10 Tongue Characteristics That Reflect Overall Health
The human tongue serves as far more than a simple organ for taste and speech—it functions as a remarkable diagnostic window into your overall health status. For thousands of years, traditional medicine practitioners across cultures have examined the tongue as a primary method of health assessment, recognizing patterns and characteristics that modern science now validates through research. This small but mighty muscle, covered in specialized tissue and rich with blood vessels, nerve endings, and lymphatic drainage, reflects systemic conditions ranging from nutritional deficiencies to autoimmune disorders, infections, and cardiovascular issues. Medical professionals today increasingly recognize that tongue examination can reveal early warning signs of diabetes, liver disease, kidney dysfunction, and even certain cancers. The tongue's appearance, texture, color, coating, and movement patterns provide valuable insights that complement traditional diagnostic methods. Understanding these ten key tongue characteristics empowers individuals to become more aware of their health status and seek appropriate medical attention when concerning changes occur, making tongue self-examination an invaluable tool for preventive healthcare.
1. Color Variations - The Spectrum of Health Indicators

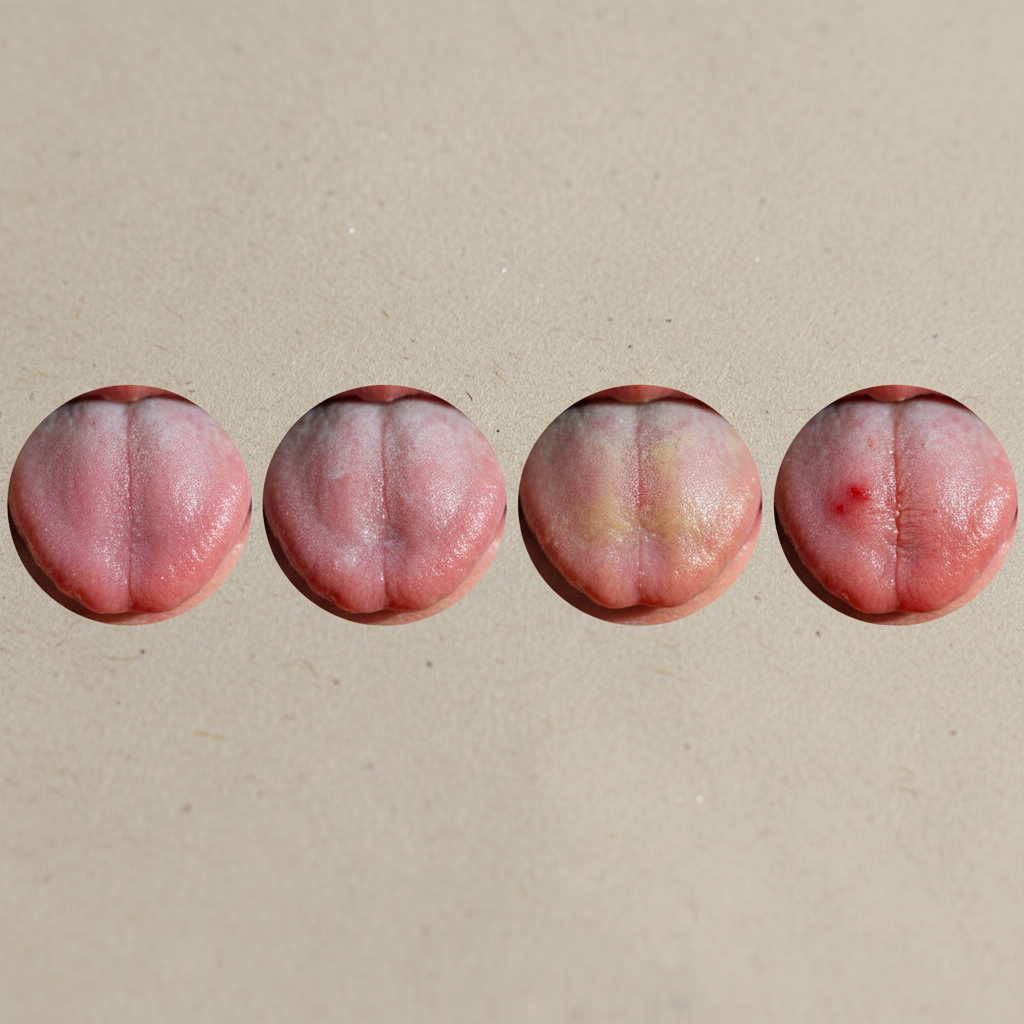
The natural color of a healthy tongue ranges from light pink to slightly reddish-pink, indicating proper circulation and oxygenation throughout the body. However, significant deviations from this baseline can signal various health conditions that require attention. A pale or white tongue often indicates anemia, poor circulation, or nutritional deficiencies, particularly iron, vitamin B12, or folate deficiency, which affects red blood cell production and oxygen transport. Conversely, a bright red or strawberry-colored tongue may suggest vitamin deficiencies, particularly B vitamins, or conditions like scarlet fever, Kawasaki disease, or geographic tongue syndrome. A blue or purple-tinged tongue typically indicates poor oxygenation or circulation problems, potentially signaling heart disease, lung conditions, or blood disorders. Yellow discoloration often accompanies liver dysfunction, jaundice, or certain bacterial infections, while a black or dark brown tongue can result from poor oral hygiene, certain medications, smoking, or rarely, a condition called black hairy tongue. Gray coloration may indicate digestive issues or chronic illness. These color changes serve as early warning systems, prompting individuals to seek medical evaluation before more serious symptoms develop, making tongue color assessment a valuable screening tool for systemic health monitoring.
2. Texture and Surface Irregularities - Reading the Topographical Map

