12 Skin Conditions Diagnosed Primarily Through Visual Assessment
# 12 Skin Conditions Diagnosed Primarily Through Visual Assessment: A Comprehensive Guide to Dermatological Recognition
The human skin serves as our body's largest organ and most visible health indicator, making visual assessment the cornerstone of dermatological diagnosis. Throughout medical history, skilled clinicians have relied primarily on their trained eyes to identify and categorize skin conditions, developing sophisticated pattern recognition skills that remain unmatched by modern technology. Visual diagnosis in dermatology combines scientific knowledge with clinical artistry, requiring practitioners to observe subtle variations in color, texture, distribution patterns, and morphological characteristics that distinguish one condition from another. This diagnostic approach has proven remarkably effective, with experienced dermatologists achieving diagnostic accuracy rates exceeding 85% through visual examination alone. The following exploration delves into twelve distinct skin conditions that exemplify the power of visual assessment, each presenting unique characteristics that allow for confident identification through careful observation. These conditions span various categories of dermatological pathology, from infectious diseases to autoimmune disorders, demonstrating how visual cues can reveal complex underlying processes affecting skin health and appearance.
1. Psoriasis - The Silvery-Scaled Sentinel
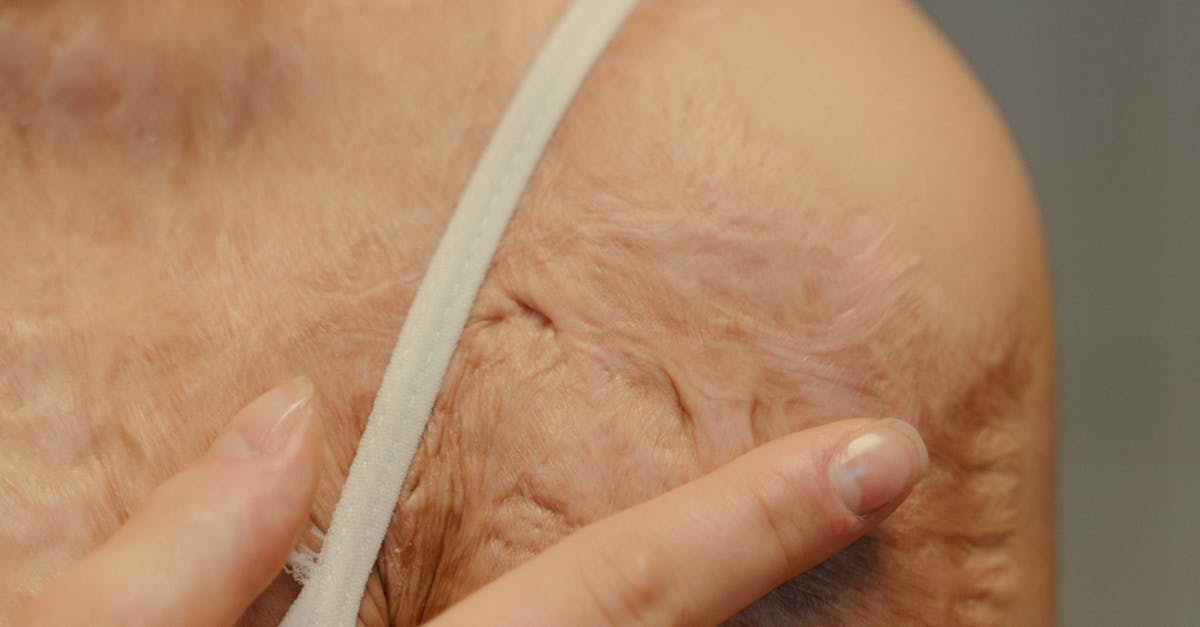
Psoriasis stands as one of the most recognizable skin conditions in dermatology, presenting with characteristic silvery-white scales overlying well-demarcated, erythematous plaques that create an unmistakable visual signature. This chronic autoimmune condition affects approximately 2-3% of the global population and manifests through accelerated skin cell turnover, resulting in the accumulation of thick, scaly patches that typically appear on extensor surfaces such as elbows, knees, and the scalp. The visual diagnosis of psoriasis relies heavily on the distinctive appearance of these lesions, which often exhibit a symmetrical distribution pattern and demonstrate the pathognomonic "Auspitz sign" when scales are gently removed, revealing pinpoint bleeding beneath. The plaques themselves present with sharply defined borders that contrast markedly with surrounding healthy skin, while the characteristic silvery scales can be easily distinguished from other scaling conditions through their adherent nature and underlying salmon-pink coloration. Experienced clinicians can often identify psoriasis variants, including guttate psoriasis with its distinctive droplet-like lesions, or inverse psoriasis affecting flexural areas, purely through visual assessment of lesion morphology and distribution patterns.
