10 Kidney Conditions That Produce Visible Symptoms Over Time
The kidneys, often called the body's silent guardians, work tirelessly behind the scenes to filter waste, regulate blood pressure, and maintain the delicate balance of electrolytes that keep us alive. These bean-shaped organs process approximately 50 gallons of blood daily, yet their deterioration often goes unnoticed until significant damage has occurred. However, when kidney function begins to decline due to various conditions, the body eventually sends visible distress signals that manifest as observable symptoms. Understanding these visual cues is crucial because kidney disease affects over 37 million Americans, with many remaining unaware of their condition until it reaches advanced stages. The following exploration delves into ten specific kidney conditions that produce distinct, visible symptoms over time, ranging from subtle changes in urination patterns to dramatic swelling and skin discoloration. By recognizing these warning signs early, individuals can seek timely medical intervention, potentially slowing disease progression and preserving kidney function. This comprehensive examination will illuminate how each condition uniquely affects the body's appearance and function, providing readers with essential knowledge to protect their renal health and recognize when professional medical evaluation becomes necessary.
1. Chronic Kidney Disease - The Progressive Decline

Chronic Kidney Disease (CKD) represents a gradual loss of kidney function over months or years, affecting millions worldwide and serving as one of the most common causes of kidney-related visible symptoms. As CKD progresses through its five stages, patients begin to exhibit increasingly noticeable physical changes that reflect their kidneys' diminishing ability to filter waste and excess fluid from the blood. The most prominent visible symptom is edema, which typically begins as subtle puffiness around the eyes upon waking and gradually extends to the ankles, feet, and eventually the entire lower extremities. This swelling occurs because damaged kidneys cannot effectively remove excess sodium and water from the body, leading to fluid retention in tissues. Additionally, patients often develop a characteristic pallor due to anemia, as failing kidneys produce insufficient erythropoietin, the hormone responsible for stimulating red blood cell production. The skin may also take on a yellowish or grayish tint due to the accumulation of uremic toxins. Changes in urination patterns become evident, with some patients experiencing foamy urine due to protein leakage, while others notice decreased urine output or changes in urine color. As CKD advances, patients may also exhibit visible signs of bone disease, including skeletal deformities, as the kidneys fail to properly regulate calcium and phosphorus levels.
2. Polycystic Kidney Disease - The Expanding Threat

Polycystic Kidney Disease (PKD) is a genetic disorder characterized by the growth of numerous fluid-filled cysts within the kidneys, creating distinctive visible symptoms as the condition progresses over time. The most striking physical manifestation of PKD is the gradual enlargement of the abdomen as the cyst-filled kidneys expand significantly beyond their normal size, sometimes reaching the dimensions of footballs. Patients often notice their waistline increasing and may require larger clothing sizes, not due to weight gain but because of the physical space occupied by the enlarged kidneys. This abdominal distension can become so pronounced that it affects posture and gait, creating a characteristic appearance in advanced cases. The enlarged kidneys can often be palpated through the abdominal wall, and in severe cases, the outline of the kidneys may be visible beneath the skin. Additionally, PKD patients frequently develop high blood pressure, which can manifest as facial flushing, headaches, and visible blood vessels in the eyes. As the cysts continue to grow and multiply, they may cause visible bruising or tenderness in the flank area due to cyst rupture or bleeding. The condition also commonly affects the liver, leading to hepatic cysts that can cause additional abdominal enlargement and a feeling of fullness. Over time, the combination of kidney and liver involvement creates a distinctive body habitus that experienced clinicians can often recognize on sight.
