12 Hair and Scalp Signs Worth Mentioning to Your Doctor
Your hair and scalp serve as remarkable indicators of your overall health, often revealing underlying conditions long before other symptoms manifest. While many people view hair concerns as purely cosmetic issues, medical professionals recognize that changes in hair texture, growth patterns, scalp condition, and hair loss can signal everything from nutritional deficiencies and hormonal imbalances to autoimmune disorders and serious systemic diseases. The hair follicle is one of the most metabolically active structures in the human body, making it particularly sensitive to internal changes and external stressors. Understanding which hair and scalp changes warrant medical attention can lead to early detection and treatment of various health conditions, potentially preventing more serious complications. This comprehensive guide explores twelve critical signs that should prompt a conversation with your healthcare provider, empowering you to take a proactive approach to your health through careful observation of these often-overlooked indicators.
1. Sudden or Rapid Hair Loss

Sudden or rapid hair loss, medically known as acute telogen effluvium, represents one of the most alarming hair-related symptoms that demands immediate medical attention. Unlike gradual hair thinning that occurs over months or years, sudden hair loss typically manifests as significant shedding within weeks, often leaving noticeable bald patches or overall thinning that becomes apparent during routine activities like shampooing or brushing. This condition can result from various triggers including severe physical or emotional stress, major surgery, high fever, rapid weight loss, medication changes, or underlying autoimmune conditions such as alopecia areata. The timing of sudden hair loss is crucial for diagnosis, as hair follicles typically enter the resting phase two to three months after a triggering event, meaning the actual cause may have occurred weeks before the visible hair loss begins. Medical evaluation becomes essential because sudden hair loss can indicate serious underlying conditions such as thyroid disorders, lupus, or even nutritional deficiencies that require specific treatment protocols. Early intervention often leads to better outcomes, as many causes of sudden hair loss are reversible when properly identified and treated promptly.
2. Persistent Scalp Itching and Irritation

Chronic scalp itching and irritation that persists despite proper hygiene and over-the-counter treatments often signals underlying dermatological or systemic conditions requiring professional medical evaluation. While occasional scalp itching may result from dry weather, product sensitivity, or temporary irritation, persistent symptoms lasting more than two weeks can indicate conditions such as seborrheic dermatitis, psoriasis, fungal infections, or contact dermatitis from hair care products or environmental allergens. The intensity and pattern of itching provide important diagnostic clues; for instance, itching accompanied by scaling and redness may suggest seborrheic dermatitis, while isolated patches of intense itching with hair loss could indicate alopecia areata or trichotillomania. Additionally, systemic conditions such as liver disease, kidney dysfunction, or certain autoimmune disorders can manifest as chronic scalp itching without obvious external signs. The psychological impact of persistent scalp itching should not be underestimated, as it can significantly affect sleep quality, concentration, and overall quality of life. Medical professionals can perform appropriate testing, including scalp biopsies or allergy testing when necessary, to identify the root cause and develop targeted treatment strategies that address both the symptoms and underlying condition.
3. Unusual Hair Texture Changes

Significant changes in hair texture that occur without obvious external causes often reflect internal health shifts that merit medical investigation. Hair texture encompasses various characteristics including diameter, curl pattern, porosity, and overall feel, all of which can be influenced by hormonal fluctuations, nutritional status, medication effects, and underlying health conditions. For example, previously straight hair becoming curly or wavy may indicate hormonal changes associated with pregnancy, menopause, or thyroid dysfunction, while coarse hair becoming fine and brittle could suggest hypothyroidism or nutritional deficiencies. Chemotherapy and certain medications can dramatically alter hair texture, sometimes permanently, but unexplained texture changes in the absence of known triggers warrant thorough evaluation. The protein structure of hair can be affected by autoimmune conditions, genetic disorders, and metabolic dysfunction, leading to changes in elasticity, strength, and appearance. Additionally, sudden changes in hair porosity—how well hair absorbs and retains moisture—can indicate damage to the hair cuticle from internal factors rather than external styling practices. Medical assessment becomes particularly important when texture changes are accompanied by other symptoms such as fatigue, weight changes, or skin alterations, as these combinations often point to systemic conditions requiring comprehensive treatment approaches.
