12 Infectious Diseases Identified by Their Characteristic Rashes
The human skin serves as our body's largest organ and often acts as a diagnostic canvas, revealing telltale signs of underlying infectious diseases through distinctive rash patterns. Throughout medical history, healthcare professionals have relied on the characteristic appearance, distribution, and evolution of cutaneous manifestations to identify and differentiate between various infectious agents. From the classic rose-colored spots of typhoid fever to the pathognomonic koplik spots preceding measles, dermatological presentations provide crucial diagnostic clues that can expedite treatment and prevent complications. This comprehensive exploration examines twelve infectious diseases that present with distinctive rashes, each offering unique visual signatures that aid in rapid identification. Understanding these characteristic patterns is essential not only for healthcare providers but also for public health surveillance, as many of these conditions are highly contagious and require immediate intervention. The ability to recognize these dermatological manifestations can mean the difference between early treatment success and potentially life-threatening complications, making this knowledge invaluable in both clinical practice and community health settings.
1. Measles - The Classic Maculopapular Eruption
Measles, caused by the highly contagious measles virus, presents with one of the most recognizable rash patterns in infectious disease medicine. The characteristic eruption begins as small, red, flat spots that appear first behind the ears and along the hairline before spreading systematically across the face, neck, trunk, and extremities over a period of three to four days. This cephalocaudal progression is pathognomonic for measles and helps distinguish it from other viral exanthems. The individual lesions start as discrete macules but quickly become confluent, creating large areas of erythematous, slightly raised patches that give the skin a blotchy, mottled appearance. Prior to the rash's emergence, patients typically experience the prodromal phase characterized by the classic triad of cough, coryza, and conjunctivitis, along with high fever. Koplik spots, small white or blue-white spots surrounded by red halos on the buccal mucosa, appear one to two days before the skin rash and are virtually diagnostic of measles. The rash typically lasts five to six days before beginning to fade in the same order it appeared, often leaving behind temporary brown discoloration and fine desquamation. Despite widespread vaccination programs, measles outbreaks continue to occur in unvaccinated populations, making recognition of this distinctive rash pattern crucial for prompt isolation and public health response.
