12 Elbow Skin Changes That Correspond to Psoriasis and Nutritional Deficiencies
The elbows, often overlooked in routine health assessments, serve as remarkable indicators of both autoimmune conditions and nutritional status. These prominent joint areas, subjected to constant friction and mechanical stress, frequently manifest the earliest and most pronounced signs of psoriasis while simultaneously revealing deficiencies in essential vitamins and minerals. The unique anatomy of elbow skin, characterized by thicker epidermis and reduced sebaceous gland activity, creates an environment where inflammatory processes and nutritional inadequacies become visibly apparent before affecting other body regions. Understanding the intricate relationship between elbow skin changes, psoriatic manifestations, and nutritional deficiencies provides healthcare professionals and individuals with a powerful diagnostic tool for early intervention. This comprehensive exploration examines twelve distinct elbow skin changes that serve as reliable markers for psoriasis progression and specific nutritional gaps, offering insights into the complex interplay between immune dysfunction, metabolic processes, and dermatological manifestations. By recognizing these patterns, we can better understand how systemic health issues manifest through localized skin changes, ultimately leading to more effective treatment strategies and improved patient outcomes.
1. Silvery Scale Formation - The Hallmark of Psoriatic Activity
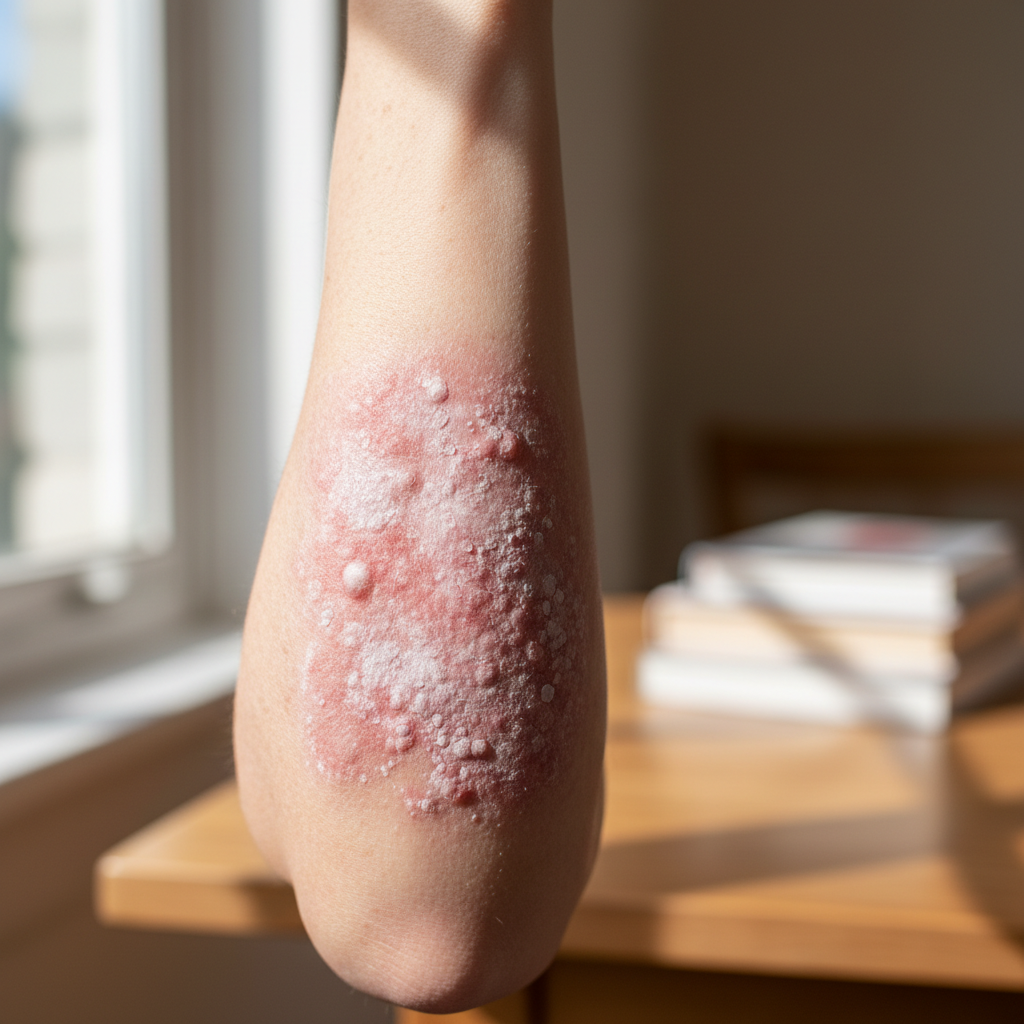
Silvery scale formation on the elbows represents the most characteristic and recognizable sign of psoriatic involvement, resulting from the accelerated turnover of keratinocytes that occurs in this autoimmune condition. These distinctive scales, which appear as thick, adherent, silvery-white plaques, develop when the normal 28-day skin cell cycle accelerates to just 3-4 days, causing immature cells to accumulate on the surface before proper maturation can occur. The scales typically begin as small, discrete patches that gradually expand and coalesce, creating larger plaques with well-defined borders and a characteristic "candle wax" appearance when gently scraped. Research indicates that the severity and extent of scale formation correlates directly with the degree of underlying inflammation and can serve as a