2. Vitiligo - The Portrait of Depigmentation
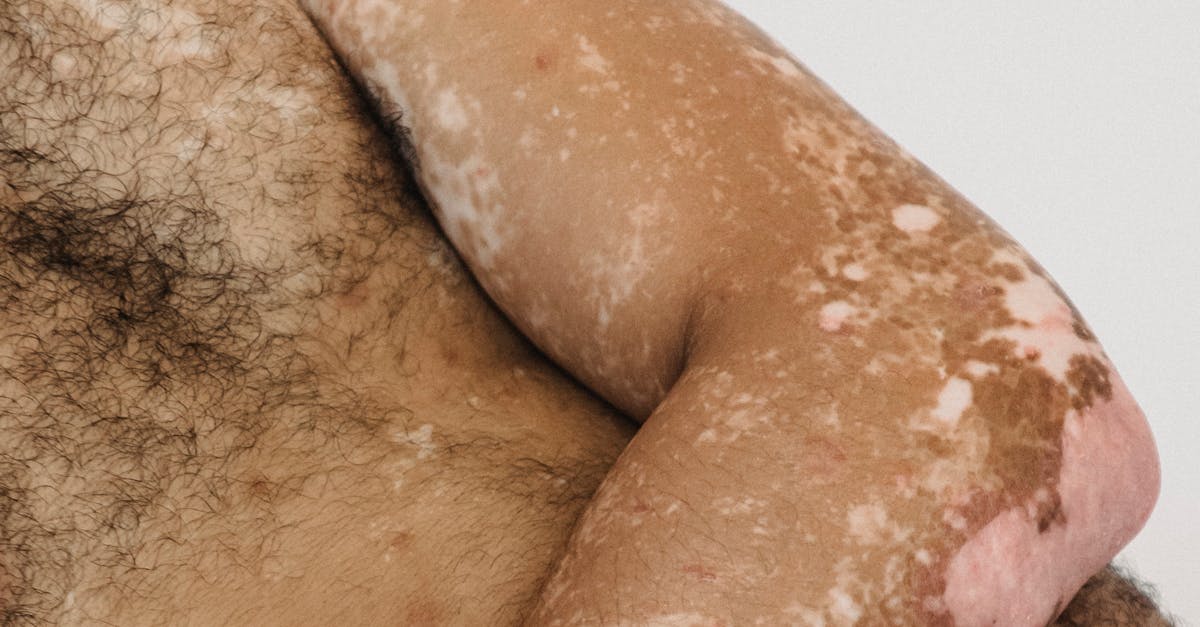
Vitiligo presents as one of dermatology's most visually striking conditions, characterized by well-circumscribed patches of complete depigmentation that create stark contrast against normal skin pigmentation. This acquired disorder affects melanocytes, resulting in the progressive loss of skin color in distinct patterns that can be readily identified through visual examination alone. The condition typically manifests as symmetrical, chalky-white macules and patches with sharply demarcated borders, often beginning around body openings, joints, or areas subject to trauma. Visual assessment reveals several distinctive patterns, including focal vitiligo with isolated patches, segmental vitiligo following dermatomal distributions, and generalized vitiligo with bilateral symmetrical involvement. The diagnosis becomes particularly evident when examining areas of recent depigmentation, where the contrast between affected and unaffected skin creates clear boundaries that distinguish vitiligo from other hypopigmentary disorders. Advanced cases may show characteristic features such as leukotrichia (whitening of hair within affected areas) and the phenomenon of Koebner's response, where new lesions develop at sites of skin trauma. The visual recognition of vitiligo's progressive nature, combined with its distinctive appearance and distribution patterns, makes it one of the most reliably diagnosed skin conditions through observation alone.