The surface texture of your tongue provides crucial information about your nutritional status, hydration levels, and underlying health conditions. A healthy tongue maintains a relatively smooth surface with small, evenly distributed papillae (tiny bumps) that house taste buds and provide the tongue's characteristic texture. When the tongue becomes unusually smooth or glossy, it often indicates atrophic glossitis, commonly associated with nutritional deficiencies, particularly vitamin B12, iron, or folate deficiency, which can also suggest pernicious anemia or celiac disease. Conversely, an overly rough or bumpy texture may indicate inflammation, allergic reactions, or geographic tongue, a benign condition characterized by irregular patches. Deep grooves or fissures running across the tongue surface, known as fissured tongue, can be genetic but may also indicate dehydration, nutritional deficiencies, or autoimmune conditions like Sjögren's syndrome. Raised, white or red patches with irregular borders might suggest leukoplakia or erythroplakia, potentially precancerous conditions requiring immediate medical evaluation. Small, painful ulcers or sores can indicate stress, nutritional deficiencies, autoimmune disorders, or viral infections. The texture changes often correlate with systemic inflammation levels, making regular tongue texture assessment valuable for monitoring overall health status and identifying conditions before they progress to more serious stages.
3. Coating Thickness and Distribution - Decoding the Body's Waste System

The presence, thickness, and distribution of coating on the tongue surface provide valuable insights into digestive health, immune function, and the body's detoxification processes. A thin, light coating is normal and indicates healthy digestive function, while significant changes in coating characteristics often reflect systemic imbalances. A thick, white coating typically suggests poor digestion, candida overgrowth, dehydration, or respiratory infections, while also potentially indicating that the body is working to eliminate toxins through increased bacterial activity. Yellow coating often correlates with liver dysfunction, gallbladder issues, or bacterial infections, particularly when accompanied by bad breath or digestive discomfort. Brown or black coating may indicate serious digestive problems, poor oral hygiene, smoking effects, or certain medications, while also potentially signaling kidney dysfunction or severe dehydration. The distribution pattern matters significantly—coating concentrated at the tongue's base often indicates digestive issues in the lower gastrointestinal tract, while coating near the tip may suggest upper digestive problems or respiratory issues. Patchy coating distribution can indicate geographic tongue or nutritional imbalances. Traditional Chinese Medicine associates different coating patterns with specific organ systems, and modern research increasingly validates these connections, particularly regarding digestive health markers. Regular monitoring of tongue coating changes can help identify digestive problems, infections, or systemic illness before more severe symptoms develop.