reliable marker for disease activity and treatment response. The presence of silvery scales specifically on the elbows, combined with similar manifestations on knees and scalp, strongly suggests psoriatic involvement rather than other inflammatory skin conditions. Interestingly, the thickness and adherence of these scales can also indicate concurrent nutritional deficiencies, particularly zinc and vitamin D, which play crucial roles in normal skin cell differentiation and immune regulation. Understanding the formation mechanism of these scales helps distinguish psoriatic changes from other scaling conditions and guides appropriate therapeutic interventions.
2. Erythematous Plaques - Inflammatory Markers of Immune Dysregulation
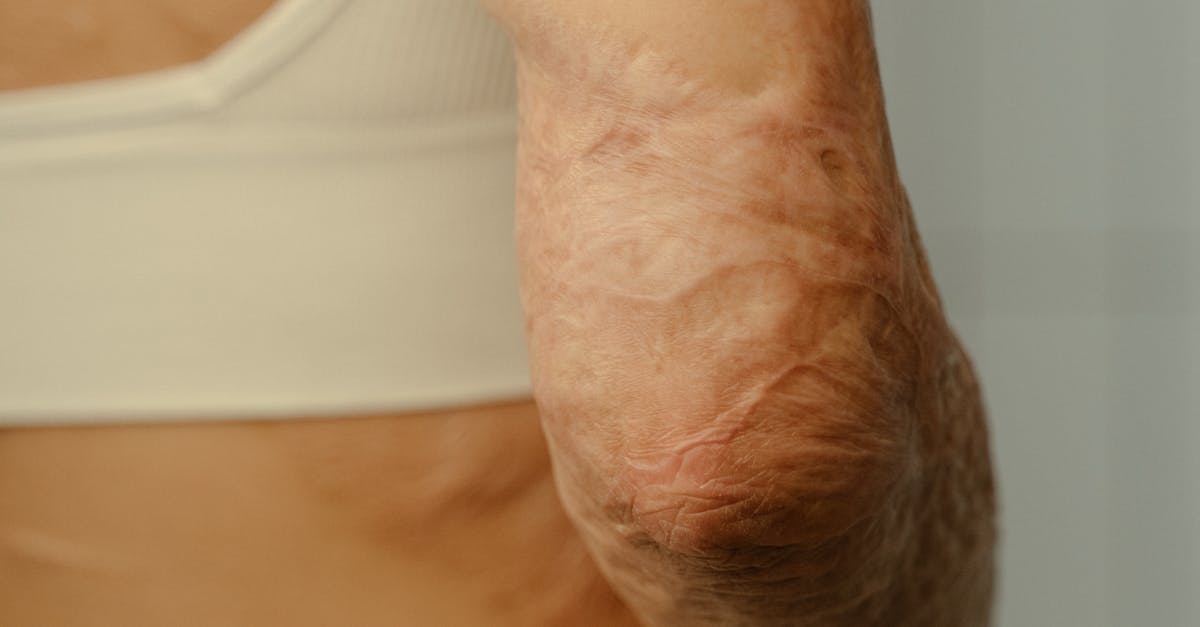
Erythematous plaques on the elbows manifest as well-demarcated, raised, red lesions that indicate active inflammatory processes characteristic of psoriatic disease progression. These inflammatory patches typically present with a distinctive salmon-pink to deep red coloration, reflecting the increased blood flow and immune cell infiltration occurring within the affected tissue. The plaques often exhibit a symmetrical distribution pattern, appearing on both elbows simultaneously, which distinguishes psoriatic involvement from other unilateral inflammatory conditions or contact dermatitis. The erythema results from vasodilation and increased vascular permeability triggered by inflammatory mediators, including tumor necrosis factor-alpha, interleukins, and interferon-gamma, which are characteristically elevated in psoriatic patients. Clinical observation reveals that the intensity of erythema often correlates with disease activity and can fluctuate based on various triggers, including stress, infections, medications, and seasonal changes. Nutritional factors significantly influence the severity of erythematous manifestations, with deficiencies in omega-3 fatty acids, vitamin E, and antioxidants potentially exacerbating inflammatory responses and prolonging plaque persistence. The raised nature of these plaques, combined with their persistent erythematous appearance, helps differentiate psoriatic lesions from other inflammatory skin conditions such as eczema or seborrheic dermatitis, which typically present with different morphological characteristics and distribution patterns.