4. Scalp Pain and Tenderness
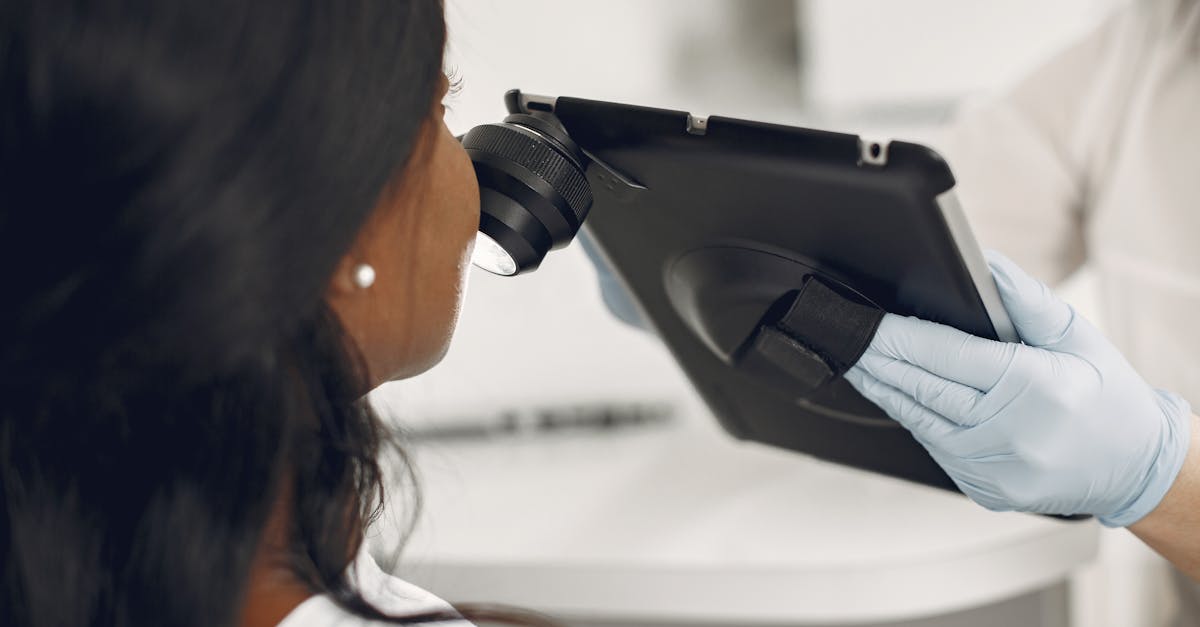
Scalp pain and tenderness, medically termed trichodynia, represents a complex symptom that can significantly impact daily life and often indicates underlying neurological, dermatological, or psychological conditions requiring professional evaluation. This condition manifests as burning, stinging, or aching sensations across the scalp surface, sometimes accompanied by increased sensitivity to touch, hair movement, or even light pressure from hats or headbands. The pain may be localized to specific areas or diffuse across the entire scalp, with intensity ranging from mild discomfort to severe, debilitating pain that interferes with sleep and daily activities. Potential causes include nerve inflammation, autoimmune conditions affecting the scalp, tension headaches with referred pain, fibromyalgia, or psychological stress manifesting as physical symptoms. Scalp pain can also result from tight hairstyles, chemical treatments, or underlying skin conditions, but persistent pain without obvious external causes requires medical investigation. The relationship between scalp pain and hair loss is particularly significant, as conditions like alopecia areata or central centrifugal cicatricial alopecia often present with both symptoms simultaneously. Healthcare providers may need to perform neurological examinations, skin biopsies, or psychological assessments to determine the root cause and develop appropriate treatment strategies that may include topical medications, nerve pain treatments, or stress management techniques.