3. Glomerulonephritis - The Inflammatory Response
Glomerulonephritis, an inflammatory condition affecting the kidney's filtering units called glomeruli, produces a constellation of visible symptoms that can develop rapidly or gradually depending on the underlying cause and severity of inflammation. One of the most characteristic and alarming visible signs is hematuria, or blood in the urine, which can range from microscopic amounts detectable only through testing to gross hematuria that turns the urine pink, red, or cola-colored. This dramatic change in urine appearance often serves as the first visible indicator that prompts patients to seek medical attention. Accompanying the hematuria, patients frequently develop proteinuria, which manifests as persistently foamy or frothy urine due to the presence of excess protein, particularly albumin, that normally should not pass through healthy glomerular filters. The loss of protein leads to hypoalbuminemia, resulting in characteristic edema that typically begins around the eyes and face, giving patients a puffy, swollen appearance that is particularly noticeable upon waking. This facial edema, combined with the pallor that develops due to associated anemia, creates a distinctive appearance often described as "nephritic facies." As the condition progresses, the edema extends to the extremities, and patients may develop ascites or pleural effusions in severe cases. The inflammatory process can also cause visible changes in blood pressure, leading to retinal changes visible during eye examinations, including hemorrhages, exudates, and papilledema in cases of severe hypertension.
4. Nephrotic Syndrome - The Protein-Losing Catastrophe

Nephrotic syndrome represents a complex kidney disorder characterized by massive protein loss through the urine, resulting in some of the most dramatic and recognizable visible symptoms in nephrology. The hallmark visible manifestation is severe edema that follows a characteristic pattern, beginning with periorbital swelling that gives patients a distinctly puffy appearance around the eyes, particularly noticeable in the morning hours. This facial edema is often so pronounced that it can significantly alter a person's appearance, making them appear as though they have been crying or have suffered facial trauma. As the condition progresses, the edema becomes generalized, affecting the entire body in a condition called anasarca, where patients develop massive swelling of the legs, abdomen, and even the genital area. The skin becomes stretched and shiny due to the excessive fluid accumulation, and patients may develop visible stretch marks or skin breakdown in severely affected areas. Another striking visible feature is the development of ascites, causing significant abdominal distension that can make patients appear pregnant regardless of their gender or actual pregnancy status. The massive protein loss also leads to muscle wasting, creating a paradoxical appearance where patients simultaneously appear swollen due to edema yet undernourished due to protein depletion. Additionally, the urine becomes notably foamy and frothy due to the high protein content, often described as resembling beaten egg whites or soap suds, a visual cue that many patients notice and find alarming.
5. Kidney Stones - The Crystalline Agony
