12 Lower Leg Skin Changes That Reflect Vascular and Circulatory Health
The lower extremities serve as remarkable indicators of our cardiovascular and circulatory well-being, with the skin acting as a visible canvas that displays the intricate relationship between blood flow, tissue perfusion, and overall vascular health. The lower legs, positioned furthest from the heart and subject to gravitational challenges, are particularly vulnerable to circulatory compromises that manifest through distinctive skin changes. These dermatological alterations often represent the earliest visible signs of underlying vascular conditions, ranging from venous insufficiency and arterial disease to systemic circulation disorders. Healthcare professionals have long recognized that careful observation of lower leg skin characteristics can provide invaluable insights into a patient's cardiovascular status, often revealing conditions before they progress to more serious complications. The skin's appearance, texture, color, temperature, and healing capacity all reflect the adequacy of blood supply and the efficiency of venous return. Understanding these visual cues enables early intervention and appropriate management of vascular conditions that might otherwise go undetected until advanced stages. This comprehensive exploration examines twelve specific skin changes that serve as critical indicators of vascular and circulatory health, providing both medical professionals and individuals with essential knowledge for recognizing and addressing potential circulation issues before they become life-threatening complications.
1. Chronic Venous Stasis Dermatitis - The Foundation of Venous Disease
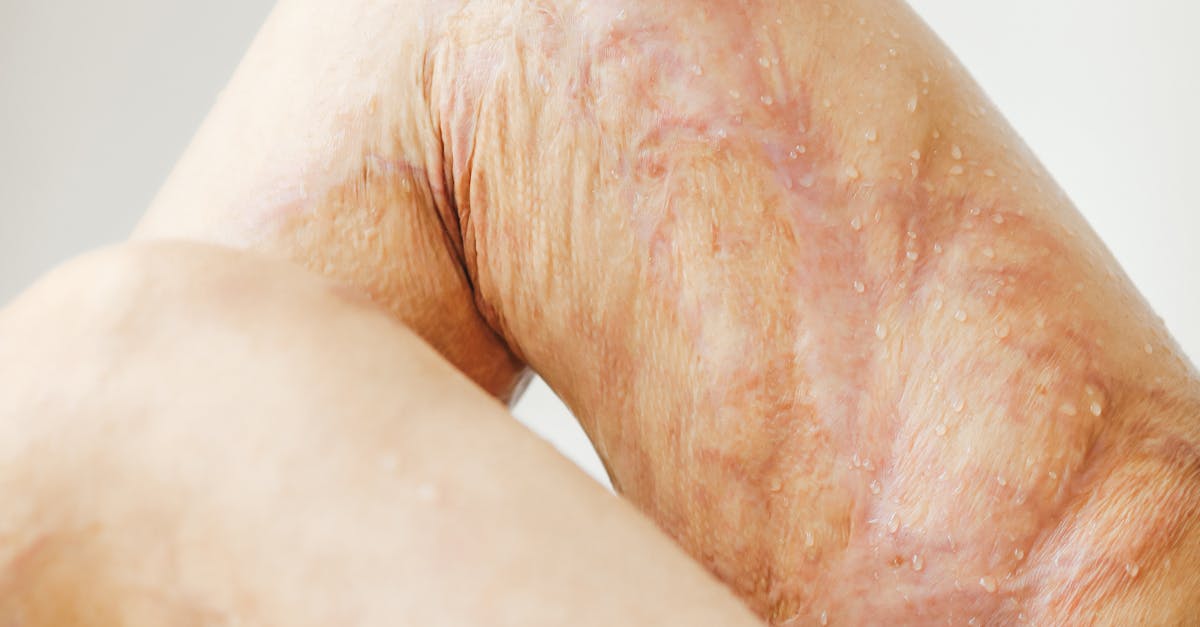
Chronic venous stasis dermatitis represents one of the most common and recognizable manifestations of venous insufficiency, characterized by inflammatory skin changes that develop as a direct result of prolonged venous hypertension and impaired venous return. This condition typically begins with subtle erythema and scaling around the ankles and gradually progresses to involve larger areas of the lower leg, creating a distinctive pattern of inflammation that reflects the underlying hemodynamic dysfunction. The pathophysiology involves increased venous pressure leading to capillary leakage, tissue edema, and subsequent inflammatory cascade that damages the skin's protective barrier. Patients often experience intense pruritus, which can lead to secondary bacterial infections and further skin deterioration through scratching and trauma. The affected skin becomes increasingly sensitive and reactive, developing a characteristic eczematous appearance with scaling, weeping, and crusting. Over time, the inflammatory process can lead to permanent skin changes including hyperpigmentation, fibrosis, and ultimately venous leg ulceration. Early recognition and treatment of venous stasis dermatitis are crucial for preventing progression to more severe complications, with management focusing on improving venous return through compression therapy, elevation, and addressing underlying venous pathology. The presence of stasis dermatitis should prompt comprehensive evaluation of the venous system to identify and treat any correctable causes of venous insufficiency.