3. Hyperkeratosis and Thickened Skin - Protective Responses Gone Awry

Hyperkeratosis, characterized by abnormal thickening of the stratum corneum on elbow surfaces, represents a protective mechanism that becomes pathologically exaggerated in psoriatic conditions and certain nutritional deficiency states. This thickening occurs as the skin attempts to protect underlying tissues from chronic inflammation and mechanical trauma, but the process becomes dysregulated in psoriasis, leading to excessive keratin production and accumulation. The hyperkeratotic changes typically manifest as rough, thickened patches with a leathery texture that may appear grayish or yellowish in color, depending on the degree of scale accumulation and underlying inflammation. Vitamin A deficiency significantly contributes to hyperkeratotic changes, as this essential nutrient plays a crucial role in regulating keratinocyte differentiation and maintaining normal skin barrier function. Research demonstrates that inadequate vitamin A levels lead to abnormal keratinization processes, resulting in follicular hyperkeratosis and generalized skin thickening that can mimic or exacerbate psoriatic manifestations. Additionally, zinc deficiency can contribute to hyperkeratotic changes by impairing normal wound healing processes and cellular turnover regulation. The combination of psoriatic inflammation and nutritional deficiencies creates a synergistic effect, where hyperkeratosis becomes more pronounced and resistant to treatment. Understanding these underlying mechanisms helps clinicians develop comprehensive treatment approaches that address both the autoimmune component and nutritional factors contributing to abnormal skin thickening.
4. Fissuring and Cracking - When Skin Barrier Function Fails
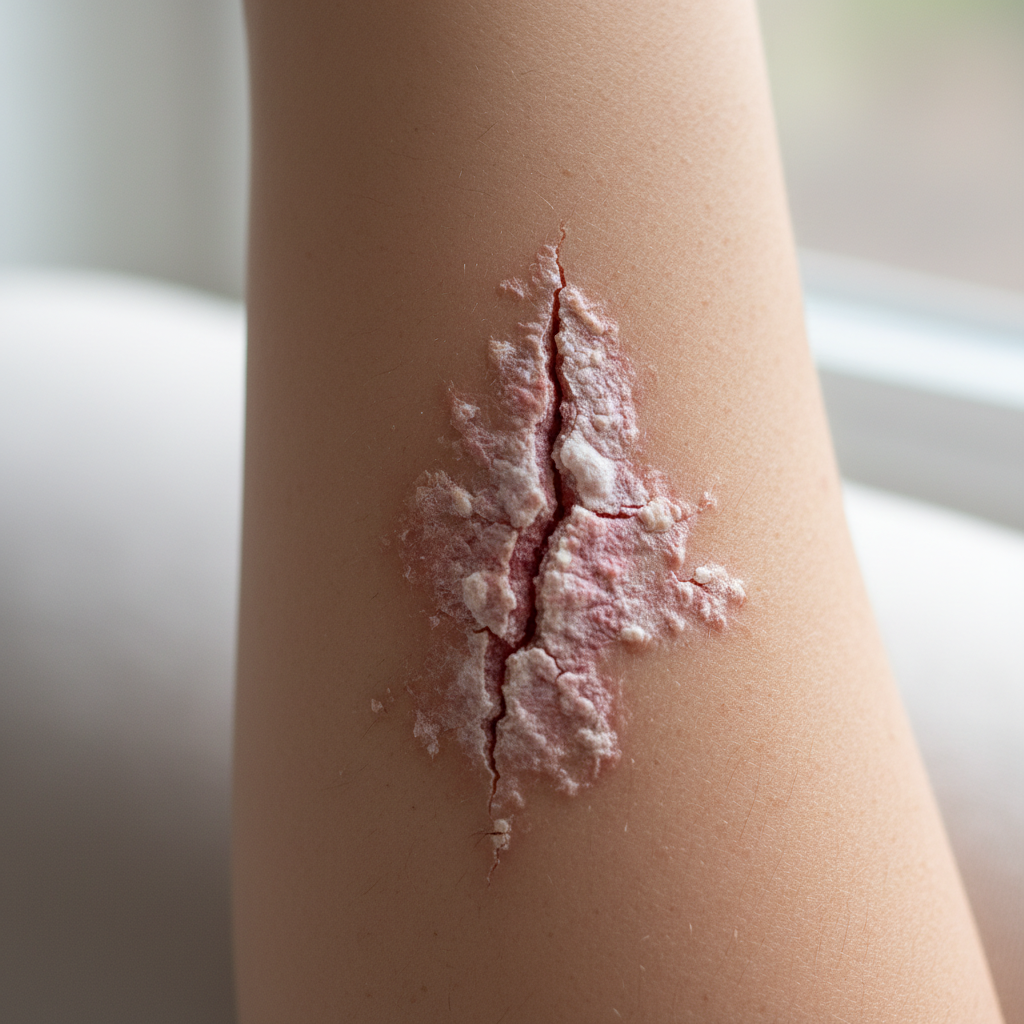
Fissuring and cracking of elbow skin represents a critical breakdown in barrier function that commonly occurs in advanced psoriatic lesions and is significantly exacerbated by specific nutritional deficiencies. These painful linear breaks in the skin surface develop when the normal elasticity and integrity of the stratum corneum become compromised due to chronic inflammation, excessive dryness, and impaired healing processes. The fissures typically appear as deep, linear cracks that may extend through multiple skin layers, creating potential entry points for bacterial infections and causing significant discomfort during elbow movement. Essential fatty acid deficiencies, particularly omega-3 and omega-6 fatty acids, play a crucial role in fissure development by compromising the skin's lipid barrier and reducing its