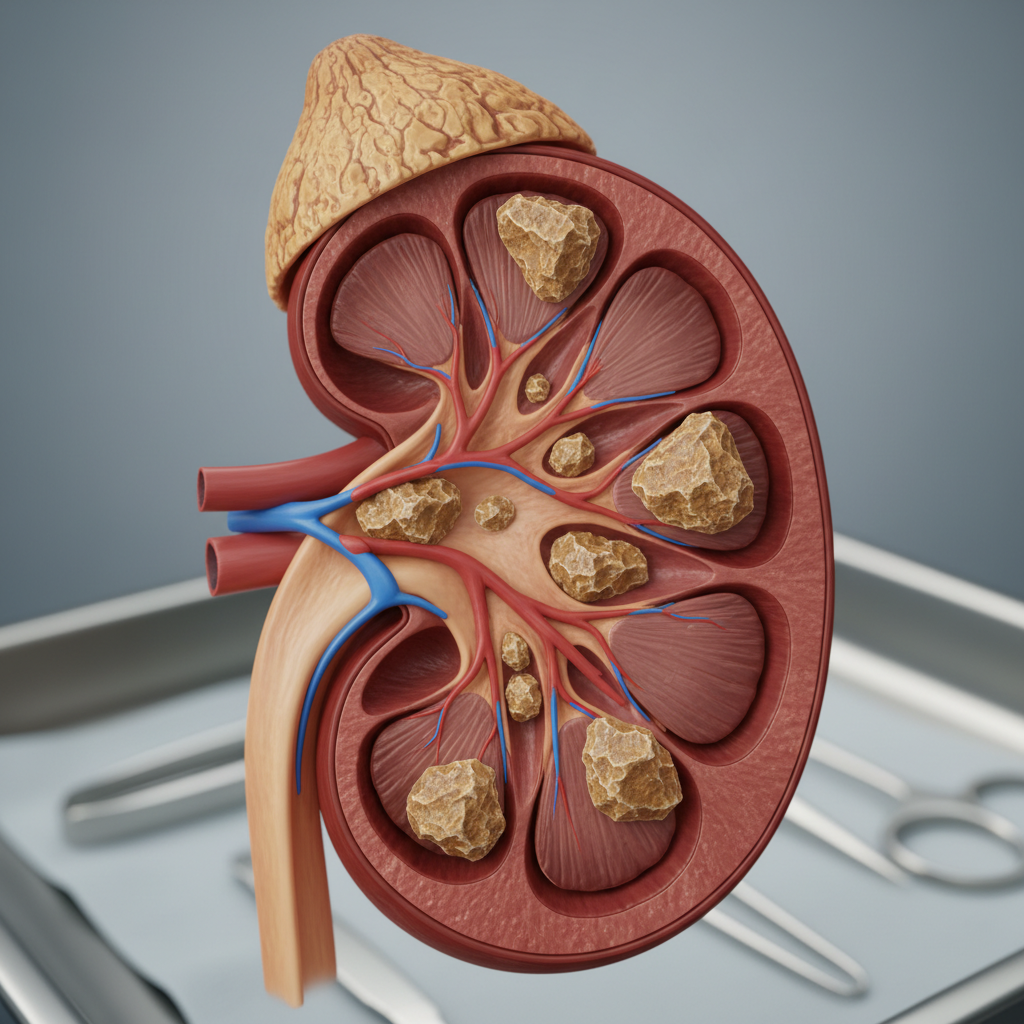
Kidney stones, or nephrolithiasis, create visible symptoms that can range from subtle urinary changes to dramatic manifestations of severe pain and complications. While the stones themselves are typically not visible externally unless they pass and are collected, their presence and movement through the urinary tract produce several observable signs that patients and healthcare providers can readily identify. The most immediate visible symptom is often changes in urine appearance, including hematuria that can range from pink-tinged urine to frank blood, creating a striking visual indicator of stone-related trauma to the urinary tract. The urine may also appear cloudy or contain visible sediment, particularly when stones are actively moving or when secondary infections develop. During acute stone episodes, patients often exhibit visible signs of severe distress, including restlessness, inability to find a comfortable position, profuse sweating, and obvious pain behaviors such as writhing or assuming unusual postures to minimize discomfort. The pain can be so severe that it causes visible nausea and vomiting, leading to signs of dehydration including dry mucous membranes, decreased skin elasticity, and sunken eyes. In cases where stones cause urinary obstruction, patients may develop visible flank swelling due to hydronephrosis, where the kidney becomes enlarged due to backed-up urine. Chronic stone formers may also develop visible scarring or discoloration in the flank area from repeated episodes, and some patients exhibit behavioral changes, becoming visibly anxious about fluid intake or dietary choices due to fear of stone recurrence.
6. Acute Kidney Injury - The Sudden Shutdown
Acute Kidney Injury (AKI) represents a rapid decline in kidney function that can develop over hours to days, producing visible symptoms that often serve as critical warning signs requiring immediate medical intervention. Unlike chronic conditions that develop gradually, AKI can cause dramatic and rapidly evolving visible changes that reflect the sudden inability of the kidneys to maintain proper fluid and electrolyte balance. One of the most noticeable early signs is oliguria, a significant decrease in urine output that patients or caregivers can easily observe and measure. Conversely, some patients may develop polyuria with very dilute urine as the kidneys lose their concentrating ability. The rapid fluid retention characteristic of AKI leads to quickly developing edema, particularly in dependent areas such as the ankles and lower legs, but can also cause facial puffiness and swelling around the eyes. This edema often develops much more rapidly than in chronic kidney disease, sometimes becoming noticeable within 24-48 hours. Patients frequently exhibit visible signs of uremia as waste products accumulate, including a characteristic uremic frost on the skin in severe cases, where crystallized urea appears as a white, powdery substance on the skin surface. The rapid accumulation of toxins can also cause visible confusion, altered mental status, and in severe cases, seizures or coma. Additionally, AKI patients often develop visible signs of metabolic acidosis, including rapid, deep breathing patterns known as Kussmaul respirations, as the body attempts to compensate for acid-base imbalances.