4. Size and Swelling Patterns - Inflammation's Visible Manifestation

Tongue size variations and swelling patterns serve as important indicators of inflammation, allergic reactions, and various systemic conditions affecting fluid balance and tissue health. A normal tongue fits comfortably within the mouth without pressing against teeth or causing discomfort, but significant size changes often signal underlying health issues requiring attention. Macroglossia, or enlarged tongue, can indicate hypothyroidism, acromegaly, amyloidosis, or severe allergic reactions, while also potentially suggesting sleep apnea or breathing difficulties that impact overall health. Localized swelling on one side may indicate infection, trauma, or rarely, tumors requiring immediate medical evaluation. Generalized tongue swelling often accompanies allergic reactions, angioedema, or autoimmune conditions like Sjögren's syndrome or lupus. Conversely, a shrunken or atrophied tongue may indicate severe malnutrition, advanced age-related changes, or neurological conditions affecting muscle mass. Swelling patterns provide clues about underlying causes—rapid onset suggests allergic reactions or infections, while gradual changes may indicate chronic conditions like thyroid disorders or autoimmune diseases. The relationship between tongue size and breathing quality affects sleep patterns, cardiovascular health, and cognitive function, making size assessment crucial for overall health evaluation. Indentations along tongue edges, called scalloped tongue, often indicate chronic swelling, teeth grinding, or anxiety-related tongue pressing, reflecting stress levels and sleep quality that impact multiple body systems.
5. Movement and Mobility Assessment - Neurological Function Indicators
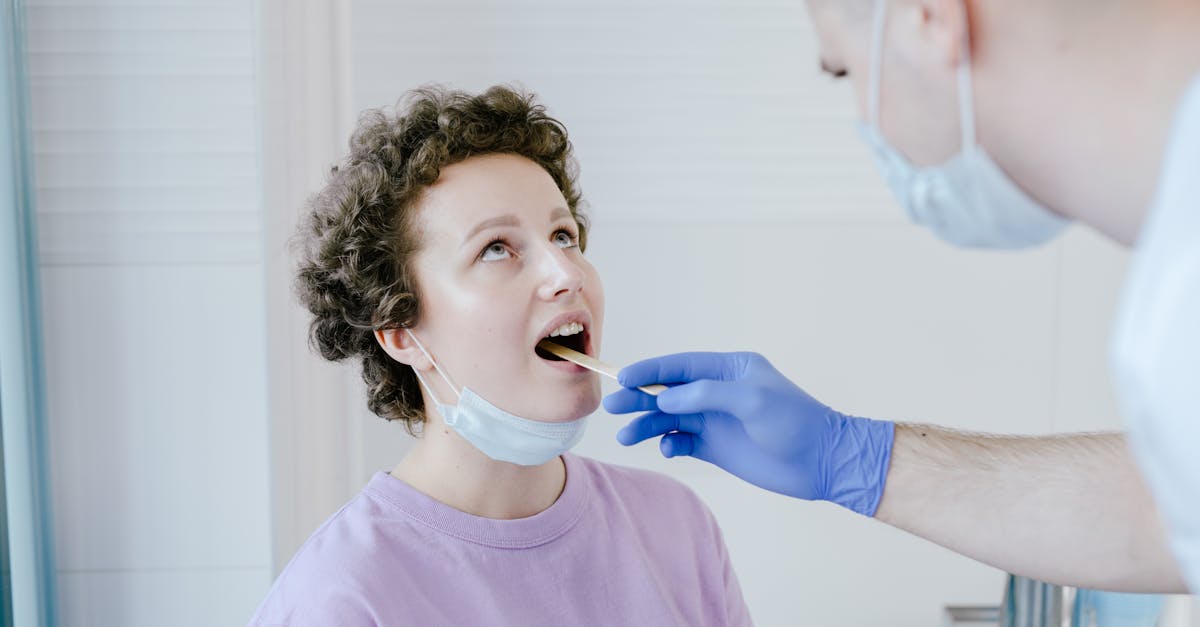
Tongue movement patterns and mobility provide critical insights into neurological function, muscle strength, and coordination that affect speech, swallowing, and overall quality of life. Normal tongue movement should be smooth, coordinated, and symmetrical, with the ability to protrude straight forward, move side to side, and curl upward without tremor or deviation. Neurological conditions often manifest through altered tongue movement patterns before other symptoms become apparent, making movement assessment valuable for early detection. Tongue deviation to one side during protrusion may indicate stroke, Bell's palsy, or other cranial nerve dysfunction, while tremors can suggest Parkinson's disease, essential tremor, or medication side effects. Fasciculations, or small muscle twitches visible on the tongue surface, may indicate motor neuron diseases like ALS or nutritional deficiencies affecting nerve function. Reduced mobility or stiffness can result from oral cancer, infections, autoimmune conditions, or medication effects, while hyperactive movement might suggest anxiety disorders, hyperthyroidism, or stimulant use. The coordination between tongue movement and swallowing function affects nutrition absorption and aspiration risk, making assessment crucial for preventing complications. Speech clarity often correlates with tongue mobility, and changes in articulation can indicate progressive neurological conditions. Regular self-assessment of tongue movement helps identify neurological changes early, enabling prompt medical intervention that can significantly impact treatment outcomes and quality of life preservation.