5. Excessive Oiliness or Severe Dryness

Extreme changes in scalp oil production, whether excessive sebum secretion or severe dryness, often reflect hormonal imbalances, metabolic disorders, or dermatological conditions that require medical attention for proper diagnosis and treatment. The sebaceous glands in the scalp are highly responsive to hormonal fluctuations, particularly androgens like testosterone and dihydrotestosterone, making sudden changes in oil production potential indicators of endocrine disorders such as polycystic ovary syndrome (PCOS), thyroid dysfunction, or adrenal gland abnormalities. Excessive oiliness that develops suddenly or worsens dramatically may also signal seborrheic dermatitis, a chronic inflammatory condition that can lead to scaling, redness, and secondary bacterial or fungal infections if left untreated. Conversely, severe scalp dryness accompanied by flaking, tightness, or irritation may indicate autoimmune conditions like psoriasis or eczema, nutritional deficiencies affecting skin barrier function, or medication side effects. The impact of extreme oil production changes extends beyond cosmetic concerns, as both excessive oiliness and severe dryness can create environments conducive to secondary infections, inflammation, and hair follicle damage. Medical evaluation becomes essential when over-the-counter treatments fail to provide relief or when scalp oil changes are accompanied by other symptoms such as irregular menstrual cycles, unexplained weight changes, or mood alterations that suggest systemic hormonal imbalances requiring comprehensive treatment approaches.
6. Patches of Hair Loss or Bald Spots
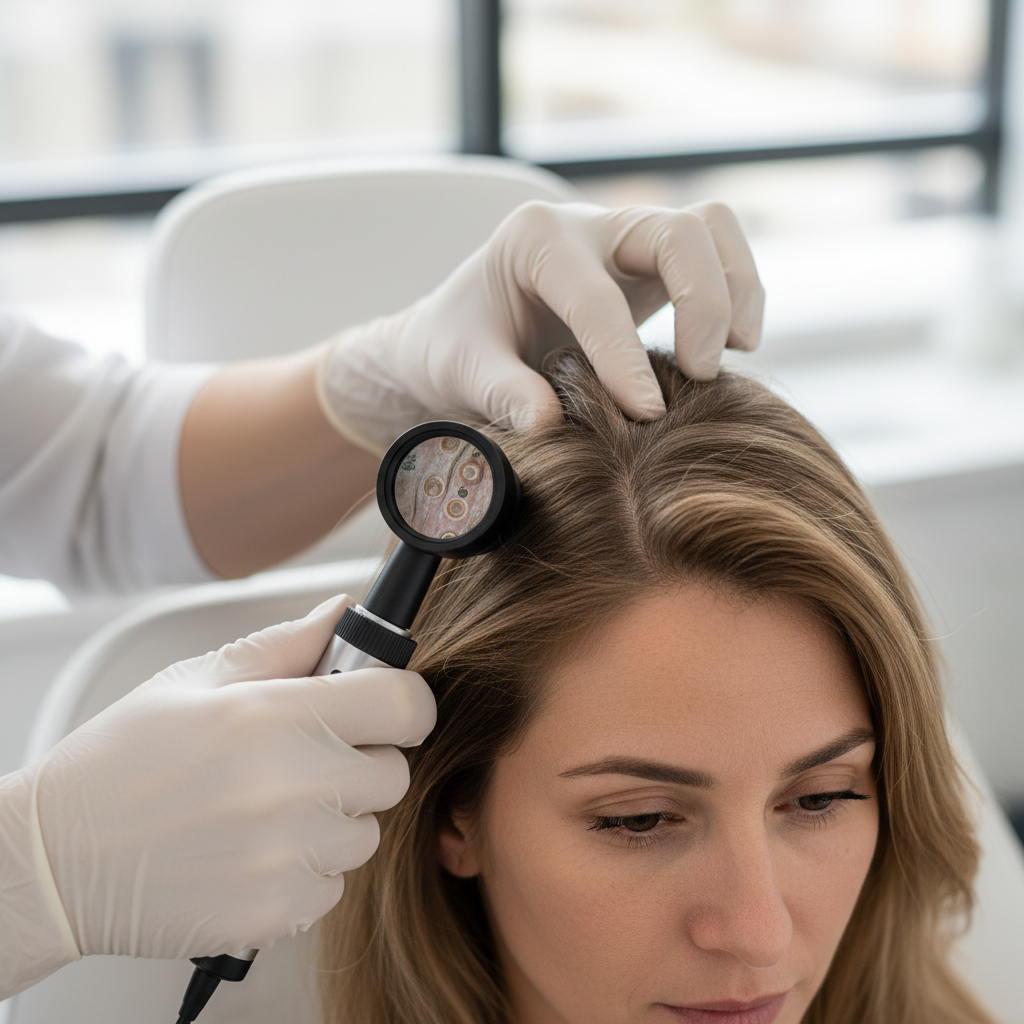
The development of distinct patches of hair loss or bald spots, particularly when they appear suddenly or in unusual patterns, represents a significant dermatological concern that demands immediate medical evaluation to prevent permanent hair loss and address potential underlying autoimmune or infectious conditions. Patchy hair loss most commonly results from alopecia areata, an autoimmune condition where the body's immune system mistakenly attacks hair follicles, creating smooth, round patches of complete hair loss that can appear anywhere on the scalp or body. The unpredictable nature of this condition, which can progress from small patches to total scalp hair loss (alopecia totalis) or complete body hair loss (alopecia universalis), makes early medical intervention crucial for implementing appropriate treatment strategies. Other causes of patchy hair loss include fungal infections such as tinea capitis, which is particularly common in children and can cause scaling, inflammation, and permanent scarring if not treated promptly with antifungal medications. Trichotillomania, a psychological condition involving compulsive hair pulling, creates irregular patches of hair loss with varying lengths of remaining hair, requiring both dermatological and psychological intervention. Central centrifugal cicatricial alopecia, more common in individuals of African descent, causes progressive patches of scarring hair loss that can be prevented from spreading with early medical treatment. The key to successful treatment lies in rapid diagnosis through appropriate testing, which may include scalp biopsies, fungal cultures, or blood tests to identify autoimmune markers.
7. Changes in Hair Growth Rate