3. Melanoma - The Chameleon of Malignancy

Melanoma represents the most dangerous form of skin cancer, yet its visual characteristics provide crucial diagnostic clues that can be life-saving when recognized early through systematic observation. The ABCDE criteria (Asymmetry, Border irregularity, Color variation, Diameter greater than 6mm, and Evolution) form the foundation of visual melanoma assessment, enabling healthcare providers and patients to identify suspicious lesions requiring immediate attention. Visual diagnosis of melanoma relies on recognizing departures from normal mole patterns, including asymmetrical shapes where one half doesn't match the other, irregular or notched borders that deviate from smooth circular patterns, and color variations within a single lesion ranging from brown and black to red, white, or blue hues. The visual assessment becomes particularly critical when observing changes over time, as melanomas characteristically evolve in size, shape, color, or texture, distinguishing them from stable benign nevi. Advanced melanomas may present with additional visual features such as ulceration, bleeding, or nodular components that create three-dimensional irregularities visible to the naked eye. The ability to recognize these visual warning signs through careful skin examination has proven instrumental in early melanoma detection, significantly improving patient outcomes and survival rates when suspicious lesions are identified and biopsied promptly.
4. Eczema (Atopic Dermatitis) - The Inflammatory Mosaic
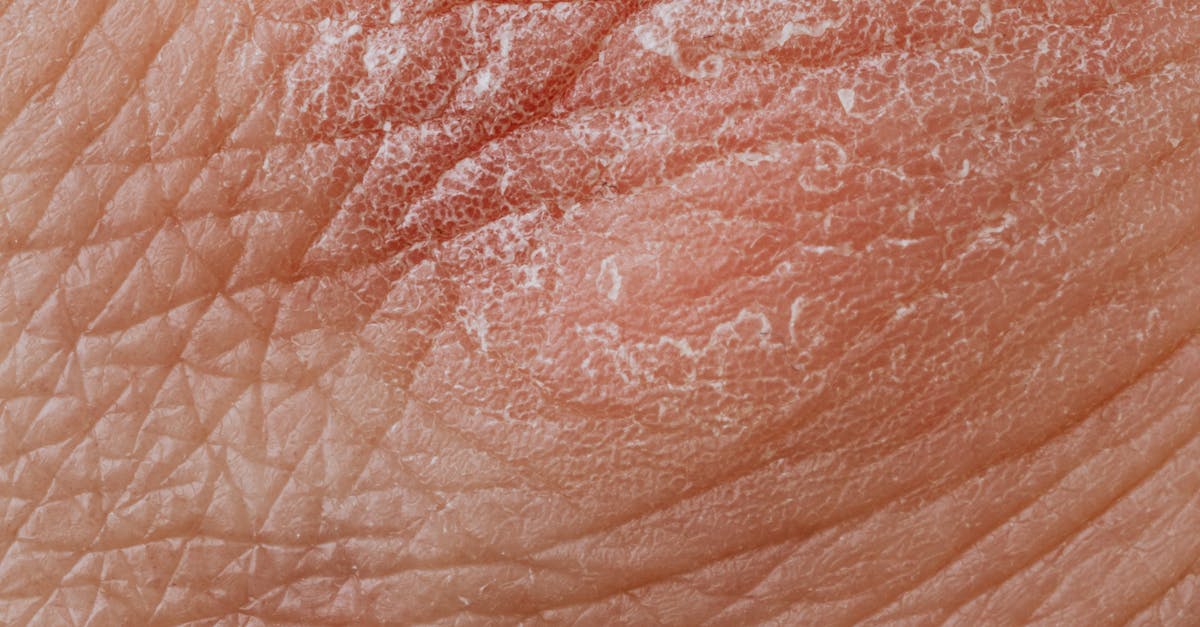
Eczema, particularly atopic dermatitis, presents a complex visual landscape characterized by inflammatory changes that vary significantly based on patient age, disease severity, and chronicity of involvement. The visual diagnosis of eczema relies on recognizing patterns of erythematous, scaling, and often lichenified patches that demonstrate characteristic distribution patterns specific to different age groups. In infants and young children, eczema typically manifests on the face, scalp, and extensor surfaces with acute inflammatory features including erythema, vesiculation, and weeping, creating a distinctive visual presentation that experienced clinicians can readily identify. Adult presentations often show chronic changes with lichenification, hyperpigmentation, and excoriation marks concentrated in flexural areas such as the antecubital and popliteal fossae. The visual assessment of eczema encompasses not only the primary lesions but also secondary changes resulting from scratching and chronic inflammation, including linear excoriations, post-inflammatory hyperpigmentation, and areas of secondary bacterial infection. The condition's visual characteristics also include the presence of xerosis (dry skin) in surrounding areas and the absence of well-demarcated borders that distinguish it from other inflammatory skin conditions. Seasonal variations and flare patterns visible through photographic documentation can further support the visual diagnosis of atopic dermatitis.