2. Chickenpox - The Vesicular Landscape
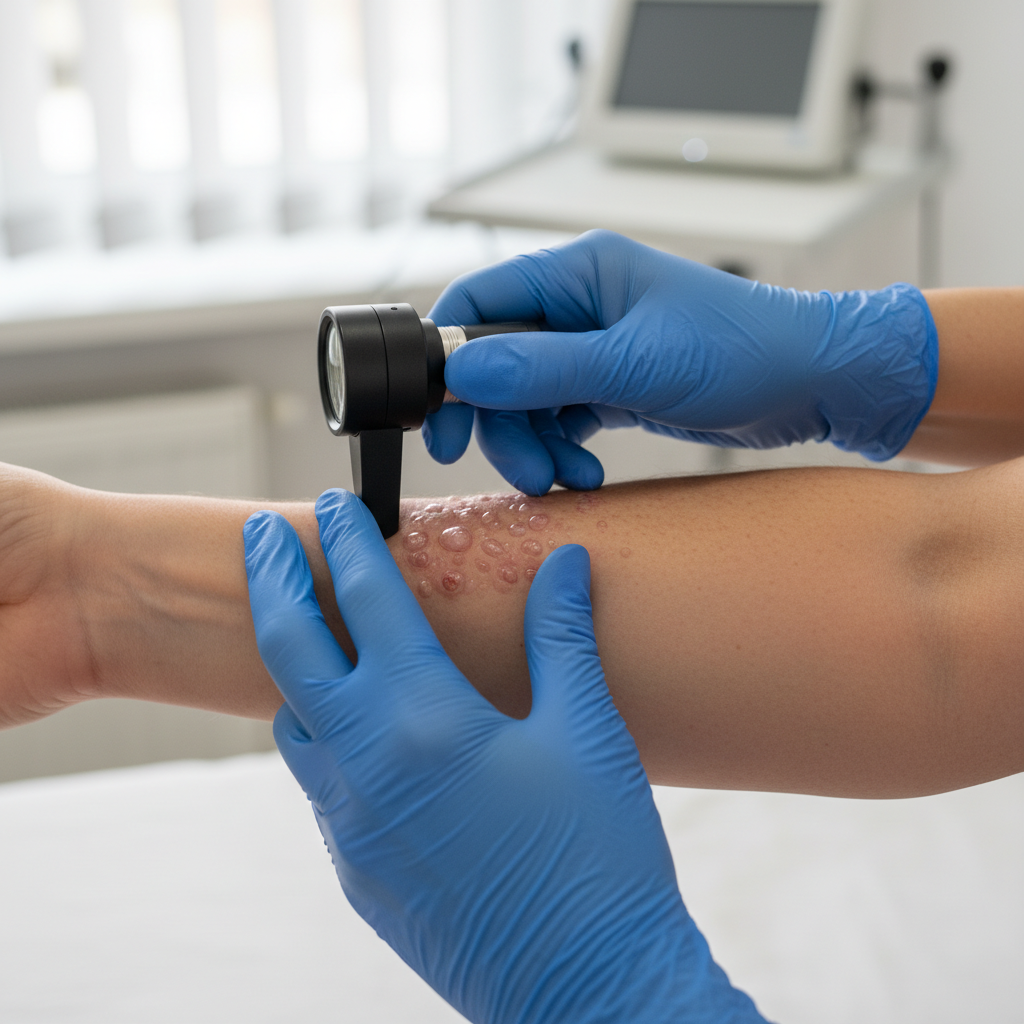
Varicella-zoster virus causes chickenpox, distinguished by its characteristic vesicular rash that appears in successive crops over several days. The eruption typically begins on the trunk and face before spreading to the extremities, presenting initially as small red papules that rapidly evolve into clear, fluid-filled vesicles surrounded by erythematous halos, often described as "dewdrops on rose petals." This distinctive appearance is virtually pathognomonic for chickenpox and helps differentiate it from other vesicular diseases. The lesions progress through predictable stages: macule to papule to vesicle to pustule, and finally to crusted scab, with new crops appearing every 24 to 48 hours. This results in the characteristic finding of lesions in various stages of development simultaneously across the body, a key diagnostic feature that distinguishes chickenpox from smallpox, where lesions are typically in the same stage of development. The vesicles are superficial, thin-walled, and easily ruptured, leading to secondary bacterial infection if scratched. The rash is typically accompanied by mild constitutional symptoms including low-grade fever, malaise, and headache. The vesicles usually begin to crust over within 24 to 48 hours, and patients are considered non-contagious once all lesions have crusted. The entire process from initial eruption to complete healing typically takes 10 to 14 days, though scarring may occur if lesions become secondarily infected or are traumatized.
3. Scarlet Fever - The Sandpaper Texture
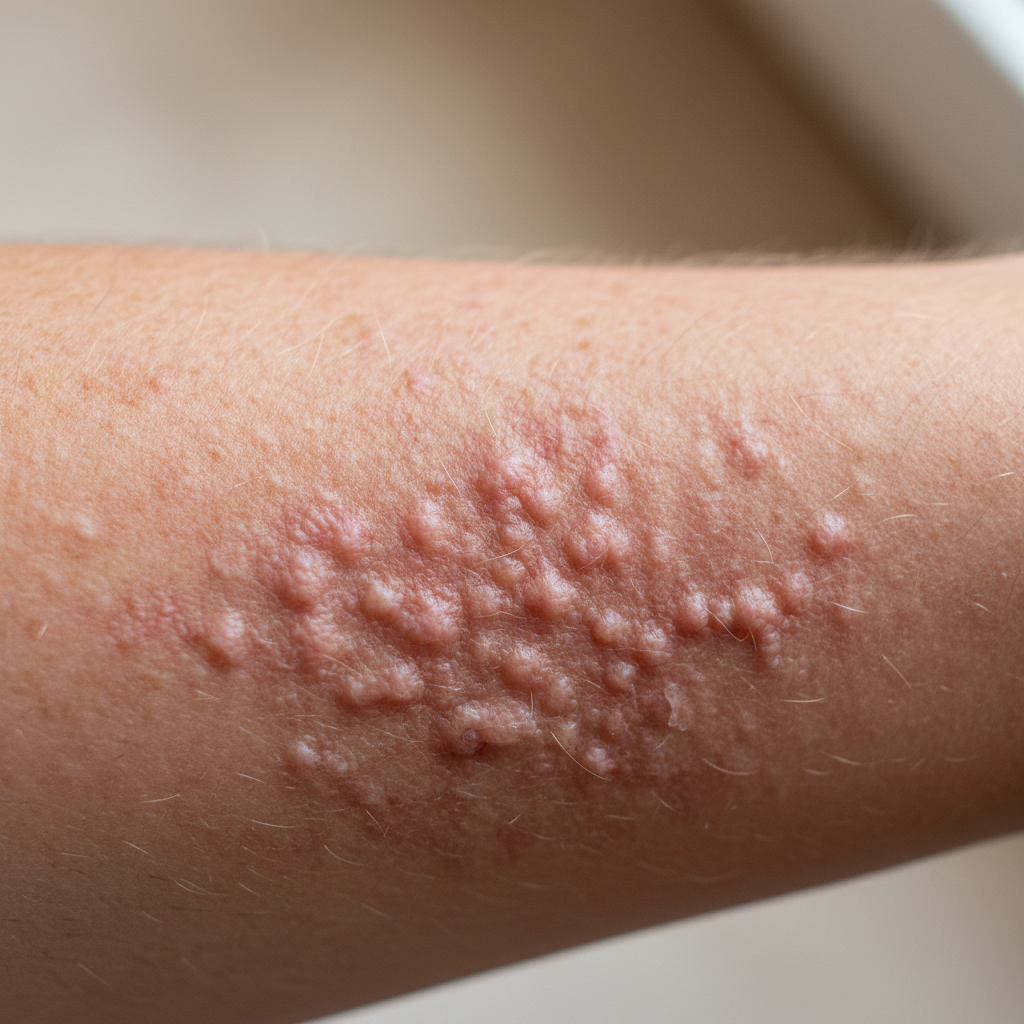
Scarlet fever, caused by group A Streptococcus pyogenes producing erythrogenic toxin, presents with a distinctive rash that feels like fine sandpaper to the touch. The eruption typically appears 12 to 48 hours after the onset of fever and sore throat, beginning on the neck and chest before spreading to the trunk and extremities. The rash consists of numerous small, closely spaced, red papules that give the skin a characteristic rough, sandpaper-like texture that is pathognomonic for this condition. The erythematous background creates a diffuse red appearance, and the rash typically spares the palms and soles while