ability to maintain adequate hydration levels. Vitamin E deficiency further contributes to fissuring by impairing the skin's antioxidant defense mechanisms and reducing its ability to repair oxidative damage caused by chronic inflammation. The mechanical stress placed on elbow skin during daily activities exacerbates fissure formation, particularly when the skin lacks the flexibility provided by adequate nutrition and proper barrier function. Biotin deficiency has also been associated with increased skin fragility and fissuring, as this B-vitamin is essential for fatty acid synthesis and maintaining skin structural integrity. Clinical management of fissuring requires addressing both the underlying psoriatic inflammation and correcting nutritional deficiencies to restore proper barrier function and promote healing.
5. Hyperpigmentation Patterns - Post-Inflammatory Color Changes

Hyperpigmentation patterns on the elbows frequently develop as a consequence of chronic psoriatic inflammation and can be significantly influenced by underlying nutritional deficiencies that affect melanin production and skin healing processes. These darkened areas typically appear as brown to black patches that persist long after active inflammation has subsided, representing post-inflammatory hyperpigmentation (PIH) that results from increased melanin deposition in response to chronic tissue damage. The hyperpigmentation often follows the distribution pattern of previous psoriatic plaques, creating a map-like appearance that can help clinicians trace the historical progression of the disease. Vitamin C deficiency significantly impacts hyperpigmentation development by impairing collagen synthesis and reducing the skin's ability to repair inflammatory damage effectively, leading to prolonged healing times and increased melanin deposition. Iron deficiency can paradoxically contribute to both hyperpigmentation and hypopigmentation patterns, depending on the severity and duration of the deficiency, as iron plays a crucial role in melanin synthesis pathways. Folate and vitamin B12 deficiencies have been associated with altered pigmentation patterns, as these nutrients are essential for DNA synthesis and cellular repair processes that regulate melanocyte function. The persistence of hyperpigmentation can serve as a marker for inadequate nutritional support during the healing process and may indicate the need for targeted supplementation to promote proper skin recovery. Understanding these pigmentation changes helps differentiate between active psoriatic lesions and residual post-inflammatory changes, guiding appropriate treatment decisions.