7. Diabetic Nephropathy - The Sweet Destruction

Diabetic nephropathy, a leading cause of kidney failure worldwide, develops as a complication of diabetes mellitus and produces a progressive array of visible symptoms that reflect the gradual destruction of kidney function by chronically elevated blood glucose levels. The earliest visible sign is often the development of proteinuria, which manifests as persistently foamy or frothy urine that patients may notice during routine bathroom visits. This protein loss gradually leads to the development of edema, which in diabetic nephropathy typically follows a characteristic pattern, beginning with subtle swelling around the ankles and feet that gradually progresses upward to involve the legs, abdomen, and eventually the face and hands. The edema associated with diabetic nephropathy can be particularly problematic because it often occurs in conjunction with diabetic peripheral vascular disease, leading to poor wound healing and visible skin changes including discoloration, ulcerations, and infections. Patients may also develop visible signs of diabetic retinopathy concurrently, as both conditions share similar pathophysiological mechanisms, with eye examinations revealing characteristic changes that mirror the kidney damage occurring simultaneously. As the condition progresses, patients often exhibit the classic signs of chronic kidney disease, including pallor due to anemia, as the failing kidneys produce insufficient erythropoietin. The combination of diabetes and kidney disease also frequently leads to visible complications such as poor wound healing, recurrent infections, and characteristic diabetic skin changes including diabetic dermopathy, which appears as light brown, scaly patches typically found on the shins.
8. Hypertensive Nephrosclerosis - The Pressure Cooker Effect
Hypertensive nephrosclerosis, also known as hypertensive kidney disease, results from chronic high blood pressure that gradually damages the small blood vessels within the kidneys, creating visible symptoms that reflect both the underlying hypertension and the resulting kidney dysfunction. The condition develops insidiously over years, with visible symptoms often appearing only after significant kidney damage has occurred. One of the most characteristic visible manifestations is the development of retinal changes that can be observed during ophthalmoscopic examinations, including arteriovenous nicking, flame-shaped hemorrhages, cotton wool spots, and in severe cases, papilledema. These retinal changes often parallel the degree of kidney damage and serve as visible markers of the systemic vascular damage occurring throughout the body. Patients frequently develop the classic signs of chronic kidney disease as their kidney function declines, including progressive edema that typically begins in the lower extremities and gradually ascends to involve the face and hands. The edema associated with hypertensive nephrosclerosis is often accompanied by visible signs of left ventricular hypertrophy, including a displaced and enlarged cardiac impulse that may be visible on chest inspection. As the condition progresses, patients may exhibit visible signs of uremia, including a characteristic sallow complexion, uremic frost in severe cases, and changes in mental status that can be observed as confusion or altered behavior. The chronic nature of hypertensive nephrosclerosis also leads to visible complications such as accelerated atherosclerosis, which may manifest as visible vascular changes, claudication, or other signs of peripheral vascular disease.