demonstrating characteristic linear petechial streaks called Pastia's lines in skin folds, particularly in the antecubital fossae and axillae. The face shows a characteristic pattern with circumoral pallor, where the area around the mouth remains pale in contrast to the flushed cheeks, creating the classic "slapped cheek" appearance. The tongue initially appears white with red, swollen papillae (white strawberry tongue) before the white coating sloughs off, revealing a bright red tongue with prominent papillae (red strawberry tongue). The rash typically lasts four to five days before beginning to desquamate, starting with fine, branny scaling on the face and progressing to larger sheets of peeling skin on the hands and feet. This desquamation phase can last several weeks and is considered pathognomonic for scarlet fever, helping to confirm the diagnosis retrospectively.
4. Fifth Disease - The Slapped Cheek Phenomenon

Erythema infectiosum, commonly known as fifth disease, is caused by human parvovirus B19 and presents with a distinctive biphasic rash pattern that begins with the characteristic "slapped cheek" appearance. The initial phase manifests as bright red, warm erythema of both cheeks that appears as if the child has been slapped, while the circumoral area remains characteristically pale. This facial erythema is often the first sign that brings patients to medical attention and is virtually pathognomonic for parvovirus B19 infection. One to four days after the facial rash appears, the second phase develops as a lacy, reticular, or net-like erythematous rash on the trunk and extremities. This reticulated pattern results from central clearing of erythematous patches, creating the characteristic lace-like appearance that can wax and wane over several weeks. The rash may become more prominent with exposure to heat, sunlight, exercise, or emotional stress, leading to recurrent episodes that can be concerning to parents but are entirely benign. Unlike many other viral exanthems, fifth disease is typically not associated with significant constitutional symptoms, though adults may experience arthralgia and arthritis, particularly affecting small joints of the hands and feet. The infectious period occurs before the rash appears, during the prodromal phase when patients may have mild cold-like symptoms, making this disease particularly challenging to control in school and daycare settings. The distinctive appearance and relatively benign course make fifth disease one of the more easily recognized childhood exanthems.