6. Lichenification - Chronic Scratching and Skin Adaptation

Lichenification of elbow skin represents a chronic adaptive response to persistent itching and scratching that commonly accompanies psoriatic lesions and can be exacerbated by specific nutritional deficiencies affecting nerve function and skin sensitivity. This condition manifests as thickened, leathery skin with accentuated skin markings that develop in response to repeated mechanical trauma from scratching and rubbing. The lichenified areas typically appear darker than surrounding skin and feel rough to the touch, with prominent skin lines creating a characteristic "bark-like" texture that distinguishes it from other forms of skin thickening. Magnesium deficiency contributes significantly to lichenification development by affecting nerve function and increasing skin sensitivity, leading to more intense itching sensations and subsequent scratching behaviors. The deficiency also impairs muscle relaxation and stress response, potentially increasing the frequency and intensity of scratching episodes during periods of psychological stress. B-vitamin complex deficiencies, particularly B6 and B12, can exacerbate lichenification by affecting peripheral nerve function and altering pain and itch perception thresholds. The chronic nature of lichenification creates a self-perpetuating cycle where thickened skin becomes more sensitive to irritation, leading to continued scratching and further skin changes. Histamine metabolism can also be affected by nutritional deficiencies, particularly vitamin C and quercetin, leading to increased allergic responses and heightened itch sensations that contribute to lichenification development.
7. Atrophic Changes - When Skin Becomes Thin and Fragile

Atrophic changes in elbow skin, characterized by thinning and increased fragility, can occur in certain forms of psoriasis and are significantly influenced by nutritional deficiencies that affect collagen synthesis and skin structural integrity. These changes typically manifest as areas where the skin appears translucent, with visible blood vessels and a papery texture that tears easily with minimal trauma. Atrophy can develop in areas of chronic psoriatic inflammation where repeated cycles of tissue damage and repair have depleted the skin's regenerative capacity, particularly when adequate nutritional support is lacking. Vitamin C deficiency plays a central role in atrophic changes by impairing collagen synthesis, as this vitamin serves as an essential cofactor for hydroxylation reactions required in collagen formation. Protein malnutrition significantly contributes to skin atrophy by limiting the availability of amino acids necessary for tissue repair and maintenance, leading to progressive thinning and loss of skin elasticity. Copper deficiency affects elastin and collagen cross-linking, resulting in weakened skin structure and increased susceptibility to atrophic changes, particularly in areas subjected to mechanical stress like the elbows. Zinc deficiency further compounds atrophic changes by impairing wound healing processes and reducing the skin's ability to maintain normal thickness and integrity. The development of atrophic changes in psoriatic patients often indicates a need for comprehensive nutritional assessment and intervention to support tissue repair and prevent further deterioration. Recognition of these changes is crucial for adjusting treatment approaches and preventing complications such as skin tears and delayed wound healing.
8. Follicular Involvement - Hair Follicle Changes and Keratosis Pilaris

Follicular involvement around the elbow area represents a distinct manifestation that can occur in psoriatic conditions and is significantly influenced by vitamin A deficiency and other nutritional factors affecting hair follicle function. This involvement typically presents as small, rough bumps surrounding hair follicles, creating a characteristic "goose bump" appearance that persists even in warm conditions. The follicular changes result from abnormal keratinization processes within hair follicles, leading to the formation of keratin plugs that block follicular openings and create raised, rough-textured lesions. Vitamin A deficiency is the primary nutritional factor contributing to follicular hyperkeratosis, as this vitamin is essential for regulating epithelial cell differentiation and maintaining normal follicular function. The deficiency leads to increased keratin production and impaired desquamation, causing keratin plugs to form and creating the characteristic rough texture associated with keratosis pilaris. Essential fatty acid deficiencies also contribute to follicular involvement by affecting the composition of sebaceous secretions and impairing the skin's barrier function around hair follicles. Biotin deficiency can exacerbate follicular changes by affecting keratin synthesis and hair follicle health, leading to increased fragility and abnormal keratinization patterns. The combination of psoriatic inflammation and nutritional deficiencies creates an environment where follicular involvement becomes more pronounced and widespread. Clinical recognition of follicular changes helps identify patients who may benefit from vitamin A supplementation and comprehensive nutritional support to restore normal follicular function and improve overall skin health.