2. Hemosiderin Deposition and Hyperpigmentation - Iron's Lasting Mark
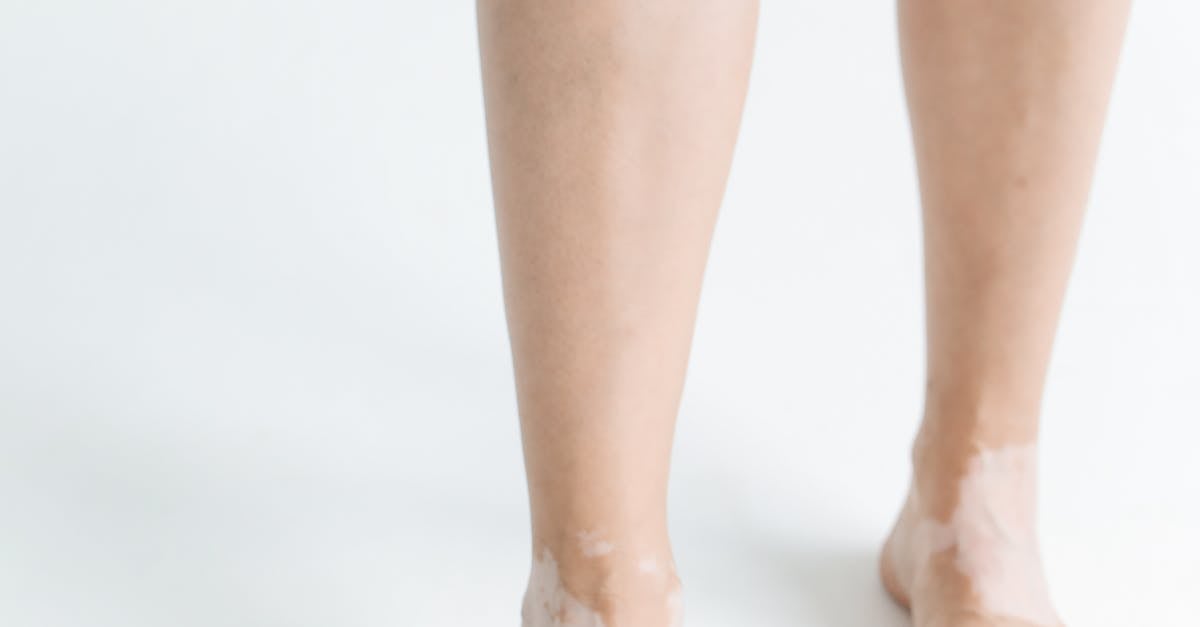
Hemosiderin deposition creates one of the most persistent and characteristic signs of chronic venous disease, manifesting as brownish-red discoloration that typically appears around the ankles and gradually extends upward along the lower leg. This distinctive pigmentation results from the breakdown of red blood cells that have extravasated from compromised capillaries due to increased venous pressure and chronic inflammation. When red blood cells are destroyed in the tissues, they release iron-containing hemoglobin, which is subsequently converted to hemosiderin and deposited within dermal macrophages and tissue spaces. Unlike other forms of hyperpigmentation that may fade over time, hemosiderin deposition tends to be permanent, serving as a lasting marker of previous or ongoing venous insufficiency. The distribution pattern of this pigmentation often follows the areas of greatest venous pressure, typically concentrated around the medial ankle and extending in a "gaiter" distribution around the lower leg. The intensity and extent of hemosiderin staining generally correlate with the severity and duration of venous disease, making it a valuable clinical indicator for assessing disease progression. While the pigmentation itself is primarily a cosmetic concern, its presence indicates significant underlying vascular pathology that requires attention to prevent further complications. Treatment options for established hemosiderin staining are limited, emphasizing the importance of early intervention in venous disease to prevent this irreversible change.
3. Lipodermatosclerosis - When Skin Becomes Armor

Lipodermatosclerosis represents an advanced manifestation of chronic venous insufficiency, characterized by progressive fibrosis and induration of the subcutaneous tissue that creates a distinctive "inverted champagne bottle" appearance of the lower leg. This condition develops through a complex inflammatory process involving chronic venous hypertension, tissue hypoxia, and persistent edema that ultimately leads to fibroblast activation and excessive collagen deposition. The affected skin becomes increasingly thick, woody, and bound down to underlying structures, losing its normal elasticity and mobility. The inflammatory phase, often called acute lipodermatosclerosis, presents with erythema, warmth, and tenderness that can be mistaken for cellulitis, leading to inappropriate antibiotic treatment. As the condition progresses to the chronic phase, the inflammation subsides, leaving behind dense fibrotic tissue that permanently alters the leg's contour and function. The fibrotic process typically affects the area between the knee and ankle, sparing the foot and creating the characteristic bottle-shaped appearance. This transformation significantly impairs lymphatic drainage and further compromises tissue perfusion, creating a cycle of progressive deterioration. Patients with lipodermatosclerosis face increased risk of developing venous leg ulcers, as the fibrotic tissue has poor healing capacity and is prone to breakdown with minor trauma. Early recognition and aggressive treatment of the underlying venous disease are essential to prevent or slow the progression of this debilitating condition.