9. Lupus Nephritis - The Autoimmune Assault

Lupus nephritis, a serious complication of systemic lupus erythematosus (SLE), produces distinctive visible symptoms that combine the characteristic features of autoimmune disease with specific kidney-related manifestations. The condition occurs when the immune system attacks the kidneys as part of the broader autoimmune process, creating a unique constellation of visible signs that can help healthcare providers recognize and monitor the disease. One of the most characteristic visible features is the combination of the classic lupus rash, particularly the butterfly rash across the cheeks and nose, with concurrent signs of kidney involvement such as edema and changes in urine appearance. Patients often develop the nephritic or nephrotic syndrome features, including significant facial edema that can be particularly pronounced around the eyes, giving patients a characteristic puffy appearance that is often more severe in the morning. The urine frequently shows visible changes, including hematuria that can range from microscopic to gross blood, creating pink, red, or tea-colored urine, and proteinuria that manifests as persistently foamy urine. The autoimmune nature of lupus nephritis also produces visible systemic symptoms including joint swelling and deformity, skin rashes and photosensitivity reactions, hair loss, and oral ulcers. As the kidney involvement progresses, patients may develop severe hypertension with visible retinal changes, and in advanced cases, signs of uremia including altered mental status, uremic frost, and the characteristic uremic fetor (a urine-like odor on the breath). The fluctuating nature of lupus can cause these visible symptoms to wax and wane, making recognition and monitoring particularly challenging but critically important for optimal management.
10. Alport Syndrome - The Hereditary Harbinger

Alport syndrome, a hereditary nephritis caused by mutations in genes encoding type IV collagen, produces a unique combination of visible symptoms that affect multiple organ systems, making it one of the most recognizable genetic kidney diseases when all features are present. The condition is characterized by a classic triad of progressive kidney disease, sensorineural hearing loss, and ocular abnormalities, each contributing distinct visible or observable features that aid in diagnosis. The kidney involvement typically manifests early with persistent hematuria, often visible as pink or red-tinged urine that may be noticed by parents in affected children or by patients themselves as they reach adolescence. Unlike many other forms of kidney disease, the hematuria in Alport syndrome is often constant rather than episodic, providing a consistent visible marker of the ongoing kidney damage. As the condition progresses, patients develop the typical signs of chronic kidney disease, including edema, pallor, and growth retardation in children, which can be readily observed by family members and healthcare providers. The ocular manifestations include characteristic changes visible during ophthalmologic examination, such as anterior cone-shaped cataracts and retinal changes, while the hearing loss, though not directly visible, often becomes apparent through behavioral changes and communication difficulties. Male patients with X-linked Alport syndrome typically show more severe and earlier visible symptoms compared to females, reflecting the genetic inheritance pattern. The progressive nature of the disease means that visible symptoms gradually worsen over time, with many patients eventually requiring visible signs of renal replacement therapy, such as arteriovenous fistulas for dialysis access or the physical changes associated with immunosuppressive medications following kidney transplantation.
11. Recognizing the Visual Language of Kidney Disease

The journey through these ten kidney conditions reveals the remarkable ways in which our bodies communicate distress through visible symptoms, transforming the often-silent progression of kidney disease into observable warning signs that demand attention and action. From the subtle morning puffiness that may herald the onset of glomerulonephritis to the dramatic abdominal distension characteristic of polycystic kidney disease, each condition presents its own unique visual signature that, when properly recognized and interpreted, can lead to earlier diagnosis and more effective treatment. The importance of understanding these visible manifestations cannot be overstated, as kidney disease often progresses silently until significant damage has occurred, making these observable symptoms crucial windows of opportunity for intervention. Healthcare providers and patients alike must develop a keen awareness of these visual cues, understanding that changes in urine appearance, the development of edema, alterations in skin color or texture, and systemic signs of illness may all represent the kidneys' desperate attempts to signal their declining function. The interconnected nature of kidney function with other body systems means that visible symptoms often extend far beyond the urinary tract, affecting cardiovascular health, bone metabolism, blood formation, and overall appearance in ways that create recognizable patterns for those trained to see them. As we advance in our understanding of kidney disease and develop new therapeutic approaches, the ability to recognize these visible symptoms early remains one of our most powerful tools for preserving kidney function and improving patient outcomes. The message is clear: our bodies speak to us through visible symptoms, and in the case of kidney disease, learning to understand this visual language can literally be a matter of life and death, making awareness and education about these observable signs an essential component of preventive healthcare and early intervention strategies.