6. Taste Bud Changes and Sensory Function - The Gateway to Nutritional Awareness

Taste bud function and sensory changes on the tongue surface provide valuable information about nutritional status, medication effects, and various health conditions that impact quality of life and eating behaviors. Healthy taste buds appear as small, pink bumps distributed across the tongue surface, enabling detection of sweet, sour, salty, bitter, and umami flavors that guide food choices and nutritional intake. Diminished taste sensation, called hypogeusia, or complete taste loss, called ageusia, can result from zinc deficiency, vitamin B12 deficiency, diabetes, kidney disease, liver dysfunction, or certain medications, potentially leading to poor nutrition and reduced food enjoyment. Altered taste perception, known as dysgeusia, where foods taste metallic, bitter, or unpleasant, often indicates medication side effects, chemotherapy treatment, pregnancy hormonal changes, or oral infections that require medical attention. Enlarged or inflamed taste buds may suggest allergic reactions, infections, acid reflux, or nutritional deficiencies, while absent taste buds in certain areas can indicate nerve damage or autoimmune conditions. The relationship between taste function and appetite regulation affects weight management, blood sugar control, and overall nutritional status, making taste assessment important for metabolic health monitoring. Burning tongue syndrome, characterized by persistent burning sensations despite normal appearance, often correlates with hormonal changes, anxiety, diabetes, or nutritional deficiencies. Regular attention to taste changes helps identify underlying health issues and enables dietary adjustments that support optimal nutrition and health maintenance throughout life.
7. Breath Odor Correlation - Internal Health Reflected Through Scent
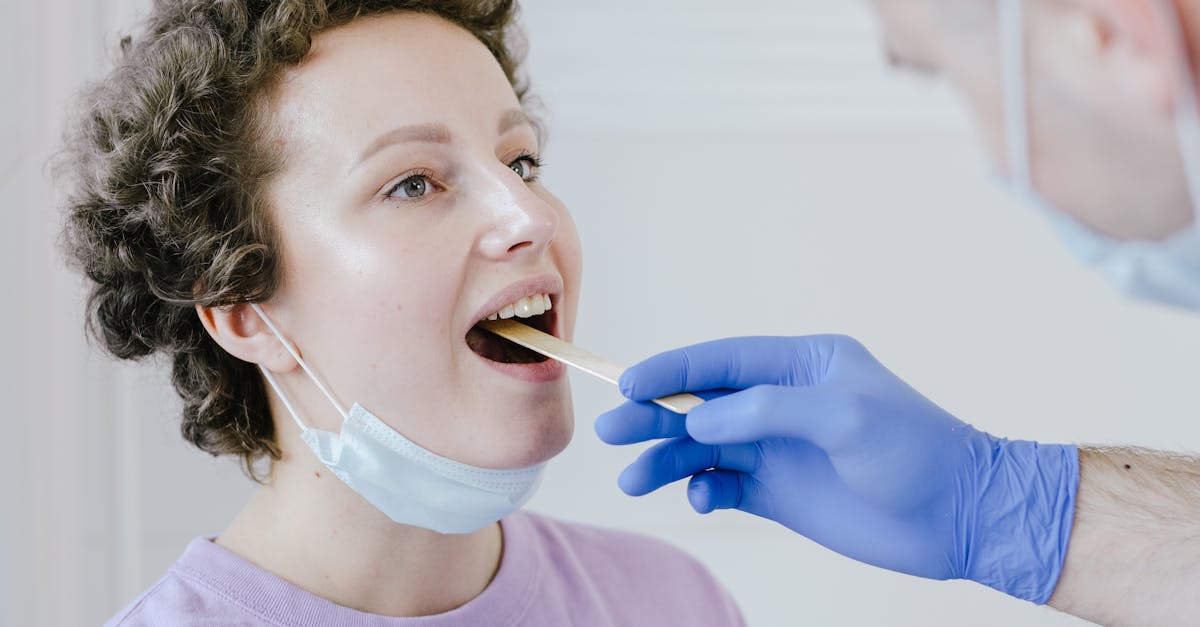
The relationship between tongue characteristics and breath odor provides significant insights into digestive health, oral hygiene, metabolic function, and various systemic conditions that affect overall well-being. While occasional bad breath is normal, persistent halitosis often indicates underlying health issues that manifest through tongue changes and require medical attention. Bacterial overgrowth on the tongue surface, visible as thick coating or discoloration, produces sulfur compounds that create characteristic odors while potentially indicating digestive imbalances, poor oral hygiene, or immune system dysfunction. Sweet or fruity breath odors combined with tongue changes may suggest diabetes or ketosis, while ammonia-like odors can indicate kidney dysfunction or liver disease. Metallic breath often correlates with medication effects, dental problems, or certain nutritional