4. Atrophie Blanche - Porcelain Scars of Vascular Compromise
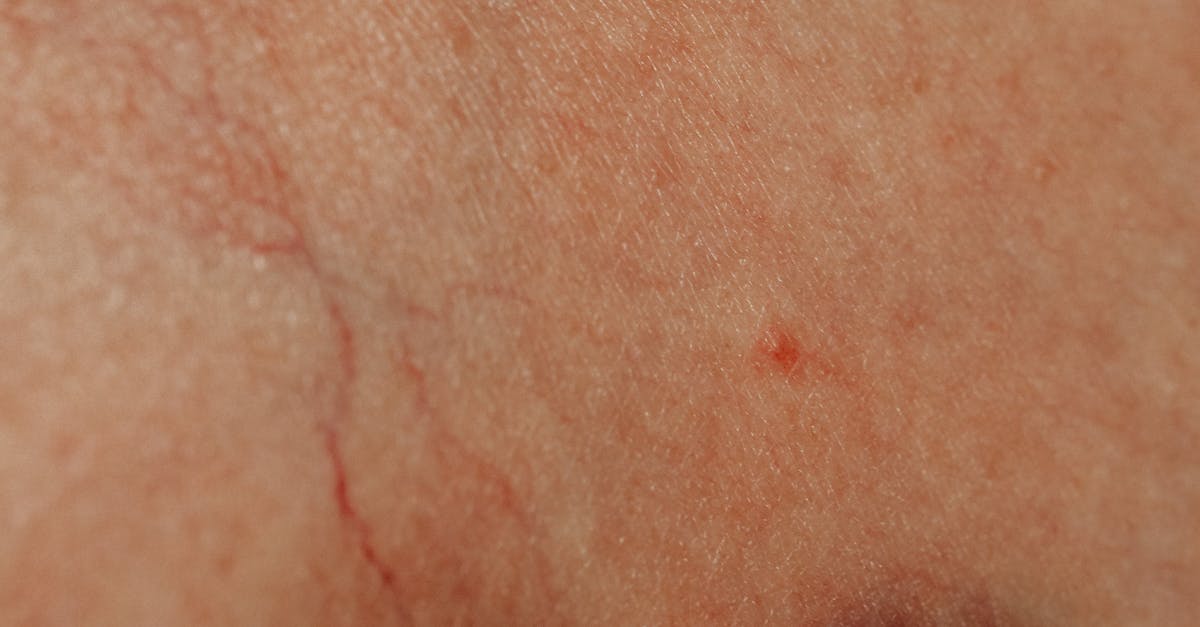
Atrophie blanche manifests as distinctive white, atrophic scars surrounded by hyperpigmentation and telangiectasias, creating a characteristic "porcelain-like" appearance that serves as a pathognomonic sign of severe chronic venous insufficiency. These ivory-colored patches develop following episodes of painful ulceration or tissue necrosis, representing areas where the skin has undergone ischemic damage and subsequent healing with minimal viable tissue remaining. The pathogenesis involves microvascular occlusion, often triggered by fibrin deposition and thrombosis in dermal capillaries, leading to localized tissue death and eventual replacement with avascular scar tissue. The surrounding hyperpigmentation results from hemosiderin deposition, while the prominent telangiectasias reflect compensatory vascular proliferation attempting to restore perfusion to the compromised area. These lesions are typically painful, particularly during the acute ulcerative phase, and demonstrate poor healing capacity due to the underlying vascular compromise. The white atrophic areas are extremely fragile and prone to recurrent breakdown with minimal trauma, creating a cycle of ulceration and re-epithelialization that gradually expands the affected area. Atrophie blanche is considered a pre-ulcerative condition, with affected individuals having a significantly increased risk of developing chronic venous leg ulcers. The presence of these lesions indicates severe underlying venous pathology requiring comprehensive evaluation and aggressive management to prevent further tissue loss and functional impairment.