5. Roseola - The Post-Fever Eruption
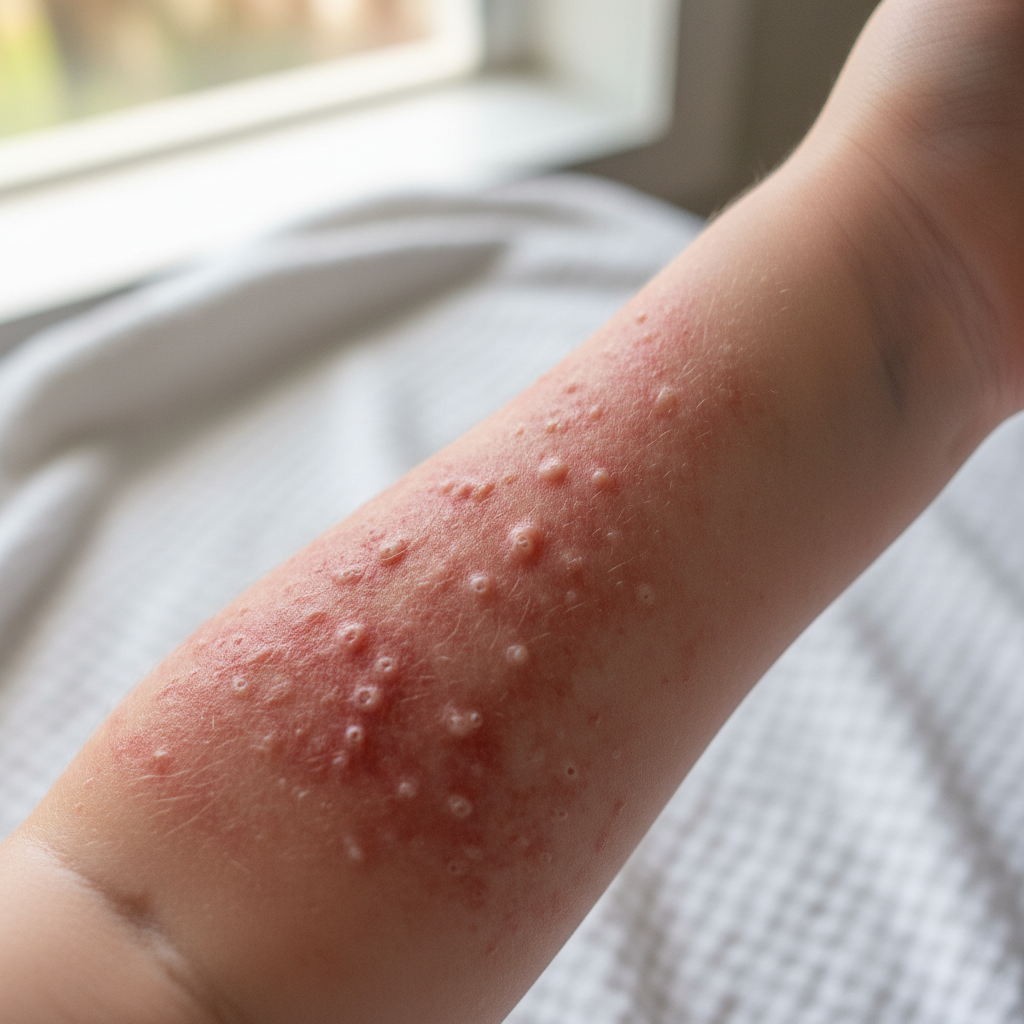
Roseola infantum, caused primarily by human herpesvirus 6 (HHV-6) and occasionally by HHV-7, presents with a unique clinical pattern that distinguishes it from other childhood exanthems. The disease typically affects children between six months and three years of age and follows a characteristic biphasic course. The initial phase is marked by sudden onset of high fever, often reaching 39-40°C (102-104°F), which persists for three to five days without other significant symptoms, creating diagnostic uncertainty for parents and healthcare providers. The fever typically breaks abruptly, often accompanied by improvement in the child's general condition, followed within hours by the appearance of the characteristic rash. The exanthem consists of discrete, rose-colored macules and papules that begin on the trunk and neck before spreading to the face and extremities. The individual lesions are typically 2-5mm in diameter, blanch with pressure, and may become confluent in some areas. Unlike many other viral rashes, the roseola exanthem is generally not pruritic and rarely causes discomfort to the child. The rash typically lasts 24 to 48 hours before fading without desquamation or pigmentary changes. This post-fever timing is pathognomonic for roseola and helps distinguish it from other febrile illnesses with rash. Some children may also develop Nagayama spots, small erythematous papules on the soft palate and uvula, which can be seen during the febrile phase and may aid in early diagnosis.