deficiencies that also affect tongue appearance and function. The posterior tongue area, where bacteria commonly accumulate, significantly contributes to breath odor and reflects overall oral health status that impacts cardiovascular health and systemic inflammation levels. Dry mouth conditions, often visible through tongue texture changes, promote bacterial growth and worsen breath odor while potentially indicating medication side effects, autoimmune conditions, or dehydration. Geographic tongue patterns sometimes correlate with specific breath odor characteristics, suggesting underlying digestive or immune system imbalances. Regular tongue cleaning and monitoring breath changes help identify health issues early, while persistent problems warrant medical evaluation to address underlying causes rather than simply masking symptoms with temporary solutions.
8. Hydration Status Indicators - The Body's Water Balance Gauge
Tongue appearance serves as an excellent indicator of hydration status and fluid balance, providing immediate visual feedback about the body's water levels and electrolyte balance that affects all organ systems. A well-hydrated tongue maintains a moist, pink appearance with adequate saliva production, while dehydration manifests through various visible changes that correlate with overall health status. Dry, sticky, or rough tongue texture often indicates dehydration, which can result from inadequate fluid intake, excessive fluid loss, certain medications, or underlying conditions like diabetes or kidney disease. The tongue's ability to produce adequate saliva affects digestion, oral health, and the body's natural cleansing mechanisms, making hydration assessment crucial for overall health monitoring. Severe dehydration may cause the tongue to appear shrunken, deeply furrowed, or unusually dark, while overhydration can sometimes manifest as excessive saliva production or tongue swelling. The relationship between hydration status and tongue coating thickness provides insights into the body's detoxification processes and metabolic function. Electrolyte imbalances, often accompanying dehydration, can affect tongue muscle function and sensation, impacting speech and swallowing abilities. Chronic dehydration reflected through persistent tongue changes increases risk for kidney stones, urinary tract infections, constipation, and cardiovascular complications. Environmental factors, age-related changes, and medication effects influence hydration requirements and tongue appearance, making regular assessment valuable for maintaining optimal health. Proper hydration supports immune function, cognitive performance, and physical endurance, with tongue monitoring serving as an accessible method for ensuring adequate fluid balance throughout daily activities.