9. Vascular Changes - Dilated Capillaries and Telangiectasias
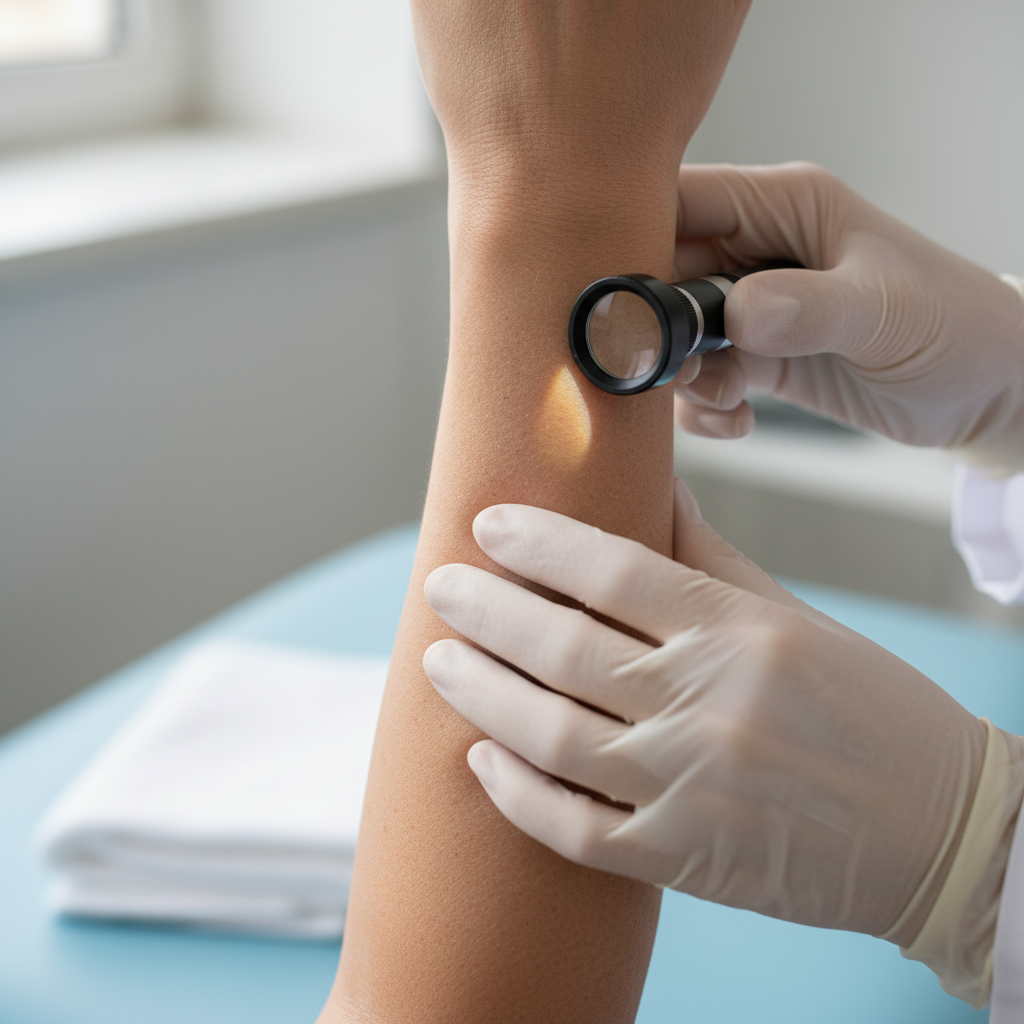
Vascular changes in elbow skin, including dilated capillaries and telangiectasias, reflect the chronic inflammatory state characteristic of psoriasis and can be influenced by nutritional factors affecting vascular integrity and function. These changes typically manifest as small, visible blood vessels that appear as red or purple lines beneath the skin surface, particularly noticeable in areas where psoriatic inflammation has been chronic or severe. The vascular dilation results from persistent inflammatory mediator release, which causes chronic vasodilation and eventual structural changes in capillary walls, leading to permanent vessel visibility. Vitamin C deficiency significantly contributes to vascular fragility by impairing collagen synthesis in blood vessel walls, making capillaries more susceptible to dilation and rupture under inflammatory stress. Bioflavonoid deficiencies, particularly rutin and hesperidin, affect capillary strength and permeability, leading to increased vascular fragility and more prominent telangiectasias in areas of chronic inflammation. Vitamin K deficiency can contribute to vascular changes by affecting blood clotting mechanisms and vascular wall integrity, potentially leading to increased bleeding and bruising in affected areas. The presence of prominent vascular changes in psoriatic elbow lesions often indicates chronic, poorly controlled inflammation and may suggest the need for more aggressive anti-inflammatory treatment approaches. Copper deficiency affects elastin synthesis in blood vessel walls, contributing to loss of vascular elasticity and increased susceptibility to permanent dilation. Understanding these vascular changes helps clinicians assess disease severity and duration while identifying patients who may benefit from vascular-supportive nutritional interventions.
10. Nail Changes - Pitting, Ridging, and Discoloration

Nail changes affecting the fingers and toes often accompany elbow psoriasis and provide important diagnostic clues while reflecting underlying nutritional deficiencies that affect nail matrix function and keratin production. These changes typically include pitting (small depressions in the nail surface), horizontal and vertical ridging, discoloration ranging from yellow to brown, and onycholysis (separation of the nail from the nail bed). Nail pitting occurs in approximately 50% of psoriatic patients and results from inflammatory involvement of the nail matrix, creating characteristic small depressions that appear randomly across the nail surface. Zinc deficiency significantly contributes to nail abnormalities by impairing keratin synthesis and nail matrix function, leading