6. Hand, Foot, and Mouth Disease - The Acral Distribution

Hand, foot, and mouth disease (HFMD), most commonly caused by coxsackievirus A16 and enterovirus 71, presents with a characteristic distribution pattern that gives the disease its descriptive name. The condition typically begins with fever, malaise, and sore throat, followed by the development of painful vesicular lesions in the oral cavity, particularly on the tongue, gums, and buccal mucosa. These oral lesions often ulcerate quickly, causing significant discomfort and difficulty eating or drinking. Simultaneously or shortly after the oral lesions appear, characteristic vesicles develop on the palms, soles, and sometimes the dorsal aspects of the hands and feet. These cutaneous lesions are typically oval-shaped, gray-white vesicles surrounded by erythematous halos and are pathognomonic for HFMD when found in the classic distribution. The vesicles on the hands and feet are usually painless, unlike the oral lesions, and may be accompanied by similar lesions on the buttocks and genital area, particularly in younger children. The acral distribution pattern is unique among common viral exanthems and makes HFMD readily distinguishable from other vesicular diseases. In recent years, atypical presentations have been observed, particularly with certain enterovirus strains, where the rash may extend beyond the classic sites to include the arms, legs, and trunk. The disease is typically self-limited, with lesions resolving within seven to ten days, though some children may experience nail changes, including onychomadesis (nail shedding), several weeks after the acute illness.
7. Impetigo - The Honey-Crusted Lesions
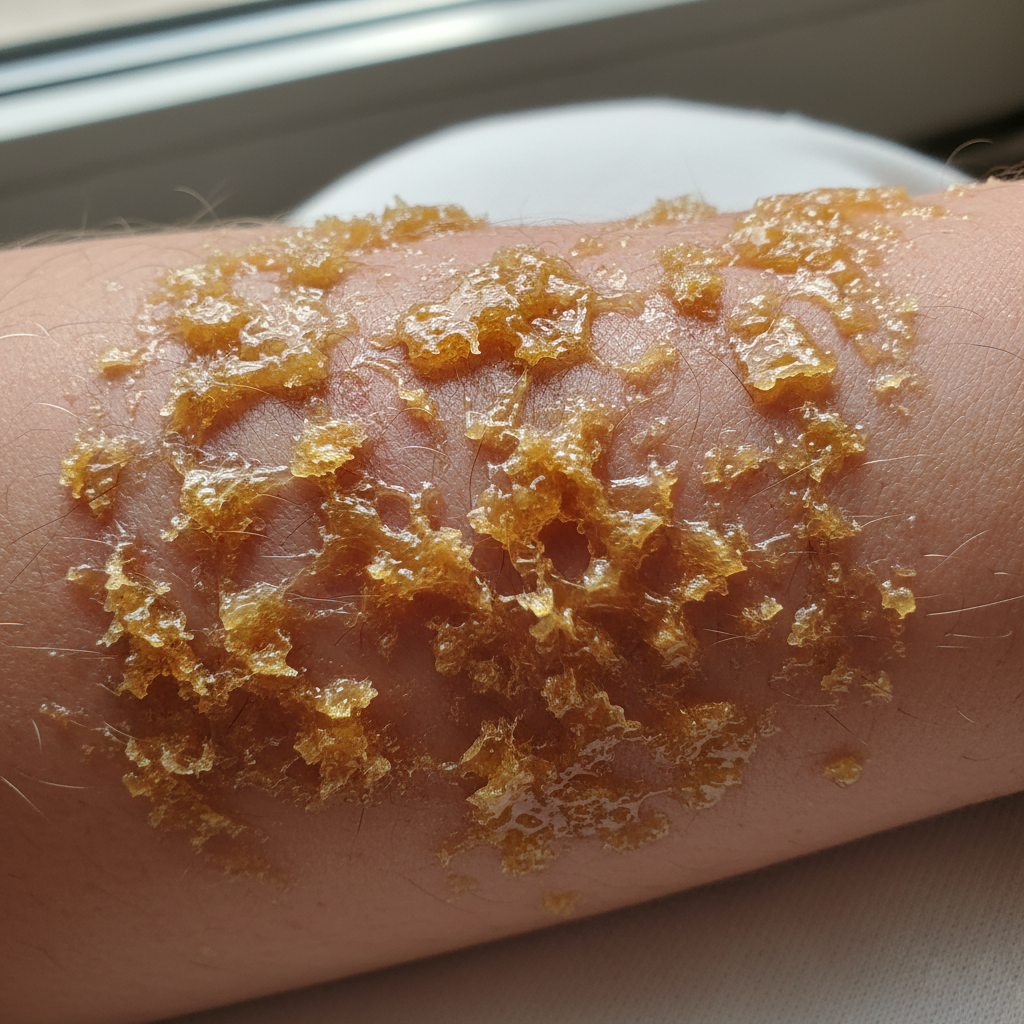
Impetigo, a superficial bacterial skin infection most commonly caused by Staphylococcus aureus and group A Streptococcus, presents with highly characteristic lesions that make it one of the most recognizable bacterial skin infections. The condition manifests in two primary forms: non-bullous (impetigo contagiosa) and bullous impetigo, each with distinctive features. Non-bullous impetigo, which accounts for approximately 70% of cases, begins as small erythematous macules that rapidly progress to vesicles and then to pustules. The hallmark of this condition is the development of thick, adherent, honey-colored