Significant alterations in hair growth rate, whether dramatically slower or unusually rapid growth, often indicate underlying metabolic, hormonal, or nutritional imbalances that require medical investigation to identify and address root causes effectively. Normal hair growth occurs in cycles, with the anagen (growth) phase lasting two to seven years and producing approximately half an inch of growth per month, but various internal and external factors can disrupt this carefully regulated process. Dramatically slowed hair growth may signal hypothyroidism, a condition where insufficient thyroid hormone production affects cellular metabolism throughout the body, including hair follicles, leading to prolonged telogen (resting) phases and reduced overall hair production. Nutritional deficiencies, particularly inadequate protein intake, iron deficiency, or insufficient B vitamins, can significantly impact hair growth rates as follicles prioritize essential bodily functions over hair production during times of nutritional stress. Conversely, unusually rapid hair growth may indicate hyperthyroidism, certain medications, or hormonal fluctuations associated with pregnancy or puberty, though sudden acceleration in previously normal growth patterns warrants medical evaluation. Chronic illnesses, autoimmune conditions, and certain medications can also alter hair growth cycles, sometimes permanently, making it essential to document changes and seek professional assessment. Medical evaluation may include thyroid function tests, complete blood counts, nutritional assessments, and hormonal panels to identify treatable causes and develop appropriate intervention strategies that address both the symptoms and underlying health conditions.
8. Scalp Discoloration or Unusual Pigmentation

Abnormal scalp discoloration or unusual pigmentation changes represent potentially serious dermatological concerns that may indicate inflammatory conditions, infections, autoimmune disorders, or even malignant processes requiring immediate medical evaluation and appropriate diagnostic testing. Normal scalp coloration should match the surrounding skin tone, with any significant deviations such as persistent redness, purple or blue discoloration, unusual darkening, or white patches warranting professional assessment to rule out serious underlying conditions. Persistent red or inflamed areas may indicate chronic dermatitis, psoriasis, or seborrheic dermatitis, but they can also signal more serious conditions such as discoid lupus or other autoimmune disorders that can cause permanent scarring and hair loss if not treated promptly. Dark or hyperpigmented patches may result from post-inflammatory hyperpigmentation following previous scalp trauma or infection, but they can also indicate certain genetic conditions or medication side effects that require monitoring and management. White or depigmented areas may suggest vitiligo, an autoimmune condition affecting melanocytes, or could indicate scarring from previous inflammatory conditions or infections. Perhaps most concerning, irregular pigmented lesions, particularly those that are asymmetrical, have irregular borders, show color variation, or change over time, may represent melanoma or other skin cancers that require immediate biopsy and treatment. The scalp's frequent sun exposure and difficulty in self-examination make regular professional scalp evaluations essential, particularly for individuals with fair skin, family history of skin cancer, or previous history of abnormal moles or lesions.