5. Rosacea - The Persistent Facial Flush

Rosacea manifests as a chronic inflammatory condition affecting the central face, presenting with distinctive visual features that enable confident diagnosis through careful observation of facial erythema patterns and associated inflammatory changes. The condition typically begins with persistent erythema across the central face, including the nose, cheeks, chin, and central forehead, creating a characteristic butterfly-like distribution that distinguishes it from other facial dermatoses. Visual assessment reveals several key diagnostic features, including persistent background erythema that doesn't fade completely, papulopustular lesions that resemble acne but lack comedones, and telangiectasias that create visible vascular networks across affected areas. The progression of rosacea can be visually tracked through its various stages, from early erythematotelangiectatic rosacea with flushing and visible blood vessels to papulopustular rosacea with inflammatory bumps and pustules. Advanced cases may develop phymatous changes, particularly rhinophyma, which creates distinctive nasal enlargement and surface irregularities that are unmistakable upon visual examination. The visual diagnosis is further supported by observing trigger-related flares, the absence of comedones despite acne-like appearance, and the characteristic sparing of the periorbital area that helps differentiate rosacea from other inflammatory facial conditions.
6. Seborrheic Dermatitis - The Greasy Scale Phenomenon
Seborrheic dermatitis presents with highly characteristic visual features that make it one of the most readily recognizable inflammatory skin conditions, particularly when affecting the scalp, face, and other sebum-rich areas of the body. The condition manifests as erythematous patches covered with greasy, yellowish scales that adhere to the skin surface, creating a distinctive appearance that experienced clinicians can identify at a glance. Visual assessment reveals the predilection for areas rich in sebaceous glands, including the scalp, eyebrows, nasolabial folds, external ear canals, and presternal area, with lesions demonstrating characteristic salmon-colored erythema beneath the overlying scales. The scaling pattern in seborrheic dermatitis differs markedly from other scaling conditions, appearing more adherent and oily rather than dry and powdery, while the underlying erythema shows a distinctive pink-orange hue that contrasts with the deeper red coloration seen in psoriasis or eczema. In scalp involvement, visual examination reveals diffuse or patchy scaling that may range from mild dandruff to thick, adherent crusts, often accompanied by varying degrees of hair loss in severe cases. The visual diagnosis becomes particularly evident when observing the bilateral symmetrical distribution pattern and the characteristic involvement of skin folds and hair-bearing areas that distinguish seborrheic dermatitis from other inflammatory dermatoses.
7. Acne Vulgaris - The Comedonal Landscape
Acne vulgaris represents one of the most common skin conditions worldwide, presenting with a distinctive visual spectrum of lesions that allows for straightforward diagnosis and severity assessment through careful observation of comedonal and inflammatory changes. The visual hallmarks of acne include the presence of comedones (blackheads and whiteheads), which serve as pathognomonic features distinguishing acne from other papulopustular conditions affecting the face, chest, and back. Visual assessment encompasses the full range of acne lesions, from non-inflammatory comedones that appear as small, flesh-colored or dark papules, to inflammatory papules, pustules, and nodules that create varying degrees of erythema and swelling. The distribution pattern of acne lesions provides crucial visual diagnostic information, typically affecting areas with high sebaceous gland density including the face, upper chest, and back, while sparing areas like the periorbital region where sebaceous glands are sparse. Chronic acne cases present additional visual features including post-inflammatory hyperpigmentation, atrophic or hypertrophic scarring, and persistent erythema that help clinicians assess disease severity and duration. The visual evolution of individual lesions, from initial comedone formation through inflammatory progression to resolution or scarring, provides valuable information about disease activity and treatment response that can be monitored through systematic visual documentation.