or golden-yellow crusts that form when the pustules rupture and dry. These crusts are pathognomonic for impetigo and are often described as having a "stuck-on" appearance that is difficult to remove. The lesions typically occur on exposed areas such as the face, particularly around the nose and mouth, and extremities, though they can appear anywhere on the body. Bullous impetigo, caused primarily by specific strains of S. aureus that produce exfoliative toxins, presents with larger, flaccid bullae that contain clear or slightly turbid fluid. These bullae are fragile and rupture easily, leaving behind shallow erosions with a collarette of scale at the periphery. Both forms of impetigo are highly contagious and can spread rapidly through direct contact or fomites, making early recognition and treatment crucial for preventing outbreaks in schools and daycare centers.
8. Erythema Migrans - The Expanding Target
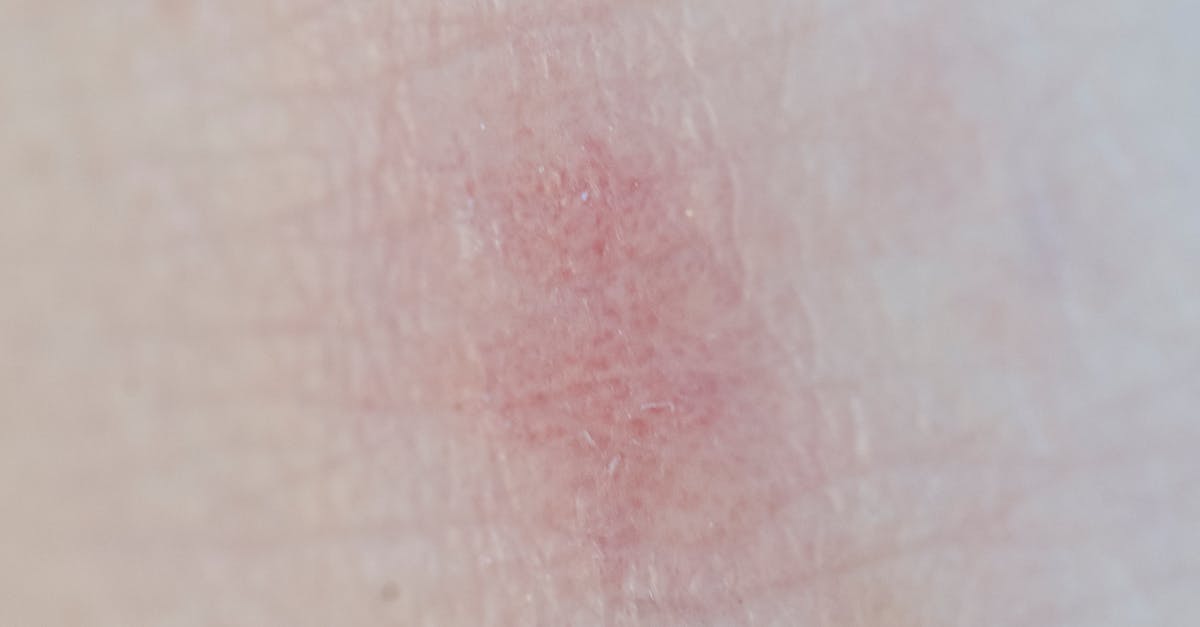
Erythema migrans, the pathognomonic skin lesion of early Lyme disease caused by Borrelia burgdorferi, presents as an expanding erythematous patch with characteristic features that make it one of the most diagnostically significant rashes in infectious disease medicine. The lesion typically appears 3 to 30 days after a tick bite, beginning as a small red area that gradually expands centrifugally at a rate of several centimeters per day. The classic presentation includes central clearing, creating the characteristic "bull's-eye" or target-like appearance, though this central clearing occurs in only about 20% of cases. More commonly, the lesion presents as a uniformly erythematous, expanding patch with well-defined borders and minimal central clearing. The rash is typically asymptomatic or only mildly pruritic, and the affected skin may feel warm to the touch but is rarely painful. The expanding nature of the lesion is pathognomonic for erythema migrans and helps distinguish it from other tick-borne illnesses or local reactions to tick bites. Multiple lesions may occur in cases of disseminated early Lyme disease, representing hematogenous spread of the spirochete. The size of erythema migrans lesions can vary significantly, ranging from a few centimeters to over 30 centimeters in diameter, and the lesions may have irregular shapes as they expand around anatomical structures. Without treatment, erythema migrans typically resolves spontaneously over several weeks to months, but early antibiotic therapy can prevent progression to disseminated Lyme disease and its associated complications.