9. Persistent Dandruff or Flaking
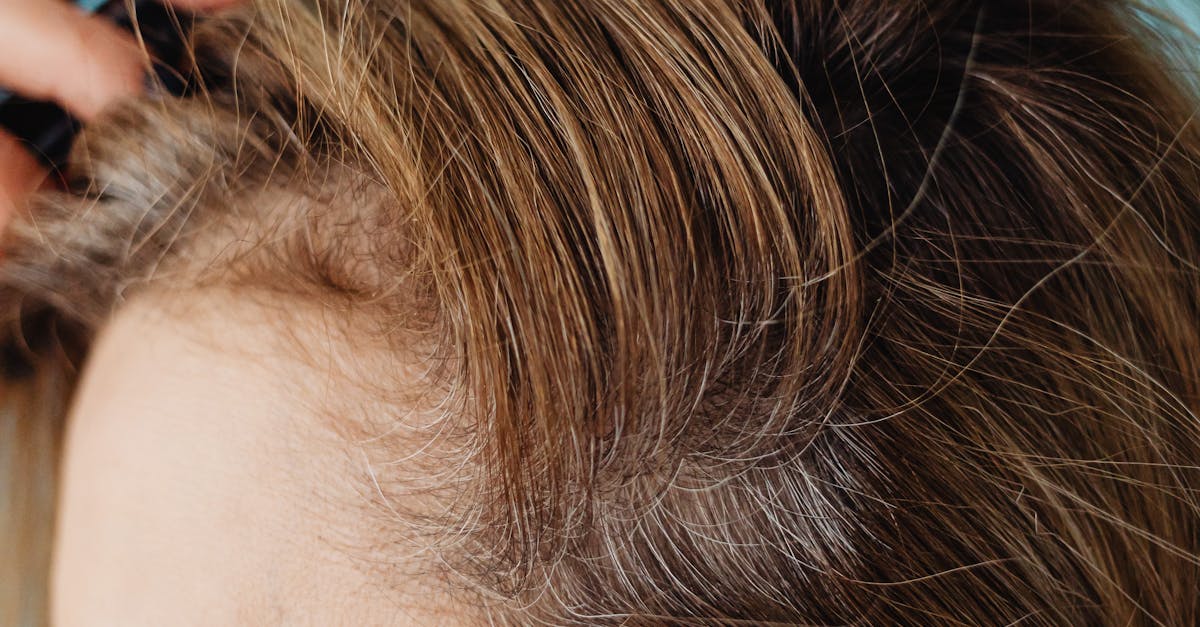
Chronic, persistent dandruff or scalp flaking that resists treatment with over-the-counter antidandruff shampoos often indicates underlying dermatological conditions such as seborrheic dermatitis, psoriasis, or fungal infections that require prescription treatments and professional medical management. While mild dandruff is common and typically responds well to zinc pyrithione or selenium sulfide shampoos, persistent flaking accompanied by inflammation, thick scales, or spreading to other body areas suggests more serious conditions requiring targeted therapy. Seborrheic dermatitis, characterized by yellowish, greasy scales and redness, results from an inflammatory response to Malassezia yeast overgrowth and often requires prescription antifungal treatments, topical corticosteroids, or calcineurin inhibitors for effective control. Scalp psoriasis presents with thick, silvery-white scales and well-defined red patches that may extend beyond the hairline onto the forehead, neck, or ears, requiring specialized treatments such as tar-based products, vitamin D analogs, or systemic medications for severe cases. The distinction between different causes of persistent flaking is crucial because treatment approaches vary significantly, and using inappropriate products can worsen certain conditions or delay proper healing. Additionally, chronic scalp inflammation from untreated flaking conditions can lead to secondary bacterial infections, permanent scarring, or hair loss, making early professional intervention essential. Medical evaluation may include microscopic examination of scale samples, fungal cultures, or skin biopsies to establish accurate diagnoses and develop effective treatment protocols that address both the underlying condition and associated symptoms.