8. Herpes Simplex - The Vesicular Signature
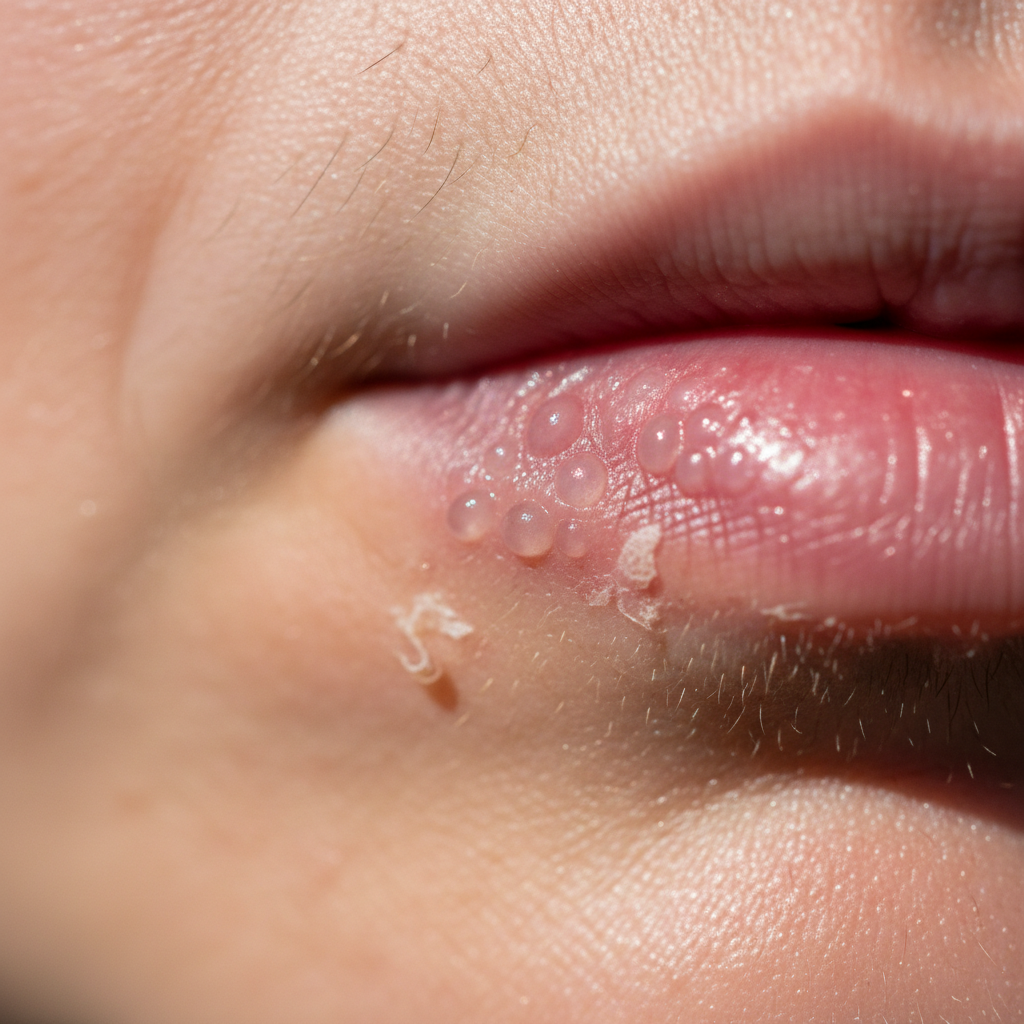
Herpes simplex virus infections create one of the most recognizable vesicular eruptions in dermatology, with characteristic visual features that enable rapid diagnosis through observation of lesion morphology, distribution, and evolutionary patterns. The classic presentation begins with prodromal symptoms followed by the appearance of grouped vesicles on an erythematous base, creating the pathognomonic "dewdrop on a rose petal" appearance that experienced clinicians can identify immediately. Visual assessment reveals the characteristic clustering of small, clear vesicles that typically measure 2-4mm in diameter and demonstrate a predilection for mucocutaneous junctions, particularly around the lips (herpes labialis) or genital areas. The evolutionary pattern of herpes lesions provides crucial diagnostic information, progressing from initial vesiculation through pustulation, ulceration, and crusting phases over a predictable 7-10 day course that can be visually documented and tracked. Recurrent episodes often demonstrate consistent anatomical locations and reduced severity compared to primary infections, with visual features including smaller lesion clusters, shorter duration, and less pronounced inflammatory response. The visual diagnosis becomes particularly evident when observing the unilateral distribution pattern that respects anatomical boundaries and the characteristic absence of systemic signs that distinguish herpes simplex from other vesicular conditions such as herpes zoster or hand-foot-mouth disease.