5. Corona Phlebectatica - The Ankle's Vascular Crown
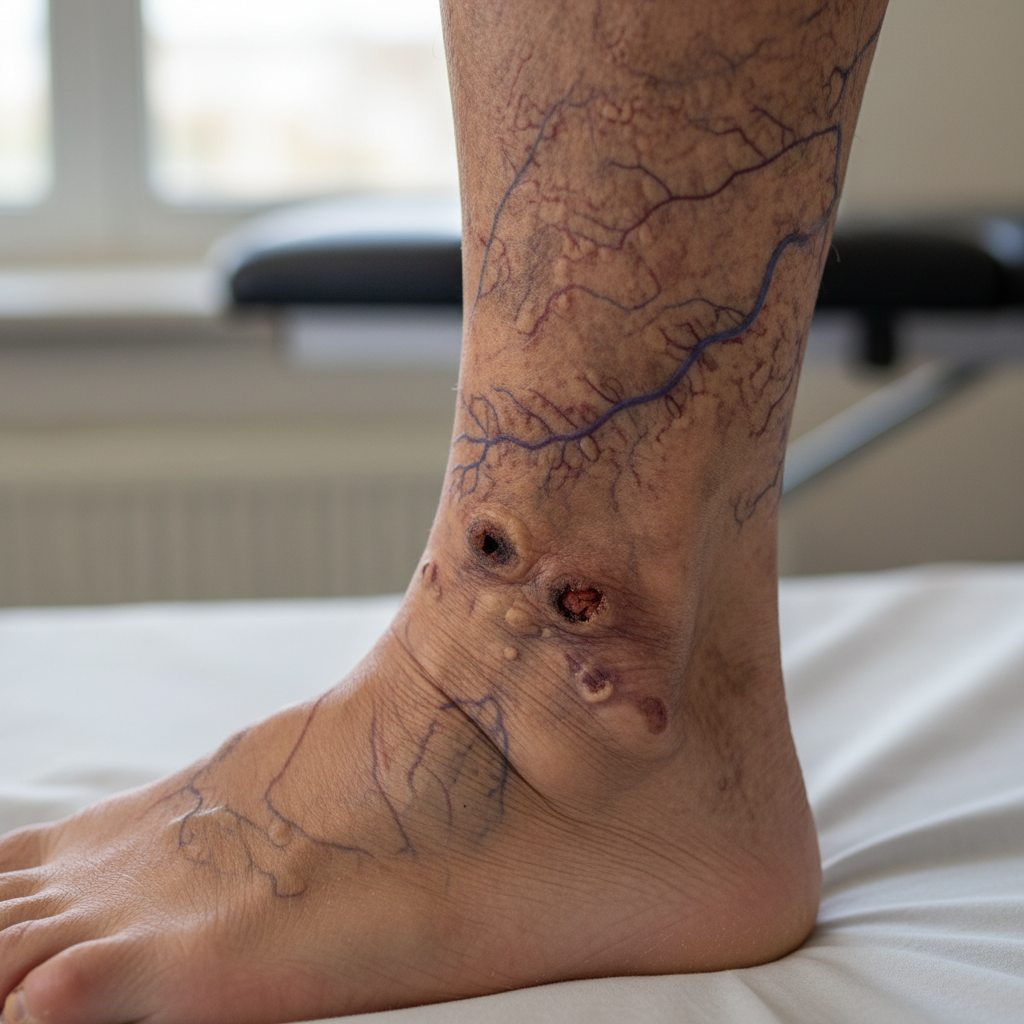
Corona phlebectatica, also known as ankle flare or malleolar flare, presents as a distinctive pattern of small, dilated intradermal veins that form a characteristic fan-shaped or crown-like distribution around the medial and lateral malleoli. These fine, blue-purple vessels represent the earliest visible sign of venous insufficiency, often appearing before other manifestations of chronic venous disease become apparent. The development of corona phlebectatica results from increased venous pressure being transmitted through incompetent perforating veins to the superficial dermal venous plexus, causing these normally invisible vessels to dilate and become prominent. Unlike simple spider veins or telangiectasias that may occur anywhere on the leg, corona phlebectatica has a specific anatomical distribution that directly correlates with areas of perforating vein incompetence. The presence of this finding should prompt careful evaluation for underlying venous insufficiency, as it often precedes the development of more serious complications such as skin changes, ulceration, and thrombotic events. The intensity and extent of ankle flare generally correlate with the severity of venous reflux, making it a useful clinical marker for disease progression. While corona phlebectatica itself is primarily a cosmetic concern, its recognition is crucial for early intervention in venous disease. Treatment typically involves addressing the underlying venous insufficiency through compression therapy, lifestyle modifications, and potentially surgical intervention to correct incompetent perforating veins and prevent progression to more advanced stages of chronic venous disease.