9. Petechial Rashes - Meningococcemia's Warning Signs
Meningococcal disease, caused by Neisseria meningitidis, can present with a rapidly evolving petechial and purpuric rash that serves as a critical diagnostic clue and prognostic indicator. The cutaneous manifestations of meningococcemia represent one of the most urgent dermatological emergencies in medicine, as the appearance and progression of the rash correlates with disease severity and outcome. The rash typically begins as scattered petechiae, small (1-2mm) red or purple spots that do not blanch with pressure, representing extravasation of blood from damaged capillaries. These initial petechial lesions may be subtle and easily overlooked, particularly in patients with darker skin tones, making careful examination crucial. As the disease progresses, the petechiae may coalesce and evolve into larger purpuric lesions, ecchymoses, and in severe cases, areas of skin necrosis and gangrene. The distribution is typically generalized but may show predilection for pressure points, the trunk, and extremities. The rapid progression from petechiae to purpura and potential skin necrosis within hours reflects the underlying pathophysiology of disseminated intravascular coagulation and vasculitis. The presence of purpuric lesions larger than 2mm in diameter, particularly when associated with fever and signs of systemic illness, should prompt immediate medical evaluation and empirical antibiotic therapy. The "tumbler test," where a glass is pressed against the rash to see if it blanches, is a simple bedside test that can help differentiate petechial rashes from other erythematous eruptions, though any suspicion of meningococcal disease warrants urgent medical attention regardless of the test result.
10. Typhoid Fever - The Rose-Colored Herald
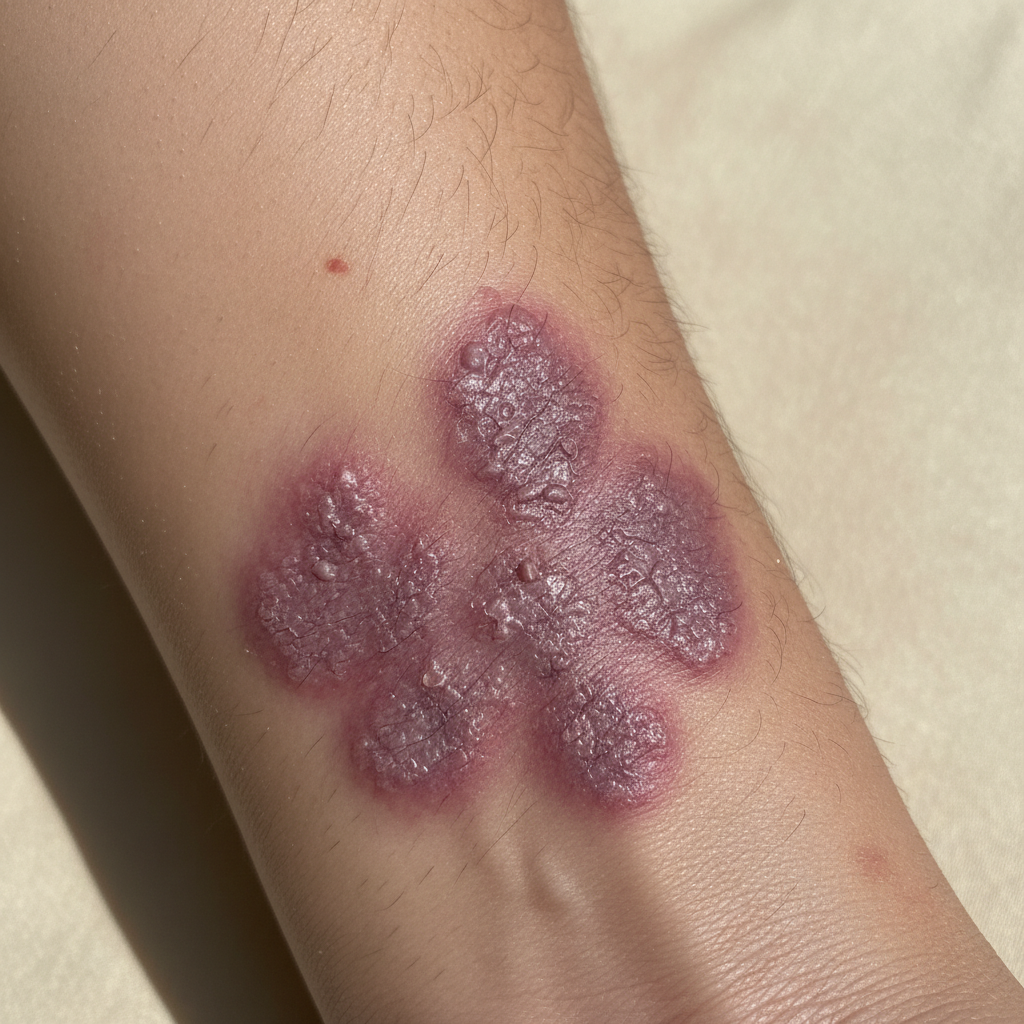