9. Geographic Tongue Patterns - Mapping Immune System Activity
Geographic tongue, characterized by irregular patches of missing papillae creating map-like patterns on the tongue surface, provides valuable insights into immune system function and inflammatory processes affecting overall health. This benign condition affects approximately 1-3% of the population and often correlates with other health conditions, making pattern recognition important for comprehensive health assessment. The patches typically appear as red areas with white or yellow borders that change location and size over time, reflecting dynamic immune system activity and inflammatory responses throughout the body. Research suggests geographic tongue patterns often correlate with psoriasis, eczema, allergies, and autoimmune conditions, indicating shared inflammatory pathways that affect multiple organ systems. Stress levels, hormonal changes, and nutritional deficiencies can influence geographic tongue severity and pattern distribution, providing insights into overall health status and lifestyle factors affecting well-being. The condition often worsens during periods of illness, stress, or hormonal fluctuation, serving as a visible indicator of immune system challenges that may require attention. While geographic tongue itself is harmless, its presence may indicate increased susceptibility to other inflammatory conditions, making monitoring valuable for preventive health care. Dietary triggers, including spicy foods, citrus fruits, or food additives, can exacerbate geographic tongue patterns, potentially revealing food sensitivities or allergic reactions that affect digestive health. The relationship between geographic tongue and vitamin deficiencies, particularly B vitamins and zinc, suggests nutritional factors that influence immune function and inflammatory responses throughout the body.
10. Age-Related Changes - The Timeline of Tongue Health Evolution
Age-related changes in tongue characteristics provide important insights into the natural aging process and help distinguish normal variations from pathological conditions requiring medical attention. As individuals age, the tongue undergoes various structural and functional changes that reflect overall health status and aging-related physiological modifications affecting multiple body systems. Taste bud numbers naturally decrease with age, potentially reducing taste sensitivity and affecting appetite, nutrition, and eating enjoyment, while also making it important to monitor for excessive changes that might indicate underlying health issues. Tongue muscle mass and strength may diminish over time, affecting speech clarity, swallowing function, and oral motor control, with significant changes potentially indicating neurological conditions or nutritional deficiencies requiring intervention. Saliva production often decreases with age, leading to dry mouth conditions that affect tongue appearance, oral health, and digestion, while also increasing infection risk and medication absorption issues. The tongue's healing capacity may slow with age, making minor injuries or irritations more persistent and potentially problematic, while also affecting the body's ability to recover from oral infections or inflammatory conditions. Medication effects become more pronounced with age, as multiple prescriptions can cause tongue changes, dry mouth, or altered taste sensation that impacts nutrition and quality of life. Age-related immune system changes may manifest through increased susceptibility to oral infections, slower healing, or altered inflammatory responses visible on the tongue surface. Regular monitoring of age-related tongue changes helps distinguish normal aging from pathological processes, enabling appropriate medical intervention when necessary and supporting healthy aging through proper oral care and nutrition management.
11. When to Seek Medical Attention - Red Flags and Professional Evaluation
Recognizing when tongue changes warrant professional medical evaluation is crucial for early detection and treatment of potentially serious health conditions that may initially manifest through oral symptoms. While many tongue variations are benign and temporary, certain characteristics indicate the need for prompt medical attention to prevent complications and ensure appropriate treatment. Persistent white or red patches that don't resolve within two weeks may indicate precancerous conditions, oral cancer, or autoimmune disorders requiring immediate professional evaluation and possible biopsy. Sudden tongue swelling, especially when accompanied by difficulty breathing or swallowing, suggests allergic reactions or angioedema requiring emergency medical care to prevent life-threatening complications. Persistent pain, numbness, or burning sensations that interfere with eating, speaking, or daily activities may indicate nerve damage, infections, or underlying systemic conditions requiring specialized treatment. Significant changes in tongue color, such as blue, black, or bright red discoloration, particularly when accompanied by other symptoms like fever, fatigue, or breathing difficulties, warrant immediate medical assessment. Progressive difficulty with tongue movement, speech changes, or swallowing problems may indicate neurological conditions requiring early intervention for optimal outcomes. Recurring ulcers, persistent bad breath despite good oral hygiene, or tongue changes accompanied by unexplained weight loss, fatigue, or other systemic symptoms require comprehensive medical evaluation. The key principle involves seeking professional assessment for any tongue changes that persist beyond two weeks, worsen over time, or interfere with normal function, as early detection and treatment significantly improve outcomes for most conditions affecting tongue health and overall well-being.