers that are typically larger, deeper, and slower to heal than those seen in individuals with normal zinc status. The ulcerations associated with zinc deficiency often appear on the tongue, buccal mucosa, and soft palate, creating multiple painful lesions that interfere with eating, speaking, and oral hygiene maintenance. Zinc deficiency also impairs immune function, making patients more susceptible to secondary bacterial and fungal infections in the oral cavity, which can complicate the healing process and create chronic inflammatory conditions. The altered taste perception that accompanies zinc deficiency, known as dysgeusia, can lead to reduced appetite and further nutritional compromise, creating a vicious cycle where poor intake worsens the deficiency and prolongs oral symptoms. Zinc deficiency is commonly seen in elderly individuals with poor dietary intake, patients with malabsorption disorders, individuals following restrictive diets, and those with increased zinc losses due to chronic diarrhea or certain medications. The oral manifestations of zinc deficiency often improve rapidly with appropriate supplementation, typically showing healing of existing ulcers within days and prevention of new lesions within weeks of starting treatment. Recognition of these oral signs is particularly important because zinc deficiency can have serious systemic consequences, including impaired immune function, delayed wound healing throughout the body, and increased susceptibility to infections. Dental professionals can play a crucial role in identifying zinc deficiency through careful oral examination and appropriate referral for nutritional assessment and treatment.
10. Tooth Grinding and Stress-Related Digestive Issues

Tooth grinding, or bruxism, often serves as a physical manifestation of stress-related digestive disorders, creating a complex interplay between psychological stress, gastrointestinal dysfunction, and oral health that can significantly impact overall well-being. Chronic stress affects the digestive system through multiple pathways, including altered gut motility, increased gastric acid production, disrupted gut microbiome balance, and compromised intestinal barrier function, all of which can lead to symptoms such as irritable bowel syndrome, gastritis, and inflammatory bowel disease. The stress response also triggers increased muscle tension throughout the body, including the muscles of mastication, leading to unconscious clenching and grinding behaviors that typically occur during sleep when conscious control is reduced. The relationship between stress, digestive issues, and bruxism is further complicated by the gut-brain axis, a bidirectional communication system between the central nervous system and the enteric nervous system that allows digestive problems to influence mood and stress levels while stress affects digestive function. Patients with stress-related digestive disorders often exhibit characteristic patterns of tooth wear,