Typhoid fever, caused by Salmonella enterica serovar Typhi, presents with characteristic rose spots that appear during the second week of illness and serve as an important diagnostic clue in this potentially life-threatening systemic infection. The rose spots of typhoid fever are small, rose-colored, blanching macules approximately 2-4mm in diameter that appear in crops on the trunk, particularly the chest and abdomen. These lesions are pathognomonic for typhoid fever when present, though they occur in only 30-50% of patients and may be difficult to detect in individuals with darker skin tones. The spots typically appear in small numbers, usually fewer than 20 lesions, and have a characteristic salmon-pink color that distinguishes them from other bacterial exanthems. Each individual lesion lasts approximately 3-4 days before fading, but new crops may continue to appear for several days, creating a pattern of lesions in various stages of evolution. The rose spots represent bacterial emboli in the skin and can be biopsied to demonstrate the presence of Salmonella organisms, providing definitive microbiological diagnosis. The appearance of rose spots typically coincides with the development of other classic features of typhoid fever, including sustained fever, headache, abdominal pain, and changes in mental status. In the pre-antibiotic era, the recognition of rose spots was crucial for diagnosis, as laboratory confirmation was limited. Today, while blood cultures and serological tests provide more reliable diagnostic methods, the recognition of rose spots remains valuable, particularly in resource-limited settings where laboratory facilities may be unavailable or delayed.
11. Rocky Mountain Spotted Fever - The Centripetal Spread
Rocky Mountain spotted fever (RMSF), caused by Rickettsia rickettsii and transmitted by tick bites, presents with a characteristic rash that demonstrates a distinctive centripetal progression, making it one of the most recognizable tick-borne illness presentations. The rash typically appears 2-5 days after the onset of fever, headache, and myalgia, beginning as small, pink, blanching macules on the wrists and ankles. This peripheral distribution at onset is pathognomonic for RMSF and helps distinguish it from other febrile illnesses with rash. Over the course of hours to days, the rash spreads centripetally toward the trunk, eventually involving the palms and soles in approximately 50-80% of cases. The involvement of palms and soles is particularly significant, as few infectious diseases cause rash in these locations, making