6. Arterial Insufficiency and Skin Atrophy - When Blood Flow Fails
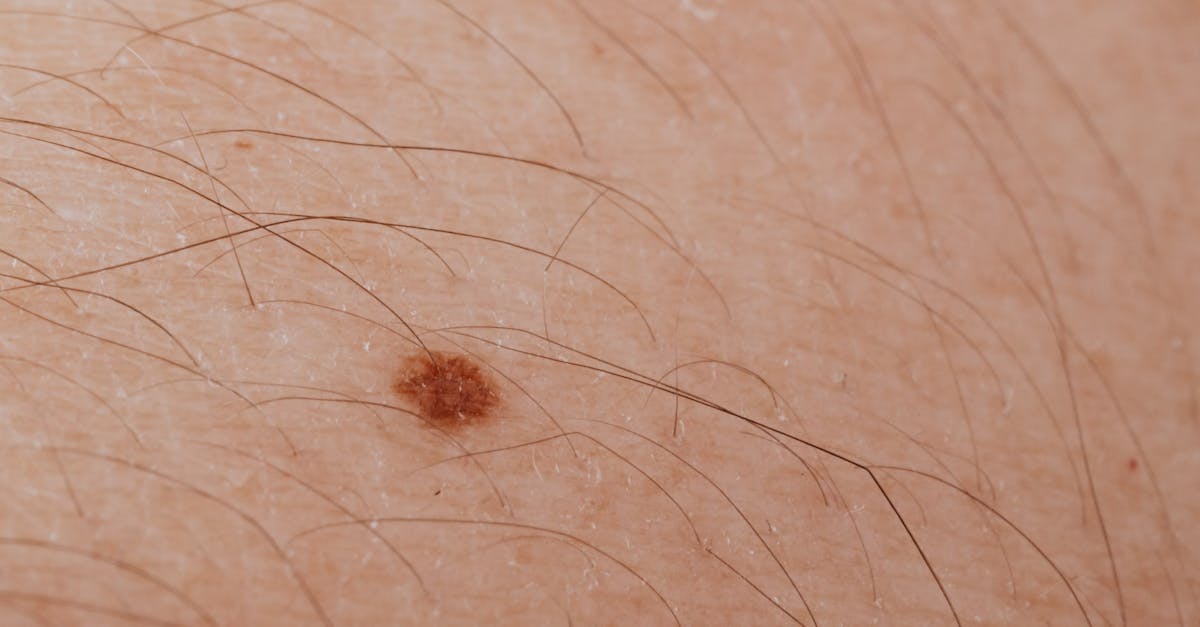
Arterial insufficiency creates a distinctly different pattern of skin changes compared to venous disease, characterized by progressive tissue atrophy, hair loss, and a characteristic shiny, taut appearance that reflects chronic hypoxia and malnutrition of the skin and subcutaneous tissues. The affected skin becomes thin, fragile, and translucent, with loss of normal skin appendages including hair follicles and sebaceous glands, creating a smooth, hairless surface that feels cool to touch. The reduced arterial perfusion leads to decreased delivery of oxygen and nutrients essential for normal cellular metabolism and tissue maintenance, resulting in progressive atrophy of all skin layers. Patients often develop a characteristic pallor that becomes more pronounced with elevation of the affected limb, followed by dependent rubor when the leg is lowered, reflecting the compromised autoregulation of cutaneous blood flow. The skin's healing capacity becomes severely impaired, with minor injuries taking weeks or months to heal and frequently progressing to chronic, non-healing ulcers. Temperature changes become more pronounced, with the affected limb feeling persistently cold due to reduced blood flow and impaired thermoregulation. The development of these changes indicates significant arterial compromise that may progress to critical limb ischemia if left untreated. Early recognition of arterial insufficiency skin changes is crucial for preventing limb loss, as timely intervention with revascularization procedures can restore blood flow and prevent irreversible tissue damage.
7. Dependent Rubor and Elevation Pallor - Gravity's Revealing Test
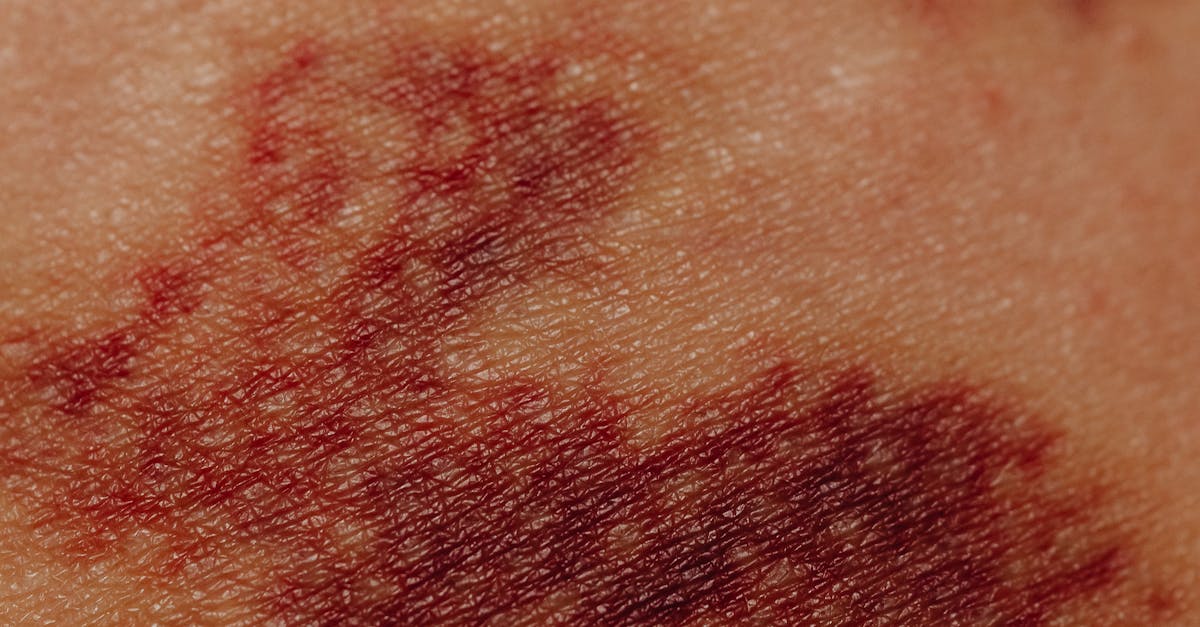
Dependent rubor and elevation pallor represent classic physical findings that demonstrate the severity of arterial insufficiency through simple positional changes that reveal the compromised circulation's inability to maintain adequate perfusion against gravitational forces. When the affected limb is elevated above heart level, the inadequate arterial pressure fails to overcome gravity, resulting in dramatic pallor as blood drains from the superficial vessels and insufficient arterial inflow occurs to maintain normal skin color. Conversely, when the limb is placed in a dependent position, gravity assists venous pooling and the compromised arterial system becomes engorged, creating an abnormal reddish-purple discoloration known as dependent rubor. This color change typically takes longer to develop than normal reactive hyperemia, often requiring several minutes for the full