9. Tinea Infections - The Expanding Ring
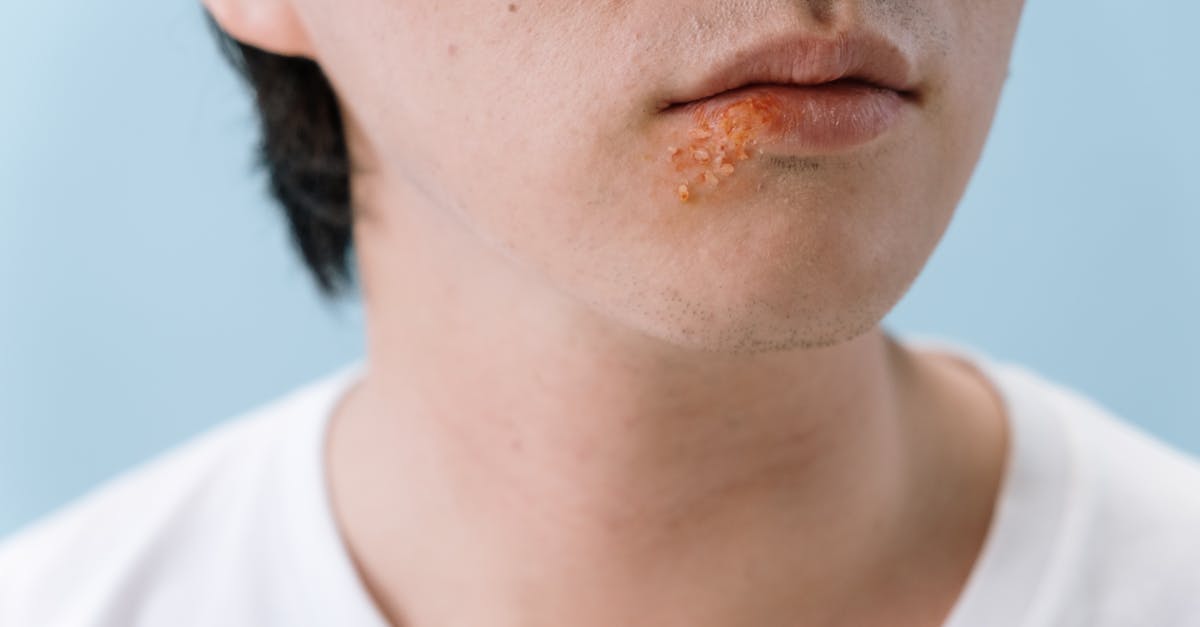
Dermatophyte infections, commonly known as tinea, present with highly characteristic visual features that make them among the most recognizable fungal skin conditions, particularly when manifesting as the classic "ringworm" pattern with expanding annular lesions and central clearing. Visual diagnosis relies on identifying the distinctive morphology of tinea lesions, which typically begin as small, scaly papules that gradually expand outward while developing central clearing, creating the pathognomonic ring-like appearance that gives the condition its common name. The visual assessment encompasses various forms of tinea based on anatomical location, including tinea corporis with its classic annular lesions on the body, tinea pedis presenting with scaling and maceration between the toes, and tinea capitis showing areas of hair loss with associated scaling on the scalp. The advancing border of tinea lesions demonstrates characteristic features including mild erythema, fine scaling, and occasional vesiculation that distinguish it from other annular conditions such as erythema migrans or granuloma annulare. Visual examination often reveals additional diagnostic clues such as the presence of broken hair shafts in tinea capitis, the characteristic "moccasin" distribution of chronic tinea pedis, or the asymmetrical involvement pattern that differs from the bilateral symmetry typical of inflammatory dermatoses. The ability to recognize these visual patterns enables clinicians to initiate appropriate antifungal therapy while confirming the diagnosis through additional testing methods.