10. Hair Becoming Brittle or Breaking Easily

Hair that becomes increasingly brittle, fragile, or prone to breakage without obvious external damage often reflects internal health issues, nutritional deficiencies, or hormonal imbalances that require medical evaluation to prevent progressive hair loss and address underlying systemic conditions. Healthy hair possesses natural elasticity and strength due to its protein structure, primarily composed of keratin, but various internal factors can compromise this structural integrity, leading to increased fragility and breakage. Thyroid disorders, particularly hypothyroidism, commonly cause hair to become dry, brittle, and prone to breakage as reduced thyroid hormone levels affect protein synthesis and cellular metabolism throughout the body, including hair follicles. Nutritional deficiencies, especially inadequate protein intake, iron deficiency, or insufficient biotin and other B vitamins, can significantly impact hair strength and elasticity as the body prioritizes essential functions over hair production during periods of nutritional stress. Autoimmune conditions such as lupus or alopecia areata can cause sudden changes in hair texture and strength, while certain medications, including chemotherapy drugs, blood thinners, and some antidepressants, can alter hair structure and increase breakage susceptibility. The pattern and location of hair breakage provide important diagnostic clues; for instance, breakage near the scalp may indicate new growth problems, while mid-shaft breakage might suggest external damage or internal health issues affecting existing hair. Medical assessment may include blood tests to evaluate thyroid function, nutritional status, and autoimmune markers, along with microscopic hair analysis to determine the cause and develop appropriate treatment strategies.
11. Unusual Odors from the Scalp
Persistent, unusual odors emanating from the scalp that cannot be eliminated through regular washing and proper hygiene practices often indicate underlying infections, metabolic disorders, or dermatological conditions requiring professional medical evaluation and targeted treatment approaches. A healthy scalp should have minimal odor even between washings, as natural sebum production and normal bacterial flora typically do not create offensive smells when proper hygiene is maintained. Strong, persistent odors may result from bacterial overgrowth, particularly when excessive sweating, poor air circulation, or compromised immune function creates favorable conditions for pathogenic organisms to flourish on the scalp surface. Fungal infections, including tinea capitis or severe seborrheic dermatitis with secondary Malassezia overgrowth, can produce distinctive musty or yeasty odors that persist despite thorough cleansing and may be accompanied by scaling, inflammation, or hair loss. Certain metabolic disorders can cause unusual body odors, including scalp odors, as the body attempts to eliminate toxins or metabolic byproducts through the skin, making persistent scalp odors potential indicators of liver dysfunction, kidney disease, or diabetes. Additionally, some medications, dietary factors, or hormonal changes can alter normal body chemistry and create unusual odors that may be most noticeable in areas with high sebaceous gland concentration like the scalp. The social and psychological impact of persistent scalp odors can be significant, affecting self-confidence and interpersonal relationships, making prompt medical evaluation essential for both physical and emotional well-being. Professional assessment may include bacterial and fungal cultures, blood tests to evaluate organ function, and careful medication review to identify and treat the underlying cause effectively.
12. Premature Graying or Color Changes

Premature graying or unexpected hair color changes, particularly when occurring before age 30 in Caucasians or before age 20 in other ethnicities, may indicate underlying autoimmune conditions, nutritional deficiencies, genetic disorders, or systemic health issues that warrant medical investigation and potential intervention. While genetics primarily determine the timing of natural graying through the gradual reduction of melanocyte activity in hair follicles, premature or sudden color changes can signal various health conditions requiring professional evaluation. Autoimmune disorders such as vitiligo, alopecia areata, or thyroid dysfunction can accelerate the graying process or cause patchy color loss as the immune system targets melanin-producing cells in hair follicles. Nutritional deficiencies, particularly vitamin B12, folate, copper, or iron deficiency, can affect melanin production and lead to premature graying that may be reversible with appropriate supplementation and dietary modifications. Certain genetic conditions, including Werner syndrome or progeria, cause accelerated aging processes that include very early graying, while some medications, chemotherapy treatments, or exposure to certain chemicals can temporarily or permanently alter hair pigmentation. The pattern of color change provides important diagnostic information; for instance, diffuse graying suggests systemic causes, while patchy color loss may indicate autoimmune conditions or localized inflammation. Additionally, sudden color changes in previously stable hair may indicate recent health events, medication changes, or