rubor to appear, indicating the sluggish circulation characteristic of arterial disease. The intensity of these color changes correlates directly with the severity of arterial compromise, with more pronounced pallor and rubor indicating more severe ischemia. Healthcare providers use this simple bedside test as part of the comprehensive vascular examination, as it provides immediate visual confirmation of arterial insufficiency without requiring sophisticated equipment. The presence of significant elevation pallor and dependent rubor indicates advanced arterial disease that may require urgent intervention to prevent tissue loss. Patients who demonstrate these findings often experience significant functional limitations, including pain with elevation and the need to sleep with their legs dependent to maintain adequate comfort.
8. Venous Leg Ulcers - The Ultimate Expression of Venous Failure
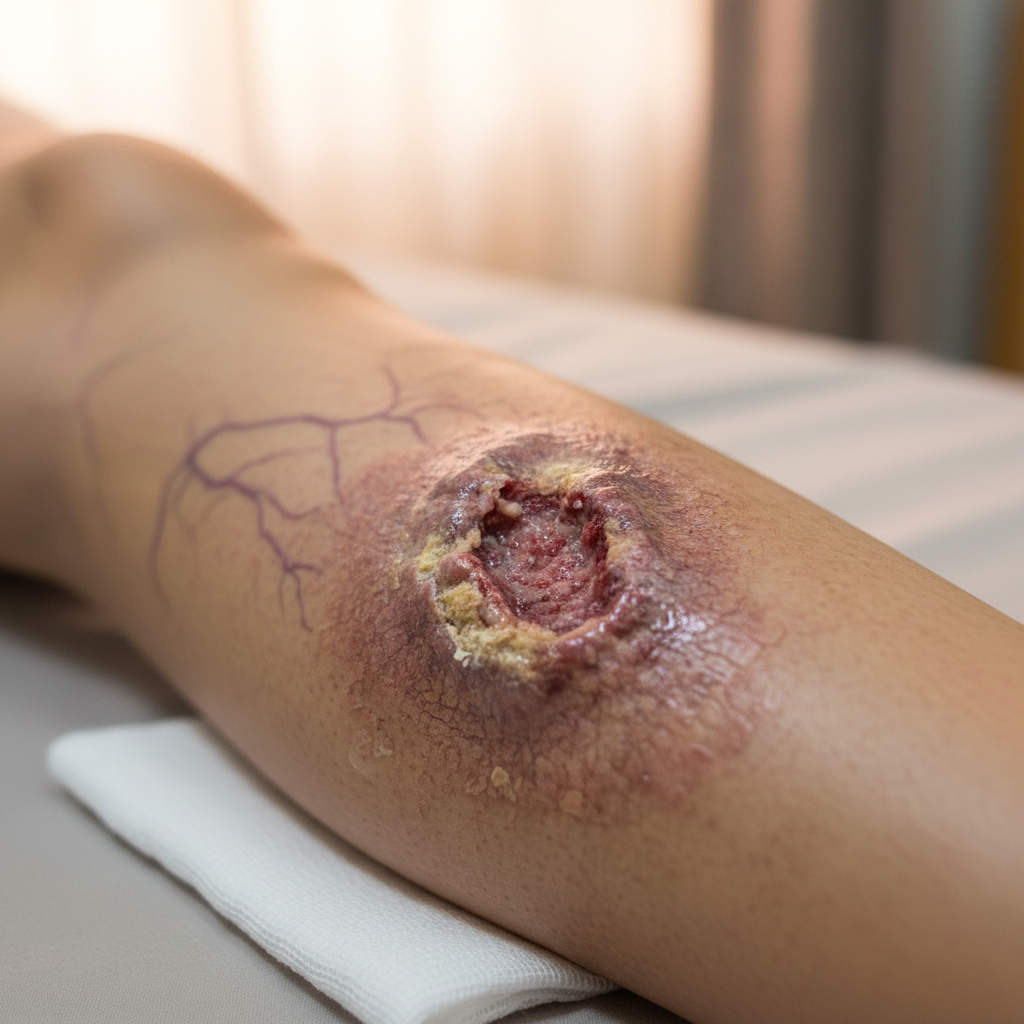
Venous leg ulcers represent the most severe manifestation of chronic venous insufficiency, developing as the end result of prolonged venous hypertension, tissue hypoxia, and inflammatory damage that ultimately overwhelms the skin's ability to maintain integrity. These ulcers typically develop in the "gaiter area" of the lower leg, most commonly around the medial malleolus where perforating vein incompetence creates the highest venous pressures. The ulceration process often begins with minor trauma to skin that has been weakened by chronic venous disease, but the underlying circulatory compromise prevents normal healing mechanisms from functioning effectively. Venous ulcers characteristically have irregular, shallow margins with a base of granulation tissue and moderate to heavy exudate production, reflecting the ongoing inflammatory process and impaired wound healing. The surrounding skin typically shows signs of chronic venous disease including hemosiderin staining, lipodermatosclerosis, and atrophie blanche, providing important clues to the underlying etiology. These ulcers are typically painless or only mildly painful, distinguishing them from arterial ulcers which are characteristically very painful. The healing process is prolonged and often complicated by secondary bacterial infection, contact dermatitis from topical treatments, and recurrent breakdown due to the persistent underlying venous pathology. Successful treatment requires comprehensive management of the underlying venous disease through compression therapy, wound care, and often surgical intervention to address incompetent veins and restore normal venous function.
9. Arterial Ulcers - Ischemic Tissue Death
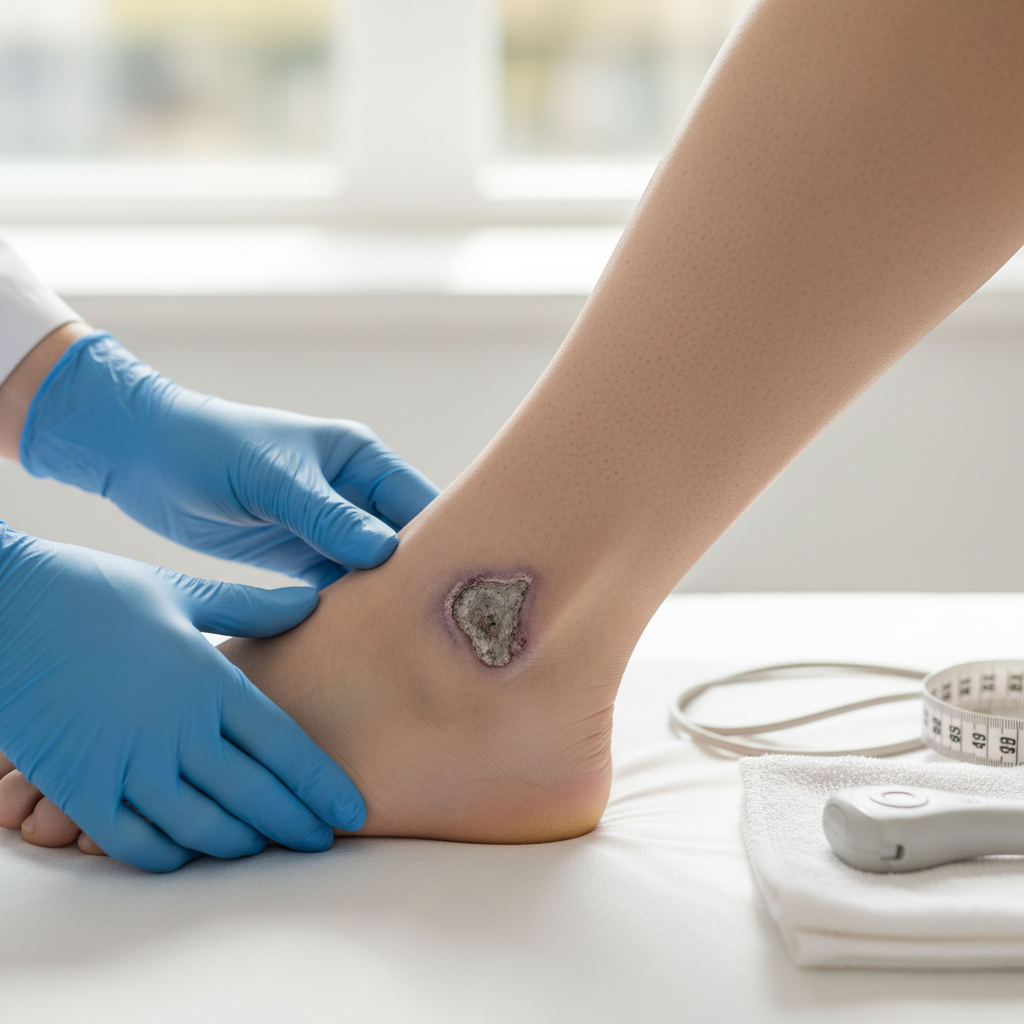