10. Contact Dermatitis - The Geographic Reaction
Contact dermatitis presents with distinctive visual patterns that often provide direct clues to the causative agent through the geometric or linear configurations that mirror the shape and distribution of the offending substance. The visual diagnosis relies heavily on recognizing these characteristic patterns, which may include linear streaks from plant allergens like poison ivy, rectangular patches from adhesive bandages, or circular lesions from metal jewelry containing nickel. Acute contact dermatitis manifests with intense erythema, edema, and vesiculation that creates a distinctive inflammatory appearance, while chronic cases develop lichenification, scaling, and hyperpigmentation that reflect prolonged exposure and repeated scratching. The visual assessment becomes particularly diagnostic when the distribution pattern defies anatomical boundaries and instead follows the outline of external contactants, such as the sharp demarcation lines seen with cosmetic reactions or the characteristic hand and wrist involvement pattern associated with latex glove allergies. Visual examination often reveals additional clues including the sparing of naturally protected areas like skin folds or areas covered by clothing, and the presence of satellite lesions where the allergen may have been transferred by touching. The temporal relationship between exposure and eruption, combined with the characteristic visual patterns and distribution, enables clinicians to identify contact dermatitis and often pinpoint the specific causative agent through careful observation of the reaction pattern.
11. Urticaria (Hives) - The Transient Wheals
Urticaria presents with one of the most distinctive and recognizable visual patterns in dermatology, characterized by raised, erythematous wheals with pale centers that appear and disappear spontaneously, creating a dynamic skin condition that can be readily identified through its characteristic morphology and behavior. The visual hallmarks of urticaria include well-demarcated, raised lesions that blanch with pressure and demonstrate the pathognomonic feature of complete resolution within 24 hours, leaving no residual marks or pigmentation changes. Visual assessment reveals wheals of varying sizes, from small papular lesions to large, geographic plaques that may coalesce to form irregular patterns across the skin surface, often accompanied by intense erythema and associated angioedema in dependent areas. The transient nature of individual lesions provides crucial diagnostic information, as the ability to document lesions that appear and resolve completely within hours distinguishes urticaria from other urticarial-appearing conditions such as urticarial vasculitis or mastocytosis. Chronic urticaria cases may demonstrate additional visual features including dermatographism, where linear wheals develop following mechanical stimulation, or pressure urticaria with delayed swelling at sites of sustained pressure. The visual diagnosis becomes particularly evident when observing the random distribution pattern that doesn't follow anatomical or dermatomal boundaries, combined with the characteristic pale, raised appearance and the absence of scaling or other surface changes that might suggest alternative diagnoses.
12. Basal Cell Carcinoma - The Pearly Nodule

Basal cell carcinoma represents the most common form of skin cancer, presenting with characteristic visual features that enable early recognition through systematic observation of nodular, ulcerative, or superficial morphological patterns. The classic nodular variant appears as a pearly, translucent papule or nodule with prominent telangiectasias coursing across its surface, creating a distinctive appearance that experienced clinicians can readily identify during routine skin examinations. Visual assessment reveals several key diagnostic features including the characteristic rolled, pearly border that surrounds central ulceration in advanced lesions, the presence of arborizing telangiectasias that create visible vascular patterns, and the slow, progressive growth pattern that distinguishes basal cell carcinoma from benign skin lesions. The superficial variant presents as a thin, erythematous plaque with fine scaling and a slightly raised, thread-like border that may be confused with eczema or psoriasis but demonstrates characteristic persistence and slow expansion over time. Visual diagnosis becomes particularly important when observing high-risk anatomical locations such as the nose, ears, and periorbital areas where basal cell carcinomas commonly develop, often presenting as non-healing wounds or persistent irritated areas that fail to respond to conservative treatment. The morpheaform variant creates a scar-like appearance with ill-defined borders and indurated texture that can be challenging to recognize visually but demonstrates characteristic features including skin tethering and subtle color changes that distinguish it from benign scarring processes.
13. Mastering the Visual Language of Dermatology

The twelve skin conditions explored in this comprehensive examination demonstrate the remarkable power and precision of visual assessment in dermatological diagnosis, showcasing how trained observation can reliably identify diverse pathological processes affecting the skin. Each condition presents unique visual signatures that, when properly recognized and interpreted, provide clinicians with immediate diagnostic insights that guide appropriate treatment decisions and patient management strategies. The mastery of visual diagnosis requires not only knowledge of individual condition characteristics but also the ability to distinguish subtle differences between similar-appearing disorders, recognize atypical presentations, and appreciate the dynamic nature of skin