to white spots, horizontal ridges (Beau's lines), and increased nail fragility. Iron deficiency affects nail health by reducing oxygen delivery to nail tissues and impairing cellular metabolism, resulting in spoon-shaped nails (koilonychia), pale nail beds, and increased brittleness. Biotin deficiency specifically affects nail keratin production, leading to soft, easily breakable nails with vertical ridging and splitting. Protein malnutrition impacts nail growth and strength by limiting amino acid availability for keratin synthesis, resulting in thin, weak nails with horizontal ridges marking periods of nutritional inadequacy. Silicon deficiency affects nail hardness and strength by impairing the cross-linking processes that provide structural integrity to nail keratin. The combination of psoriatic inflammation and nutritional deficiencies creates a synergistic effect where nail changes become more pronounced and persistent, often serving as indicators of both disease activity and nutritional status.
11. Pruritus and Sensory Changes - The Itch-Scratch Cycle
Pruritus (itching) represents one of the most distressing symptoms associated with elbow psoriasis and can be significantly influenced by nutritional deficiencies affecting nerve function, histamine metabolism, and skin barrier integrity. The itching sensation in psoriatic lesions results from inflammatory mediator release, nerve sensitization, and compromised skin barrier function, creating an intense urge to scratch that can perpetuate the inflammatory cycle. Magnesium deficiency contributes to increased skin sensitivity and nerve hyperexcitability, potentially intensifying itching sensations and making them more difficult to control through standard treatments. The deficiency affects nerve membrane stability and neurotransmitter function, leading to altered pain and itch perception that can make psoriatic itching more severe and persistent. Vitamin D deficiency has been associated with increased pruritus in psoriatic patients, as this vitamin plays important roles in immune regulation and skin barrier function, with deficiency potentially exacerbating inflammatory responses and skin sensitivity. Omega-3 fatty acid deficiencies contribute to pruritus by affecting inflammatory mediator production and skin barrier lipid composition, leading to increased skin dryness and sensitivity to irritants. Histidine deficiency can affect histamine metabolism and contribute to increased allergic responses and itching, particularly in patients with concurrent allergic sensitivities. The itch-scratch cycle creates additional complications by causing mechanical trauma to already inflamed skin, leading to further barrier disruption and potential secondary bacterial infections. B-vitamin