Arterial ulcers develop as a consequence of severe arterial insufficiency where tissue perfusion becomes inadequate to maintain cellular viability, resulting in ischemic necrosis and subsequent ulceration that reflects the critical nature of the underlying vascular compromise. These ulcers typically appear on pressure points such as the toes, heels, and lateral malleoli, where the combination of reduced blood flow and mechanical stress creates conditions conducive to tissue breakdown. Unlike venous ulcers, arterial ulcers characteristically have well-defined, "punched-out" margins with a pale or necrotic base that may contain black eschar, reflecting the ischemic nature of the tissue death. The surrounding skin shows classic signs of arterial insufficiency including pallor, coolness, hair loss, and nail dystrophy, providing important diagnostic clues to the underlying etiology. Pain is a prominent feature of arterial ulcers, often described as severe, constant, and worse at night when cardiac output naturally decreases, leading many patients to sleep with their legs dependent to maximize gravitational assistance to perfusion. The healing capacity of arterial ulcers is severely compromised due to the inadequate blood supply, with many ulcers remaining static or enlarging despite appropriate wound care unless arterial circulation is restored. The development of arterial ulcers indicates critical limb ischemia that requires urgent vascular evaluation and intervention to prevent limb loss. Treatment focuses primarily on revascularization through surgical or endovascular procedures, as topical wound care alone is insufficient when tissue perfusion is critically compromised.
10. Mixed Arterial-Venous Ulcers - The Complex Challenge
Mixed arterial-venous ulcers present a particularly challenging clinical scenario where both arterial insufficiency and venous disease contribute to ulcer development and impaired healing, creating a complex pathophysiology that requires careful evaluation and nuanced treatment approaches. These ulcers typically occur in patients with long-standing venous disease who have developed concurrent arterial compromise, often related to diabetes, smoking, or advanced age. The clinical presentation combines features of both arterial and venous ulceration, with irregular margins typical of venous disease but with poor granulation tissue and signs of ischemia characteristic of arterial insufficiency. The surrounding skin may show mixed findings including hemosiderin staining and lipodermatosclerosis from venous disease alongside pallor, coolness, and hair loss from arterial compromise. Pain characteristics can be variable, sometimes showing the severe pain typical of arterial ulcers but potentially modified by the presence of venous disease. The diagnostic challenge lies in determining the relative contribution of arterial versus venous pathology, as this significantly impacts treatment decisions, particularly regarding the use of compression therapy which is beneficial for venous disease but potentially harmful in the presence of significant arterial compromise. Ankle-brachial index measurements and additional vascular studies are essential for proper evaluation and treatment planning. Management requires addressing both components of the disease process, often necessitating arterial revascularization before aggressive venous treatment can be safely implemented. The prognosis for mixed ulcers is generally poorer than for pure venous or arterial ulcers, with higher rates of complications and limb loss.
11. Lymphedema and Skin Changes - When Drainage Fails

Lymphedema creates distinctive skin changes that reflect the progressive accumulation of protein-rich fluid in the interstitial spaces due to impaired lymphatic drainage, leading to chronic inflammation, fibrosis, and increased susceptibility to infection. The affected skin initially appears swollen and pits with pressure, but as the condition progresses, it develops a characteristic "peau d'orange" or orange peel texture due to the combination of edema and fibrotic changes in the dermis and subcutaneous tissue. The skin becomes progressively thicker and more indurated, eventually developing a woody consistency that no longer pits with pressure, indicating the transition from fluid accumulation to fibrotic tissue formation. Chronic lymphedema leads to hyperkeratosis, particularly prominent in the toe webs and dorsal foot, where the skin develops a warty, papillomatous appearance known as lymphostatic verrucosis. The impaired lymphatic function significantly compromises the skin's immune defense mechanisms, making patients extremely susceptible to bacterial and fungal infections that can trigger acute episodes of cellulitis or lymphangitis. These infectious episodes create a vicious cycle, as the inflammatory response further damages lymphatic vessels and worsens the underlying lymphedema. The skin changes in lymphedema are typically bilateral when due to systemic causes but may be unilateral when resulting from local lymphatic obstruction or damage. Recognition of these characteristic skin changes is crucial for early intervention with compression therapy and lymphatic drainage techniques that can prevent progression to the irreversible fibrotic stage of lymphedema.
12. Temperature and Color Changes - Thermal Indicators of Circulation
